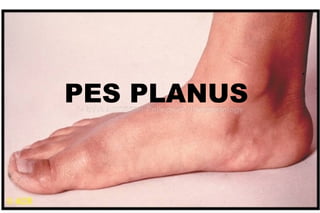
Pes Planus (Flat Foot): Causes, Symptoms, Diagnosis and Treatment
- 1. PES PLANUS
- 2. PES PLANUS (FLAT FOOT) • Medial border of the foot is abnormally in contact with the floor during weight bearing • Low or absent medial longitudinal arch • When associated with deformities of the hind, mid and forefoot – called as pes plano valgus
- 4. JOINTS MOVEMENTS Ankle Plantarflexion and dorsiflexion SUBTALAR (TALOCALCANEAL) inversion and eversion MIDTARSAL adduction and abduction, flexion and extension, supination and pronation
- 5. COMPONENTS OF FLAT FOOT The medial column of the foot appears to be longer than the lateral column Forefoot abduction and supination (relative to hind foot) Talar head displaced medially, anteriorly and downwards Calcaneum everts, dorsiflexes - hindfoot is in valgus Navicular subluxates dorso-laterally, uncovering the talar head
- 6. NORMAL FOOT PES PLANUS
- 7. SECONDARY CHANGES Navicular, cuneiform, cuboid become wedge-shaped, with apex directed dorso-laterally Plantar, spring and deltoid ligaments are stretched Anterior, posterior tibial tendons and plantar muscles are stretched whereas the achilles tendon and peronei become adaptively shortened Calluses develop over the medial bony prominences
- 8. RADIOLOGICAL EXAMINATION 1.Standing anterior-posterior (AP) (dorsoplantar), 2.lateral, and oblique views 3.Harris-Beath views if a tarsal coalition is suspected
- 9. RADIOLOGICAL FEATURES • There are basically 3 components that are involved in producing the alignment abnormalities of symptomatic adult flatfoot: 1.Forefoot abduction 2.Collapse of the longitudinal arch 3.Hindfoot valgus
- 12. a) Talonavicular coverage angle Two lines are drawn, one connecting the edges of the articular surface of the talus, and one connecting the edges of the articular surface of the navicular. The angle formed by these two lines is the talonavicular coverage angle Normally it is less than 7 degrees
- 13. • Lateral subluxation of the navicular on the talus (or talonavicular uncoverage) • This is an indication of forefoot abduction
- 14. b) AP Talar - 1st metatarsal angle Normal talar-1st metatarsal angle on AP view. A line drawn trough the mid-axis of the talus passes through the base of the first metatarsal and is angled laterally in relation to the long axis of the shaft of the metatarsal.
- 15. Abnormal talar-1st metatarsal angle, angled medial to the first metatarsal. It indicates pes planus.(forefoot abduction)
- 16. 2.Collapse of the longitudinal arch
- 17. a) Meary’s angle between long axis of talus and long axis of first metatarsal on a standing lateral X ray long axis of the talus should nearly bisect the navicular and first metatarsal shaft 0 degrees – normal 0 – 15 degrees – mild 15 – 40 degrees – moderate > 40 degrees – severe The location of the sag, talo-navicular, naviculo-cuneiform or both can also be determined
- 18. Normal Meary's angle. The long axis of the talus intersects that of the first metatarsal
- 19. The long axis of the talus is angled plantarward in relation to the first metatarsal, consistent with pes planus
- 20. b) Calcaneal pitch – A line is drawn from the plantar-most surface of the calcaneus to the inferior border of the distal articular surface. The angle made between this line and the transverse plane is the calcaneal pitch Normal 17-32 degrees, in flat foot is decreased May be 0 or negative in case of tightened TA
- 22. Decreased calcaneal pitch indicating pes planus
- 24. a) Lateral Talocalcaneal Angle (Turco’s angle) The normal range is 25-45 degrees
- 25. Increased talocalcaneal angle indicaitng hindfoot valgus in pes planus.
