Rakai Data Mart
- 2. Rakai Health Sciences Program - Initiated by Ugandan colleagues (Drs. D Serwadda and N Sewankambo) in 1987 - Researchers at: - Makerere University - Uganda Virus Research Institute - Johns Hopkins - Columbia University, Karolinska, University of Toronto, University College London, etc… - NIH/NIAID (International Center for Excellence in Research) - Registered independent legal entity in Uganda - ~ 350 Ugandan colleagues and staff
- 3. Rakai Community Cohort Study: core of the RHSP Observational research (Quantitive / Qualitative) - Community demography - HIV epi/dynamics and spacial dynamics - HIV/STI risk factors (biological and behavioral) - Use of services - STIs, OIs, malaria, NCD - Social (Intimate partner violence, alcohol…) - Time trends …. And much more Randomized Trials -STD control for HIV prevention& pregnancy outcomes - Male circ for HIVI prevention in men - Male circ for HIV prevention in women partners - HSV-2 suppression for HIV progression - Prevention of IPV and HIV (SHARE trial) -Trial of demand generation (Stylish Man & Woman) Implementation Science/Operations Research P-MTCT, condoms, VCT, ART/HIV care provision, male circumcision, family planning, adolescent health, prevention of intimate partner violence Methods of improving service uptake and adherence (peer programs, communication technologies) Service provision -Combined HIV prevention, HIV/STI care and treatment, family planning, some general health care Basic science (with an epi flavor) - Mucosal immunology, microbiology, pathology, immunohistochemistry, HSV-2, drug resistance, HSV-2, HPV Molecular epi - HIV Subtypes, HIV superinfection - HIV phylogentics - ART resistance Clinical studies: HIV related neurological outcomes Liver fibrosis, CVD, kidney disease, etc…
- 4. Presentation of RHSP studies and resources • Kate Grabowski: – Cohort and key nested studies • Aaron Tobian – Lab studies and resources • Larry Chang – Clinical and HIV prevention studies, and implementation science • Maria Wawer – Mop up
- 5. What we hope will come of this presentation • Opportunities for you – Secondary data analyses – New setting for your current research interests and ideas – New research ideas – Grants (!) • Opportunities for RHSP – New research ideas – New collaborations (and grants ) – New expertise (substance abuse research, etc…)
- 6. The Rakai Community Cohort Study: Overview and opportunities for population-based HIV research and beyond in Rakai, Uganda
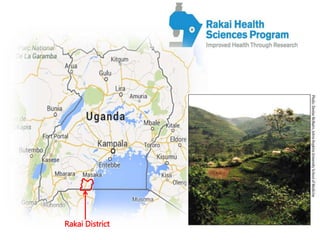
- 7. Rakai Community Cohort Study (RCCS) • Open population-based HIV incidence cohort in 40-50 agricultural, trading, and fishing communities in Rakai District, Uganda • ~15-17,000 study participants are surveyed on an ~annual basis. • Surveys ongoing since 1994. • 16 survey rounds completed • Fish communities surveyed beginning in survey round 15 • N=4 fish landing sites (Dimu and Kansensero) • Each survey includes household census and individual interviews for adults aged 15-49.
- 8. RCCS data overview • Census • Household membership • Family relationships • In/out migration • Deaths and births • GPS • Socio-demographic and behavioral survey • Basic demographics • Relationship history • Egocentric Sexual networks • Family planning • Uptake of prevention interventions • HIV/STI Testing • Biological samples stored • Qualitative data • Focus groups, in-depth interviews Survey Subject Areas Captured 72,962 Total RCCS Subjects Research Data 16 Rounds of Study + Lab Data Over 1,800 Questions 55,664 Households in Census
- 9. Prevalence (%) Incidence (per 100py) General Population 11 0.8 Fish Landing Sites 34 3.2 Table 1. Male HIV prevalence and incidence, 2012-2013 HIV incidence and prevalence in the RCCS Prevalence (%) Incidence (per 100py) General Population 17 1.0 Fish Landing Sites 49 3.7 Table 2. Female HIV prevalence and Incidence, 2012-2013
- 10. Large Spatial heterogeneity in HIV burden
- 11. 0 2 4 6 8 10 12 14 16 18 R1 R2 R3 R4 R6 R7 R8 R9 R10 R11 R12 R13 R14 1.6 0.2 HIVprevalence,% HIVIncidence/100py 1.0 1.4 Longitudinal trends in the RCCS 0.6 1995 2002 2013
- 12. High viral diversity in RCCS communities • High viral diversity. • Subtypes A and D predominate, both heterosexually transmitted. • Incidence declines in both subtypes, but rapid decline in D.
