040044947
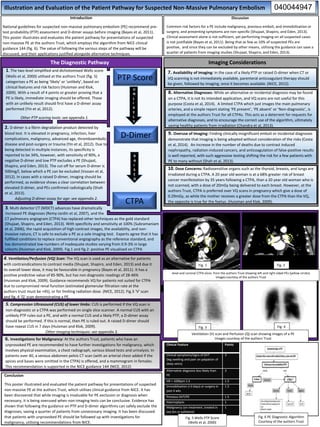
- 1. Illustration and Evaluation of the Patient Pathway for Suspected Non-Massive Pulmonary Embolism Introduction National guidelines for suspected non-massive pulmonary embolism (PE) recommend pre- test probability (PTP) assessment and D-dimer assays before imaging (Bayes et al, 2011). This poster illustrates and evaluates the patient pathway for presentations of suspected non-massive PE at the authors Trust, which employs the algorithm from NICE clinical guidance 144 (fig. 6). The value of following the various steps of the pathway will be discussed, and their applications justified alongside alternative techniques. Discussion Common risk factors for a PE include malignancy, previous emboli, and immobilisation or surgery, and presenting symptoms are non-specific (Shujaat, Shapiro, and Eden, 2013). Clinical assessment alone is not sufficient, yet performing imaging on all suspected cases is not justifiable (Bayes et al, 2011). Being that as few as 10% of suspected PEs are positive, and since they can be excluded by other means, utilising the guidance can save a quarter of patients from imaging studies (Shujaat, Shapiro, and Eden, 2013). CT pulmonary angiogram (CTPA) has replaced other techniques as the gold standard (Shujaat, Shapiro, and Eden, 2013). With specificity and sensitivity at 100% (Subramaniam et al, 2006), the rapid acquisition of high contrast images, the availability, and non- invasive nature, CT is safe to exclude a PE as a sole imaging test. Experts agree that it has fulfilled conditions to replace conventional angiography as the reference standard, and has demonstrated low numbers of inadequate studies varying from 0.9-3% in large cohorts (Huisman and Klok, 2009). Fig.1 and fig.2: positive PE visualised on CTPA 3. Multi detector CT (MDCT) advances have dramatically increased PE diagnoses (Remy-Jardin et al, 2007), and the PTP Score D-Dimer CTPA 1. The two level simplified and dichotomised Wells score (Wells et al, 2000) utilised at the authors Trust (fig. 5) categorises a PE as being ‘likely’ or ‘unlikely’, based on clinical features and risk factors (Huisman and Klok, 2009). With a result of 4 points or greater proving that a PE is likely, immediate imaging should be offered. Those with an unlikely result should first have a D-dimer assay performed (Yin et al, 2012). Other PTP scoring tools: see appendix 1. 2. D-dimer is a fibrin degradation product detected by blood test. It is elevated in pregnancy, infection, liver complications, malignancy, advanced age, thromboembolic disease and post-surgery or trauma (Yin et al, 2012). Due to being detected in multiple instances, its specificity is reported to be 34%, however, with sensitivity of 90%, a negative D-dimer and low PTP excludes a PE (Shujaat, Shapiro, and Eden, 2013). The cut off for serum D-dimer is 500mg/l, below which a PE can be excluded (Vossen et al, 2012). In cases with a raised D-dimer, imaging should be performed, as evidence shows a clear correlation between elevated D-dimer, and PEs confirmed radiologically (Shah et al, 2013). Adjusting D-dimer assay for age: see appendix 2. The Diagnostic Pathway Imaging Considerations 7. Availability of Imaging: In the case of a likely PTP or raised D-dimer when CT or VQ scanning is not immediately available, parenteral anticoagulant therapy should be given, followed by imaging, once it becomes available. (NICE, 2012). 9. Overuse of Imaging: Finding clinically insignificant emboli or incidental diagnoses demonstrate that imaging is being adopted without consideration of the risks (Costa et al, 2014). An increase in the number of deaths due to contrast induced nephropathy, radiation-induced cancers, and anticoagulation of false-positive results is well reported, with such aggressive testing shifting the risk for a few patients with PE to many without (Shah et al, 2013). 8. Alternative Diagnoses: While an alternative or incidental diagnosis may be found on a CTPA, it is not its intended application, and VQ scans are not useful for this purpose (Costa et al, 2014). A limited CTPA which just images the main pulmonary arteries, and a simple report stating ‘PE present’, ‘PE absent’ or ‘Non-diagnostic’, is employed at the authors Trust for all CTPAs. This acts as a deterrent for requests for alternative diagnoses, and to encourage the correct use of the algorithm, ultimately saving healthy patients from irradiation (Chandra et al, 2013). 