- 26. b) AP Talocalcaneal angle (Kite's angle) This is the angle formed by the intersection of a line bisecting the head and neck of the talus and a line running parallel with the lateral surface of the calcaneus. The range of normal for adults is 15 - 30°
- 27. Abnormally increased AP talocalcaneal angle, more than 30 degrees indicating hindfoot valgus in pes planus.
- 28. 4.CYMA line
- 29. CYMA line is an architectural term designating the union of two curve lines. A normal midtarsal joint should create a smooth cyma between the talonavicular joint and calcaneocuboid joint on both the AP and lateral views
- 30. Normal CYMA line connecting talonavicular joint and calcaneocuboid joint is smooth and continuous.
- 31. • If the cyma line is broken it suggests “shortening” of the calcaneus relative to the talus • This is often just a radiographic shortening possibly due to rotation of the talus on calcaneus (typically seen in a patient with adult flatfoot including loss of the medial arch)
- 32. Broken Cyma line of pes planus.
- 33. HOW COMMON IS FLAT FOOT? One of the most common orthopedic deformities Affects 15 - 20% of adults, mostly asymptomatic Of this 2/3rd have flexible flatfoot , 1/4th have a contracted tendo-achilles associated with a flexible flatfoot and the remainder have rigid flatfoot the most common cause being tarsal coalition
- 34. HOW COMMON IS FLAT FOOT? The medial longitudinal arch normally develops during the first decade of life Therefore flatfeet are usual in infants, common in children and rare in adults Flatfoot in an infant is actually a ‘fat foot’ as the excessive amount of fat obscures the arches
- 35. ANATOMY OF THE ARCHES OF A NORMAL FOOT An arched foot is a distinctive feature of man A) Two longitudinal arches • Medial longitudinal arch • Lateral longitudinal arch B) Transverse arch
- 36. USE OF THE ARCHED FOOT Supports body weight in upright posture Acts as a lever to propel the body forwards in walking, running and jumping Acts as a shock absorber Concavity of the arches protects the soft tissues of the sole against pressure
- 37. FORMATION OF MEDIAL ARCH Ends : Anterior : 1-3 MT heads Posterior : Medial tubercle of calcaneum Summit: Superior articular surface of body of talus Pillars : Anterior: Talus, navicular, 3 cuneiforms, 1-3 MT Posterior: Medial half of calcaneum
- 38. FACTORS RESPONSIBLE FOR MAINTENANCE OF MEDIAL ARCH (as compared to stone bridge) Shape of bones: wedge shaped with apex pointing downwards. The talus acts as a key-stone Intersegmental ties: ligaments and muscles Spring ligament Dorsal ligaments - interosseus talocalcaneal ligament Tendinous extensions of tibialis posterior Tie beams or bow strings : connect two ends of an arch • Medial part of plantar aponeurosis • Medial part of the FDB • Abductor hallucis, FHL, FHB • Medial part of FDL Slings : suspend the arch from above Tibialis posterior, Flexor digitorum longus, Tibialis anterior and peroneus longus Flexor hallucis longus - bulkiest and strongest muscles supporting med arch
- 40. Flat foot classification based on mobility of tarsal joints FLEXIBLE • Physiologic – due to ligamentous laxity in 1st decade • Hypermobile flatfoot – excessive ligamentous laxity – familial, down’s, marfan’s, ehlers-danlos, osteogenesis imperfecta • Bony abnormalities – hypoplasia of sustentaculum tali, hypoplastic calcaneum • Occupational • Obesity RIGID • Congenital • Tarsal coalition • Vertical talus • Acquired • Inflammatory arthrosis, Traumatic arthrosis • Charcot foot • Residua of clubfoot • Contractures of peronei or TA - Rheumatoid arthritis, Gout, Degenerative arthritis, Infection, Acute sprain, Osteochondral fracture, Foot tumors especially osteoid osteoma