- 13. Nested studies – examples and possibilities • Risk assessment • Evaluation of prevention interventions and service utilization • Male circumcision • Community randomized trials • Mobility and migration analyses • Sexual network studies • High risk populations • Couples analyses • Family planning and health studies • Demographics and household structure • HIV transmission dynamics
- 14. Multidisciplinary research: HIV transmission dynamics in the RCCS Background: The extent to which continued HIV transmission in sub-Saharan Africa is driven by intra-community sexual networks versus viral introductions from outside of communities remains unknown. Methods: Data: RCCS (2008-2009) 46 communities, 11 geographic regions Spatial dependence between HIV cases (n=1,786) 14,594 participants total, HIV prevalence ~ 12% 189 incident cases >8000 geo-located households Genetic relatedness of infecting viruses with respect to spatial location (env, gag genes) Transmission model Attributable fractions from intra-household, intra-community, and extra-community sexual contacts (self-reported locations) Grabowski et al., Plos Med, 20
- 15. Multidisciplinary research: HIV transmission dynamics in the RCCS Grabowski et al., Plos Med, 20 • Household transmission is common. • Strong genetic and spatial clustering in households. • Transmission model: 39% (95% CI: 32-44%) of transmissions occurred within stable household partnerships. • Extra-household HIV acquisition is more common from non-stable partners outside of the local community • High viral diversity and weak spatial clustering at the community scale • 44% of incident cases clustered with another participant in one or both gene regions. • 60% of incident cases that did not cluster with a household partner, clustered exclusively with extra- community participants • Transmission model: 62% (95%CI: 58-66%) infected outside household were infected
- 16. Linkage of disparate community-based HIV epidemics in Rakai • R01 NIAID, Gates Foundation (PANGEA-HIV) • Timeframe: 2014-2018 • What? Elucidation of community sexual network structures and quantification of the extent to which fishing communities drive endemic HIV transmission in Rakai, District • How? RCCS observational data on migration, geography of sexual partnerships, and whole genome HIV sequencing • Opportunities? – Data analysis Ron Gray (PI), Kate Grabowski
- 17. Rakai Lab Studies (Not just an HIV support laboratory) International Collaborators: NIH International Centers of Excellence in Research (ICER) Thomas Quinn Lab Group (NIH/JHU) University of Toronto George Washington University Karolinska Institute
- 18. Randomised Trials Showed Male Circumcision Reduces HIV Infection Rakai, Uganda Gray et. al. (2007) Lancet; 657 – 66 Kisumu, Kenya Bailey et. al. (2007) Lancet; 643 – 56 Orange Farm, South Africa Auvert et. al. (2005) PLoS Med; e298
- 19. Rakai Laboratory Assays • ELISA/Serology – HIV Detection – HIV Incidence – HSV-2 – CMV – HBV – HCV • PCR/Nucleic Acid Testing – HIV Detection – HIV viral load – HSV-2 – HPV – CMV – Malaria • Complete Blood Count • Flow cytometry • Histology processing • Microscopy – Bacterial vaginosis – Malaria • Bacterial culture – Trichomonas vaginalis • 454 Pyrosequencing – HIV-superinfection – Microbiome • Other Infections to be assessed – Dengue? – Influenza?
- 20. Male Circumcision (MC): Why the foreskin is our window to viruses and immunology • 3 male circumcision trials showed the foreskin is the site of entry for 50-60% of HIV • Serum samples, genital swabs and foreskin tissues provide insight into virology, immunology and the microbiome • All studies presented today are from archived samples to give you examples of types of studies that can be performed with the RHSP archive.