10. Dose Concerns: Radiosensitive organs such as the thyroid, breasts, and lungs are irradiated during a CTPA. A 20 year old woman is at a 68% greater risk of breast cancer manifestation by 35 years following a CTPA, than a 20 year old woman who is not scanned, with a dose of 20mGy being delivered to each breast. However, at the authors Trust, CTPA is preferred over VQ scans in pregnancy which give a dose of 0.29mGy, as while the mother receives a greater dose from the CTPA than the VQ, the opposite is true for the foetus. (Huisman and Klok, 2009). 4. Ventilation/Perfusion (VQ) Scan: The VQ scan is used as an alternative for patients with contraindications to contrast media (Shujaat, Shapiro, and Eden, 2013) and due it its overall lower dose, it may be favourable in pregnancy (Bayes et al, 2011). It has a positive predictive value of 85-90%, but has non diagnostic readings of 28-46% (Huisman and Klok, 2009). Guidance recommends VQ for patients not suited for CTPA due to compromised renal function (estimated glomerular filtration rate at the authors trust must be >45), or for limiting radiation dose. (NICE, 2012). Fig.3 ‘V’ scan and fig. 4 ‘Q’ scan demonstrating a PE. 5. Compression Ultrasound (CUS) of lower limbs: CUS is performed if the VQ scan is non-diagnostic or a CTPA was performed on single slice scanner. A normal CUS with an unlikely PTP rules out a PE, and with a normal CUS and a likely PTP, a D-dimer assay should be performed. If this is normal, then PE is ruled out. A raised D-dimer should have repeat CUS in 7 days (Huisman and Klok, 2009). Other imaging techniques: see appendix 3. 6. Investigations for Malignancy: At the authors Trust, patients who have an unprovoked PE are recommended to have further investigations for malignancy, which involves physical examination, a chest radiograph, various blood tests and urinalysis. In patients over 40, a venous abdomen pelvis CT scan (with an arterial chest added if the apices and bases were omitted in the CTPA) is offered, and a mammogram in females. This recommendation is supported in the NICE guidance 144 (NICE, 2012) Clinical Feature Points Clinical symptoms/signs of DVT (leg swelling and pain on palpation of deep veins) 3 Alternative diagnosis less likely than PE 3 HR > 100bpm 1.5 1.5 Immobilisation (>3 days) or surgery in past 4 wks 1.5 Previous DVT/PE 1.5 Haemoptysis 1 Malignancy (on treatment, treated in last 6m or palliative) 1 Conclusion This poster illustrated and evaluated the patient pathway for presentations of suspected non-massive PE at the authors Trust, which utilises clinical guidance from NICE. It has been discovered that while imaging is invaluable for PE exclusion or diagnosis when necessary, it is being overused when non-imaging tests can be conclusive. Evidence has shown that following the guidance on PTP and D-dimer algorithms can safely exclude the diagnoses, saving a quarter of patients from unnecessary imaging. It has been discussed that patients with unprovoked PE should be followed up with investigations for malignancy, utilising recommendations from NICE. Fig. 1 Fig. 2 Fig. 3 Fig. 4 Fig. 5 Wells PTP Score (Wells et al, 2000) Axial and coronal CTPA slices from the authors Trust showing left and right sided PEs (yellow circles) Images courtesy of the authors Trust Ventilation (V) scan and Perfusion (Q) scan showing images of a PE Images courtesy of the authors Trust Fig. 6 PE Diagnostic Algorithm Courtesy of the authors Trust 040044947 U N L I K E L Y R A I S E D
- 2. References Bayes, H.K., O'Dowd, C.A., Glassford, N.J., McKay, A. & Davidson, S. 2011, "D-dimer assays - a help or hindrance in suspected pulmonary thromboembolism assessment?” Journal of postgraduate medicine, vol. 57, no. 2, pp. 109-114. Chandra, S., Sarkar, P.K., Chandra, D., Ginsberg, N.E. & Cohen, R.I. 2013, "Finding an alternative diagnosis does not justify increased use of CT-pulmonary angiography", BMC Pulmonary Medicine, vol. 13, pp. 9-9. Costa, A., Basseri, H., Sheikh, A., Stiell, I. & Dennie, C. 2014, "The yield of CT pulmonary angiograms to exclude acute pulmonary embolism", Emergency Radiology, vol. 21, no. 2, pp. 133-141. Huisman, M.V. & Klok, F.A. 2009, "Diagnostic management of clinically suspected acute pulmonary embolism", Journal of Thrombosis & Haemostasis, vol. 7, pp. 312-317. National Clinical Guideline Centre 2012, "Venous thromboembolic diseases: the management of venous thromboembolic diseases and the role of thrombophilia testing. Clinical Guideline Methods, evidence and recommendations", National Institute for Health and Clinical Excellence. Remy-Jardin, M., Pistolesi, M., Goodman, L.R., Gefter, W.B., Gottschalk, A., Mayo, J.R. & Sostman, H.D. 