- 42. FLEXIBLE FLAT FOOT • MOTOR WEAKNESS – PTTD, accessory navicular, muscular dystrophy, peripheral nerve lesions, cerebral palsy, spinal cord conditions like polio, myelodysplasia, Werdnig – Hoffman disease, spina- bifida • SECONDARY TO ANATOMIC DEFECTS ELSEWHERE : • Ext. rotation of the limb • Genu valgum • Equinus deformity of the ankle (tight tendo- achilles) • Varus deformity of the foot
- 43. FLEXIBLE FLAT FOOT Hereditary condition Marked ligamentous laxity Deformity disappears when feet are freed of weight bearing Weight bearing axis - shifted medial to normal position Prolonged weight bearing in the everted foot - Heel cord contractures ( flexible flatfoot associated with tight heel cord)
- 44. ETIOLOGY No broad consensus Unstable architecture of tarsal bones Congenitally short tendo achilles Weakened muscle power Ligamentous laxity
- 45. HISTORY Age of presentation: adolescence Usually bilateral and asymptomatic Family history of flatfeet and joint hyper mobility Pain, discomfort, burning sensations and fatigue on activity and prolonged standing, cramping at night Felt around the navicular, talocalcaneal joint, below the medial malleolus or at the ant. or post. extremities of the plantar ligaments
- 46. PHYSICAL EXAMINATION Flatfoot only on weight bearing Deformity correctable on tip toe standing Jack’s (great toe extension) test - the arch can be restored by simply dorsiflexing the great toe – suggests that sag is at the naviculocuneiform level
- 47. Arch appearing on tip toe standing
- 48. PHYSICAL EXAMINATION Examine the tendo-achilles for tightness (TA contracture tends to make flexible flatfoot symptomatic) Short tendo-achilles: limited dorsiflexion(not able to walk on heels) Harris and Beath documented that presence or absence of the longitudinal arch did not corelate with the disability and a flatfoot was compatible with normal function unless associated with a tight tendo-achilles Examine ROM of ankle,subtalar, midtarsal joints Examine the gait Generalized ligamentous laxity Hypermobility of the subtalar and mid-tarsal joints: the forefoot can be bent outwards and upwards to an unusual degree
- 49. PHYSICAL EXAMINATION Spine, hips and knees should be examined General examination for neuromuscular abnormalities Don’t forget to examine the shoes shoes show excessive wear along the medial border Pedobarography A record of pressures can be obtained by making the patient to stand and walk on a force plate. Mainly used to compare pre and post operative function
- 50. Footprints made with the aid of an ink pad show the difference between normal sole contact and flat-footed contact. (a) Normal footprint, showing the main contact areas across the anterior metatarsal arch, the lateral border of the foot and the heel, with a ‘hollow’ corresponding to the medial arch. (b) Flat-footed contact, across the sole to the medial side of the foot
- 51. TREATMENT Physiological flexible flatfoot with full ROM is asymptomatic It does not cause pain or disability Xrays are not indicated and treatment is not required Child should be left alone If symptomatic always look for associated causes most commonly tight heel cord
- 52. PARENT EDUCATION AND REASSURANCE Mainstay of treatment as This is what is required in majority Condition is essentially benign Only symptomatic treatment possible No change in ultimate shape of the foot – it is the parents and grand parents who need treatment and not the child
- 54. ORTHOTICS Conservative treatment should always be tried first Arch supports, rubber inserts, Plastizote Whitman valgus brace UCBL (University of California Biomechanics Laboratory) heel inserts Shoe modifications –Thomas heel or a 14 inch wedge on the inner border Custom molded orthotics
- 55. • Medial heel wedge
