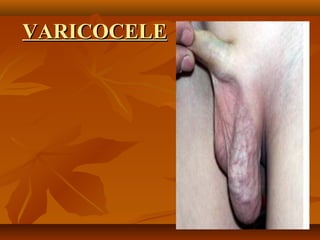
Varicocele
- 1. VARICOCELE
- 2. NORMAL ANATOMYOF PAMPINIFORM PLEXUS Union of multiple spermatic veins frm back of testis and epididymis. Ascend along cord infront of the ductus deferens below the superficial inguinal ring.They unite to form 3-4 veins--inguinal canal—enter abdo thru deep ring--forms 2 veins which unite—testicular vein-- IVC—acute. Drain from testes,epididymis and vas deferens-drain into spermatic veins Left spermatic vein drains into renal vein and right spermatic into inferior vena cava and then into the rt renal vein.
- 4. What is varicocele? Dilatation and tortuosity of the pampiniform plexus and so also of the testicular veins. Seen commonly in men aged 15-30yrs and rarely after 40yrs. Occur in 15-20% of all males and 40% of all infertile males. Normal small vessels of plexus- 0.5-1.5mm. Diameter greater than 2mm- Varicocele.
- 5. Seen commonly on the left side –5 reasons. -longer -enters at right angle to the renal vein -left testicular artery arching over it -a loaded sigmoid colon. - compressed b/w the aorta and SMA.
- 6. Aetiology and types 1.IDIOPATHIC/PRIMARY – due to incompetency of valves. 98% occur on the left side. 2.SECONDARY- pelvic or abdominal mass. - L renal cell carcinoma with tumor thrombus in left vein. -Nutcracker syndrome- SMA compressing left vein. Common conditions- RCC, Retroperitoneal fibrosis or adhesions.
- 7. CLINICAL FEATURES Swelling Dragging /aching pain in the groin and scrotum “ bag of worms” feeling Scrotum on the affected side hangs down. On lying down,it gets reduced. Bow sign- hold varicocele b/w thumb and fingers,patient is asked to bow-reduced in size.
- 8. Cough impulse present Long standing cases- affected side testis is reduced in size and softer. Fertility problems.
- 9. Varicocele and subfertility Altered heat exchange mechanism due to stagnation- hyperthermia-inhibition of spermatogenesis. Increased temperature-increased metabolic activity-depletion of glycogen storage-injury of parenchyma of testis-oligospermia. Hypoxia, Leydig cell dysfunction-low testosterone. Maturation arrest-poor spermatogenesis.
- 10. INVESTIGATIONS Venous doppler of the scrotum and groin- -standing/ valsalva’s manouevre. U/S abdomen to look for kidney tumours. Semen analysis
- 13. GRADING 1.SMALL - identified only by bearing down i.e, an increase in abdominal pressure. 2.MODERATE - identified by palpation w/o bearing down. 3.LARGE - easily identifed by inspection alone. 4.SEVERELY TORTUOUS.
- 14. INDICATIONS FOR SURGERY American Urological Society recommends that varicocele treatment should be offered to the male partner of a couple attempting to conceive when all of the following are present. A varicocele is palpable. The couple has documented infertility. The female has normal fertility or potentially correctable infertility. The male partner has one or more abnormal semen parameters or sperm function test results.
- 15. The indications in adolescents- presence of significant testicular asymmetry (>20%) demonstrated on serial examinations, testicular pain, and abnormal semen analysis results. Very large varicoceles may also be repaired; however, in the absence of atrophy, this indication is relative and controversial .
- 16. TREATMENT 3 SURGICAL AND 1 NON SURGICAL PROCEDURE. VARICOCELECTOMY- The most common approaches are inguinal (groin)-easier and safer. retroperitoneal (abdominal) infrainguinal/subinguinal (below the groin), suprainguinal extraperitonial( Palomo’s operation), Scrotal approach- grade 4.
- 17. Done in GA or spinal. 2-3 inch incision. Ligate the offending veins. Avoid strenuous exercise for several days after surgery. Apply scrotal support.
- 18. Complications 20% chance of recurrence. 5% chance of hydrocele Damage to testicular artery. Infection. hematoma
- 19. 2. MICRODISSECTION Microsurgery (also called microsurgical ligation) smaller incision is made. Cut the skin and fatty tissue. Because muscle is not cut-less pain and faster recovery. The doctor identifies the varicoceles (swollen veins) through an operating microscope. Large varicoceles are cut and stapled closed. Smaller varicoceles are cut and stitched shut. Takes less than an hour and recovery time is short. Higher success rate,fewer complications,smaller scar.
- 20. 3.LAPROSCOPY Similar to conventional surgery. Incision made on abdomen. High ligations required. Larger incision or more retraction needed. Complications more- testicular artery injuryy and hydrocele.
- 21. IV. Coil Embolization, Radiologic Balloon Occlusion or Radiologic Ablation Non-surgical procedure. Steel coil or silicone balloon catheter is introduced into a vein below the groin through a nick in the skin. Passed under X-ray guidance. Tiny metal coils or other embolizing agents introduced through the catheter.
- 22. No stitches needed. Patient can go back in 24hrs. Lower rates of complications. Disadv- less effective, higher recurrence(5- 11%), danger that the coil could migrate to the heart and cause death .
- 25. CONTRAINDICATIONS Subclinical varicocele in an infertile person- controversial. discovery of a varicocele at the time of vasectomy or vasectomy reversal-relative contraindication to immediate repair. A 6-month delayed repair is recommended -to allow the development of collateral vessels to decrease the chance of vascular compromise to the testicle.