2007, "Management of suspected acute pulmonary embolism in the era of CT angiography: a statement from the Fleischner Society", Radiology, vol. 245, no. 2, pp. 315-329. Shah, K., Quaas, J., Rolston, D., Bansal, S., Bania, T., Newman, D., Wiener, D. & Lee, J. 2013, "Magnitude of D-dimer matters for diagnosing pulmonary embolus", The American Journal of Emergency Medicine, vol. 31, no. 6, pp. 942-945. Shujaat, A., Shapiro, J.M. & Eden, E. 2013, "Utilization of CT pulmonary angiography in suspected pulmonary embolism in a major urban emergency department", Pulmonary Medicine, , pp. 1-6. Subramaniam, R.M., Chou, T., Swarbrick, M. & Karalus, N. 2006, "Pulmonary embolism: accuracy and safety of a negative CT pulmonary angiogram and value of a negative D-dimer assay to exclude CT pulmonary angiogram-detectable pulmonary embolism", Australasian Radiology, vol. 50, no. 5, pp. 424-428. Vossen, J.A., Albrektson, J., Sensarma, A. & Williams, S.C. 2012, "Clinical usefulness of adjusted D-dimer cut-off values to exclude pulmonary embolism in a community hospital emergency department patient population", Acta radiologica, vol. 53, no. 7, pp. 765- 768. Wells PS, Anderson DR, Rodger M, Ginsberg JS, Kearon C, Gent M et al. Derivation of a simple clinical model to categorize patients probability of pulmonary embolism: increasing the models utility with the SimpliRED D-dimer. Thrombosis & Haemostasis. 2000; 83(3):416-420. Yin, F., Wilson, T., Della Fave, A., Larsen, M., Yoon, J., Nugusie, B., Freeland, H. & Chow, R.D. 2012, "Inappropriate use of D-dimer assay and pulmonary CT angiography in the evaluation of suspected acute pulmonary embolism", American Journal of Medical Quality, vol. 27, no. 1, pp. 74-79. Bounameaux, H. 2010, "Contemporary management of pulmonary embolism: the answers to ten questions", Journal of internal medicine, vol. 268, no. 3, pp. 218-231. Bowman, A.W., Johns, G.S. & Karstaedt, N. 2011, "Markedly elevated plasma D-dimer and the prevalence of acute pulmonary embolus", Acta Medica Academica, vol. 40, no. 2, pp. 152-158. Bibliography
- 3. Appendices: Appendix 2: Adjusting D-dimer for age Typically, the cut off value for serum D-dimer is 500 mg/L, below which the diagnosis of PE can be ruled out. However one study concluded that this could be increased to 1000 mg/L without affecting its sensitivity, safely eliminating the diagnosis in more patients, and further reducing the use of imaging (Bowman, Johns and Karstaedt, 2011). A PE is more likely to occur in the elderly, and multiple comorbidities associated with aging can mimic a PE clinically. Hence, the argument exists regarding the usefulness of this value for the elderly, with evidence showing that a PE may be excluded in as few as 5% of patients over 80, compared with 60% in those under 40, using this D-dimer value (Bounameaux, 2010). Appendix 1: Other PTP scoring tools “Geneva score (original and revised) - The original Geneva score is based on seven clinical factors and required interpretation of the findings on chest X-ray and arterial blood gases. The revised Geneva score covers eight parameters in 3 clinical areas: risk factors, symptoms and clinical signs. Each of these is given 1 to 5 points accordingly. This gives a possible score range of 0 to 25. A score of 11 or higher is classified as ‘high risk’ of PE; a score of 4 to 10 as ‘intermediate risk’ and a score of 0 to 3 as ‘low risk’. Charlotte rule - Patients with suspected PE (based on empiric clinical assessment) are stratified into low-risk and high-risk (pre-test probability groups). Patients are classified as high risk if they have at least two of the following: • Age greater than 50 • Heart rate greater than systolic blood pressure • Surgery in the past month • Unilateral leg swelling • Haemoptysis • Unexplained oxygen saturation less than 95% on room air.” (National Clinical Guideline Centre 2012, p 69.) Appendix 3: Other imaging techniques Pulmonary Angiogram (PA) The PA was the traditional gold standard (Yin et al, 2012) reference imaging method (Huisman and Klok, 2009). However it is Invasive and resource demanding and no longer routinely performed (Bounameaux, 2010). Magnetic Resonance Angiography (MRA) MRA has potential as an alternative for those unsuited to iodinated CM (Huisman and Klok, 2009), due to shortened acquisition times and improved spatial resolution. Combined perfusion and non-contrast/contrast scans have a specificity of 93% (Remy-Jardin et al, 2007), however, 25% of scans are inadequate (Bounameaux, 2010).