- 56. LIMITATIONS Do not alter underlying structural fault Do not encourage redevelopment of the arch Running sports shoes have been found to be as effective as traditional orthoses and are more socially acceptable They reduce shoe wear and are said to be more effective in treating shoes rather than feet
- 57. EXERCISES Excercises are designed to improve the strength of invertors and the plantar flexors Toe-walking and multiple toe-ups If tendo-achilles is contracted, stretching it actively and passively is an important form of management Grasping marbles with toes Heel to toe walking Playing in sand Ballet dancing Walking on a supination board There is no scientific study evaluating the effectiveness (or lack of it) of these exercises
- 58. SURGICAL TREATMENT Reserved for patients with intractable symptoms unresponsive to shoe or orthotic modifications and who are unable to modify pain producing activity Limitation of daily activities is an indication for surgery Surgery for flexible flatfoot should not be performed for cosmetic reasons
- 59. SURGICAL OPTIONS Arthrodesing procedures should be delayed until 10 and preferably 15 years Before 10 years arthrodesis is difficult because of excessive cartilaginous component of tarsal bones Subsequent bony growth is retarded Patient must be prepared to accept permanent loss of inversion- eversion motion
- 60. TA LENGTHENING Achilles tendon lengthening is included if the ankle lacks at least 10 degrees of dorsiflexion with the knee extended If patient has severe enough symptoms to warrant surgery, then heel cord lengthening should be part of a comprehensive procedure to reconstruct the arch TECHNIQUE 3 small insicions( 2 medial, 1 lateral) along the length of the tendon Tendon is cut from midline outwards Tendon sheath is repaired to prevent scarring Closure is done with knee extended and ankle dorsiflexed Long leg cast with ankle in neutral is given for 6 weeks
- 62. DURHAM FLATFOOT PLASTY TECHNIQUE Elevation of tibialis posterior tendon Elevation of osteoperiosteal flap from proximal to distal Naviculocuneiform arthrodesis Advancement of osteoperiosteal flap Advancement of tibialis posterior
- 65. POSTERIOR CALCANEAL DISPLACEMENT OSTEOTOMY Displacement of the posterior half of the calcaneus medially Reestablishes the weight bearing line Indicated in cases with excessive heel valgus
- 67. ANTERIOR CALCANEAL LENGHTENING DISTRACTION OSTEOTOMY Osteotomy is fashioned in a coronal plane 1.5 cm posterior to the calcaneocuboid joint between the anterior and middle facets This is not a simple opening wedge osteotomy, but rather a lengthening distraction wedge osteotomy, and it requires a trapezoid graft Tricortical iliac crest graft is inserted between the anterior and middle facets of the calcaneus Additional internal fixation is required
- 69. COMPLICATIONS Nonunion of calcaneal graft Displacement of the graft requiring revision Diplacement of the calcaneocuboid joint Recurrence of deformity or pain
- 70. Plantar Flexion Opening Wedge Medial Cuneiform Osteotomy Hirose and Johnson Indicated for correction of residual deformities in flat foot Forefoot supination is corrected by a plantar medial closing wedge osteotomy of first cuneiform The goal is to plantar flex the first ray down to the level of the fifth metatarsal to restore Cotton's normal “tripod” configuration.
- 72. Rigid flat foot
- 73. RIGID (OR FIXED) FLAT FOOT Tarsal coalition (peroneal spastic flatfoot, congenital rigid flatfoot) [most common cause] Heel cord tightening Accessory navicular Vertical talus
- 74. RIGID FLATFOOT Cannot be passively manipulated without causing pain Feet are flat - regardless of weight bearing / position Pain is usually a prominent symptom.