- 21. Male Circumcision Reduces HSV-2 Acquisition 0 1 2 3 4 5 6 7 8 9 10 Overall 2+ Sexual Partners Inconsistent condom use Age 20-24 HSV-2Incidence/100py Control Circumcision IRR = 0.72 (0.56-0.96) IRR = 0.48 (0.31-0.73) IRR = 0.47 (0.30-0.73) IRR = 0.55 (0.36-0.84) Tobian et al. NEJM 2009
- 22. Male Circumcision Reduces Human Papillomavirus (HPV) Prevalence in Men Tobian et al. NEJM 2009 0.0 10.0 20.0 30.0 40.0 50.0 60.0 High-risk HPV Non-high-risk HPV All HPV genotypes Multiple high- risk HPV Prevalence(%) Control Intervention PRR = 0.65 (0.45-0.94) PRR = 0.66 (0.49-0.91) PRR = 0.70 (0.53-0.91) PRR = 0.35 (0.17-0.71) 27.9 18.0 26.2 39.4 4.7 13.7 35.6 51.2
- 23. 0 10 20 30 40 50 60 Trichomonas BV Severe BV Prevalence(%) Control Circumcision Male Circumcision Reduces Trichomonas and Bacterial Vaginosis in Female Partners PRR 0.53 CI 0.33 – 0.85 PRR 0.80 CI 0.71 – 0.89 PRR 0.31 CI 0.18 – 0.54 Gray et al. Am J Ob Gyn 2009 11.2 5.9 50.6 40.3 6.5 2.0
- 24. 0.0 10.0 20.0 30.0 40.0 50.0 60.0 All HPV genotypes Low-risk HPV High-risk HPV Prevalence(%) Control Intervention Male Circumcision Reduces HPV Prevalence in Women PRR = 0.82 (0.72-0.92) PRR = 0.77 (0.66-0.91) PRR = 0.71 (0.60-0.85) 56.5 46.1 42.5 32.9 38.6 27.5 Wawer et al. Lancet 2011
- 25. Biological Plausibility CD4+ T Cells Dendritic Cells Tobian et al. J Infect Dis. 2013Redd et al, J Infect Dis. 2011 Foreskins from HSV-2 seropositive men have high frequency of CD4+ T-cells present in submucosa Foreskins from men who have recently cleared HPV have a sig. increase in dendritic cells
- 26. Liu, CM et al MBio 2013 Male Circumcision Reduces Prevalence and Load of Genital Anaerobic BacteriaPro-inflammatory Anaerobic bacteria are reduced by circumcision; Rakai Trial Liu et al Mbio 2013 Species Circumcised Prevalence % Uncircumcised Prevalence % Absolute difference (%) Clostridia 84.4 48.1 -36 Prevotella 90.9 51.9 -39 Finegoldia 79.2 48.1 -31 Dialister 61.0 16.5 -45 Decreased pro-inflammatory anaerobes may reduce HIV target cell recruitment and reduce HIV risk following MC Decreased pro-inflammatory anaerobes may reduce HIV target cell recruitment and reduce the risk of HIV following male circumcision.
- 28. HSV-2 infection associated with increase in CCR5 expression on foreskin CD4 T cells 0 15 30 45 60 p = 0.024ns Blood Foreskin HSV-2 Positive HSV-2 Negative %CCR5+ofCD4Tcells Prodger et al, AIDS, 2012
- 29. HIV Shedding from MC Wounds
- 30. Redd et al, JID, 2012 Diagnostic Criteria for Superinfection Rakai, Uganda Rate of SI (1.4/100py)
- 31. Available Archived Samples • 20 years of consecutive samples among persistently HIV-negative, HIV-positive and HIV-seroconverters • 476,000 samples – 162,000 genital swabs – 314,000 sera • Human cellular DNA – Buffy coat – Vaginal and penile swabs • Largest repository of foreskins in the world
- 32. HIV Implementation Research in Rakai, Uganda: Overview & Opportunities Larry William Chang, MD, MPH Assistant Professor of Medicine, Epidemiology, & International Health Johns Hopkins School of Medicine and Bloomberg School of Public Health
- 33. Overview • Since 2004, RHSP has provided combination HIV prevention (CHP) services as a PEPFAR implementer – pre-antiretroviral therapy (ART) and ART care (with virologic outcomes) – prevention of mother to child HIV transmission (PMTCT) – medical male circumcision (MMC) – HIV counseling and testing (HCT) – condoms and promotion of behavioral change • 2004-2012, most services provided directly through RHSP- run clinics. • Currently, a hybrid, RHSP oversees all government provided HIV services in the entire Rakai District and provides some services directly.
- 34. Evaluating demand generation (stylish man) for HIV/family planning services Rakai • R01 NIAID • Timeframe: 2014-2018 • What? A novel, demand creation approach (mass media + community mobilization) to increasing HIV service and family planning uptake by demedicalizing HIV prevention and care. • How? Community-randomized trial • Opportunities? – Adaptive study design Maria Wawer (PI) et al.