- 75. TARSAL COALITION Thin or thick bar composed of bone (synostosis), cartilage (synchondrosis) or fibrous tissue (syndesmosis) connects tarsal bones Failure of embryonic segmentation Calcaneum is held in eversion An irritative focus is produced which causes painful spasm of the peronei Impossible for the patient to walk on the lateral border of the foot due to limited inversion Mechanics of the tarsus is impaired and abnormal stresses result casing sec. degenerative arthritis
- 76. TARSAL COALITION Symptoms : do not develop until ossification of the fibrous syndesmosis or the cartilagious synchondrosis Syndesmosis and synchondrosis are usually more troublesome than synostosis Symptoms – vague active adolescents with dorsolateral foot pain around the sinus tarsi, difficulty in walking on uneven surfaces, foot fatigue, painful limp Tenderness is present along the bar The condition is known to run in families Auto. dominant inheritance with variable penetrance 50% bilateral Incidence - 0.4-6%
- 77. CALCANEONAVICULAR COALITION Symptomatic at 8 – 12 yrs Varying loss of subtalar motion Best seen on a 45 degree lat oblique projection Beaking of dorsal articular margin of talus is uncommon CT is usually not required
- 79. TALOCALCANEAL COALITION Middle facet talocalcaneal coalition is most common Symptomatic at 12 – 16 yrs of age Marked reduction or absence of subtalar motion (cardinal sign) Best seen on a Harris Beath axial calcaneal view – posterosuperior oblique projection Talar beaking is commonly seen – traction spur and not a sign of degenerative arthritis CT is usually needed for diagnosis(in coronal plane at 3mm increments)
- 81. Harris axial calcaneal view for middle facet coalition
- 82. CT scan showing middle facet coalition
- 83. TREATMENT Most patients respond to conservative treatment – Rest Shoe inserts (arch supports) Orthotics (AFO, Plastizote, UCBL insert) Shoe modifications (high top shoes, Thomas heel, Whitman plate) 4-6 weeks of immobilization in a short leg walking cast with the foot plantigrade may provide lasting relief of symptoms Splintage with an outside iron and inside T-strap
- 84. SURGICAL OPTIONS Resection of the bar and interposition of muscle, fat or gelfoam – should be performed before secondary degenerative changes have set in Calcaneal osteotomy can be combined to to correct hind foot valgus Subtalar arthrodesis Triple arthrodesis
- 85. Resection of calcaneonavicular tarsal coalition. A, Before surgery. B, Direction of osteotome. C, After resection.
- 86. Resection of middle facet tarsal coalition. A, Sheath is opened and retracted dorsally or plantarly. B, Coalition is removed with osteotome until it is flush with posterior facet.
- 87. INDICATIONS FOR TRIPLE ARTHRODESIS Extensive talocalcaneal coalition Multiple coalition Development of sec. degenerative arthritis Ball and socket ankle joint When the coalition involves more than 50% articular surface of talocalcaneal joint or more than 50% of the posterior facet
- 88. SUBTALAR ARTHROEREISIS • The concept •“limiting the ability of the calcaneus to externally rotate and the talus to internally rotate” • maintenance of correction of the arch was possible.
- 89. Maxwell and Cerniglia biomechanical classification of sinus tarsi implants. Self-locking wedge inserted in a screw fashion between the lateral process of the talus and the anterior process of the calcaneus and prevents external rotation of the calcaneus on the talus
- 90. Axis-altering device. intraarticular device that is inserted under the lateral process of the talus in the lateral most portion of the subtalar joint and elevates the lateral aspect of the talus
- 91. Impact-blocking device is inserted in bone in the floor of the sinus tarsi and acts in a similar fashion to the selflocking wedge by preventing external rotation of the calcaneus under the talus
- 92. •In summary, after review of the literature, several findings seem to be consistent: • 1. Insertion of a sinus tarsi blocking implant, whichever design is used, seems consistently to reduce the pes planus deformity and, at least in short-term follow-up studies • 2. A significant incidence of sinus tarsi pain requiring implant removal has been noted, and this pain does not always resolve with removal of the implant.
- 93. • 3. Follow-up can be characterized as midterm at best with no truly long-term studies available at this point. • 4. Further studies are needed before these devices can be recommended for general use. • 5. The literature appears to indicate that the best use of these implants is in children with symptomatic pes planus who have combined neuromuscular disorders
- 94. ACCESSORY NAVICULAR First described by Bauhin in 1605 Also called prehallux, accessory scaphoid, os tibiale externum, os naviculare secondarium and navicular secundum Separate ossification center for the tuberosity of the navicular Prevalance 5-10%
- 96. ACCESSORY NAVICULAR • Cause and effect relationship with flatfoot has not been shown • 3 types 1. Round sesamoid bone within TP tendon - rarely symptomatic 2. 8-12 mm ossicle connected to the navicular by a synchondrosis. This is the type that is usually symptomatic as the synchondrosis is at risk of disruption from traction injury / shear forces 3. Navicular beak / Cornuate navicular -fusion of acc. navicular with the primary navicular.
- 97. SYMPTOMS Usually asymptomatic, noticed incidentally Presentation - adolescence Pain over an enlarged area at the medial aspect of the navicular just at the insertion of the tibialis posterior tendon Pain aggravated by wearing tight-fitting shoes
- 98. INVESTIGATIONS Accessory navicular is best seen on the external oblique view Accessory navicular ossifies even later than a normal navicular which is the last tarsal bone to ossify CT can identify an accessory navicular Bone scan can identify a hot accessory navicular
- 99. TREATMENT Soft pads, avoid wearing tight fitting shoes Special shoes, valgus correcting shoe inserts( UCBL devise) Steroid and analgesic injections Strenghening of tibialis tendon and treatment of tendonitis Immobilization in a short leg cast
- 100. SURGERY Simple excision of the accessory navicular shelling it out of the post. tibial tendon Navicular is resected until it is slightly depressed relative to the talus and cuneiform Bone wax is applied to the to prevent regrowth Good or excellent result in 93% cases
- 101. KIDNER’S PROCEDURE Involves excision of the accessory navicular with re-routing of the central slip of the tibialis posterior laterally onto the plantar surface of the navicular, where it is sutured under tension to the surrounding ligaments Gives no added advantage in short term and long term follow up and therefore the simpler procedure is preferred
- 104. CONGENITAL VERTICAL TALUS Congenital rigid flat foot, rocker bottom foot, convex pes valgus or teratologic dorsolateral dislocation of the talo-naviculo-cuneiform joint First description by Henken in 1914 Characteristic features described by Lamy and Weissman
- 105. Bilateral congenital vertical talus in 14-month-old child
- 106. X-ray shows the vertical talus pointing downwards towards the sole and the other tarsal bones rotated around the head of the talus
- 107. after bilateral operative correction at age 14 months in which transverse circumferential approach was used.
- 108. CONGENITAL VERTICAL TALUS Congenital dislocation of talonavicular joint such that the talus is disposed vertically with its head forming the most prominent part of the sole The navicular is displaced dorsolaterally firmly lodged on to the neck of the talus, preventing reduction. The navicular abuts the ant. surface of the tibia The calcaneum is displaced posterolaterally in relation to the talus, is rigidly locked into equinus and in contact with the distal fibula The angle between the long axis of the talus and calcaneum is markedly increased The forefoot is deviated outwards and dorsally and hence the sole has a convex contour
- 109. CONGENITAL VERTICAL TALUS Dorsolateral dislocation or extreme subluxation of calcaneocuboid joint might occur Abnormal relationship of tarsal bones remain constant whether the foot is plantar flexed or dorsiflexed, this is in contrast to congenital flexible flatfoot Achilles tendon is contracted, ant. tibial and peroneal tendons are taught The subtalar joint is abnormal with the anterior facet absent and the middle facet hypoplastic
- 110. Plantar flexion lateral stress radiographs in diagnosis of congenital vertical talus. In normal foot, long axis of first metatarsal passes plantarward to long axis of talus.
- 111. In congenital vertical talus, long axis of first metatarsal remains dorsal to long axis of talus, indicating dorsal dislocation of midfoot and forefoot. with equinus deformity of calcaneus.