- 35. Male Circumcision • U01 K25 NIAID • What? Determinants and impact of male circumcision uptake, circumcision device safety, task shifting models, infant circumcision, role of women in increasing circumcision uptake. • How? RCCS, Qualitative • Opportunities? – Mixed methods research understanding health seeking behaviors – New behavioral interventions Xiangrong Kong, Ron Gray
- 36. Combination HIV Prevention Evaluation and Treatment Cascades • Funding: Multiple sources • Timeframe: 2000-2017 • What? Impact of combination HIV prevention on HIV incidence, quantification of HIV service cascades over time • How? RCCS, time series analysis • Opportunities – Analytic input, economic evaluation, modeling Everyone. Figure courtesy of Veena Billioux.
- 37. The PeerCARE Study: A Randomized Trial • Timeframe: 2011-2013 • What? A randomized trial on the impact of peer support on pre-ART outcomes (n=442). • Results? Peers improved engagement in care, cotrimoxazole use, and water vessel use. • Opportunities – Secondary data analyses – Psychometric evaluation of behavioral model (sIMB) Larry Chang (PI) et al.
- 38. Mobile Ecological Momentary Assessment & Intervention of Unhealthy Behaviors in Rakai, Uganda • Center for Global Health Award • Timeframe: 2015-2016 • What? Proof-of-concept study on whether we can use smartphones to collect near real-time, geo-located behavioral data (e.g. sex, smoking, alcohol). • How? N~50, 60 days f/u, process indicators, qualitative eval, compare to conventional survey • Opportunities – Similar study in other settings? – Novel analyses? Larry Chang (PI), Kate Grabowski (Co-Investigator/Analyst)
- 39. CHWs, mHealth, and Combination HIV Prevention in a Hotspot: A Randomized Trial • R01 (scored within funding range) • Timeframe: 2015-2019 • What? A randomized trial on the impact of CHWs promoting CHP supported by novel mHealth tools. • How? Household-level randomization in Kasensero, a fishing community on Lake Victoria which qualifies for Treatment as Prevention (TasP). Primary outcomes are CHP coverage evaluated via RCCS. • Opportunities – Nested studies – Economic evaluations Larry Chang (PI) et al.
- 40. Geospatial HIV Implementation Research • Funding Source: None yet • RHSP has collected rich geospatial data on households, health care facilities, community, and geographic features. • The data can be linked to HIV epidemiologic, service utilization, and clinical outcomes offering the opportunity for novel geospatially-informed HIV implementation research. Examples/Opportunities: – Impact of clinic distance and travel time on virologic outcomes of HIV-infected patients on antiretroviral therapy and on MMC uptake – Geospatial analyses of the appropriateness of HIV health facility and service distribution in Rakai, Uganda Larry Chang, Kate Grabowski
- 41. How to start a collaboration • Most important: contact us to chat • Secondary data analyses: short proposal to be shared with US and Ugandan collaborators, indication of funding for data set creation - if needed. • New RCCS module: same as above. • New study: Discussion with US and Ugandan colleagues on study goals and potential design; drafted study aims; ongoing consultation.
- 42. Contact information • Kate Grabowski: mgrabows@jhu.edu (cohort, transmission dynamics, phylogentics) • Aaron Tobian: atobian1@jhmi.edu (lab, virology, immunology) • Larry Chang: lchang8@jhmi.edu (implementation sci, clinical) • Maria Wawer: mwawer1@jhu.edu (a bit of everything) • Ron Gray: rgray4@jhu.edu (a bit of everything) • Xiangrong Kong: xkong4@jhu.edu (biostats, epi, health seeking behaviors) • Tom Quinn: tquinn2@jhmi.edu (lab, virologiy, NIH) • Oliver Laeyendecker: olaeyen1@jhmi.edu (lab, virology, NIH, ) • Andy Redd: aredd2@jhmi.edu (lab, immunology, NIH) • Jessica Prodger: jessiprodger@gmail.com (immunology) • Caitlin Kennedy: caitlinkennedy@jhu.edu (qualitative research) • Ned Sacktor: sacktor@jhmi.edu (neuro-HIV epidemiology) • Nandy Pilgrim npilgrim@popcouncil.org (social science, adolescents) • Lilian Mutesi (Admin): lmutesi1@jhu.edu