- 112. CONGENITAL VERTICAL TALUS Adaptive changes occur in the tarsal bones with weight bearing The talus becomes shaped like an hour glass, with its longitudinal axis almost same as the tibia Only the posterior 1/3rd of the superior articulating surface of the tibia articulates with the tibia Anterior part of the plantar surface of the calcaneus becomes rounded Callosities develop beneath the anterior end of the calcaneus and along the medial border of the foot superficial to the head of the talus
- 113. ETIOLOGY Muscle imbalance Intra-uterine compression Arthrogryposis Autosomal dominant transmission Arrest of fetal development of the foot between 7th and 12th weeks of gestation
- 114. CLINICAL PICTURE Usually bilateral Sole is characteristically convex at birth, so that it resembles the bottom of a rocking chair and hence the name Dorsolateral fold is deep and situated at the mid-tarsal area Talar head is prominent over the medial and plantar aspects Deformity from the outset is rigid Deformity may be so severe that heel might not touch the ground at all Gait is awkward and resembles a waddle Shoes are rapidly worn out over the inner sides Pain - at adolescence or soon thereafter
- 115. DIFFERENTIAL DIAGNOSIS Idiopathic flatfoot Paralytic flatfoot Spurious correction of clubfoot Talipes calcaneovalgus (benign condition easily amenable to correction) Tarsal coalition
- 116. PATHOLOGY Calcaneus is held in eversion by contracted interosseous ligament, bifurcated ligament and calcaneofibular ligament Calcaneus is fixed in equinus by contracted posterior capsule and achilles tendon Dorsal capsules of talonavicular, calcaneocuboid joints and tibio- navicular portion of the deltoid ligament are markedly contracted and prevent reduction Tibialis anterior, long toe extensors, peroneus brevis and triceps surae are contracted Posterior tibial and peroneal tendons may be displaced anteriorly so that they act as dorsiflexors rather than plantar flexors
- 117. PATHOLOGY Forefoot dorsiflexors are contracted Calcaneonavicular ligament is elongated and attenuated Posterior tibial tendon becomes attenuated as it passes over the displaced head of talus If deformity persists into late childhood, alterations in the bony shape develop that encourage redisplacement even after surgery Talus assumes hour-glass constriction, calcaneus becomes curved dorsally at its anterior end becoming beak shaped and navicular becomes wedge shaped
- 118. NONOPERATIVE TREATMENT • Difficult to treat tends to recur • Serial casting to stretch the foot in plantarflexion and inversion while counterpressure is applied to the medial aspect of the talus • Reverse Ponseti method • Complete correction rarely achieved. • Open reduction is generally required
- 119. SURGICAL OPTIONS 1 - 4 yrs : soft tissue release, open reduction and realignment of the talonavicular and subtalar joints (KUMAR, COWELL, RAMSEY) Children > 3 yrswith severe deformity generally require navicular excision at the time of open reduction 4 - 8 yrs : soft tissue release and open reduction with Grice-Green subtalar extra-articular arthrodesis >12 yrs failure of above procedure striple arthrodesis
- 120. OPEN REDUCTION AND REALIGNMENT OF TALONAVICULAR AND SUBTALAR JOINTS (KUMAR, COWELL, RAMSEY) Should be done before 2 yrs Best done as a single stage release at 1 yr STEPS Dorso-lateral soft tissue release Medial soft tissue release Reduction of talonavicular and calcaneocuboid jts Posterior soft tissue release Internal fixation
- 121. •Kodros and Dias reported a single- stage procedure • in which a threaded Kirschner wire is used as a “joystick” • To manipulate the talus into correct position. • The corrected position is held with threaded Kirschner wires across the talonavicular and subtalar joints
- 122. Single-stage correction of congenital vertical talus. Threaded Kirschner wire is placed axially in vertical talus from posterior and is used as “joystick” to manipulate talus into reduced position.
- 123. Wire is advanced across talonavicular joint.
- 124. RESULTS Results are satisfactory if surgery is done before 27 months All feet have some residual midfoot sag and forefoot abduction and some have decreased motion Commonest reason for surgical failure is inadequate reduction of the navicular
- 125. COMPLICATIONS Aseptic necrosis of the navicular Aseptic necrosis of the talus These can be averted by limited amount of dissection
- 128. Examination of the flatfoot compares the (A) nonweightbearing and (B) weightbearing arch of the foot. As the arch depresses, (C) the forefoot abducts and (D) the lesser toes become visible upon posterior observation of the foot. The relaxed calcaneal stance position is viewed standing behind the patient. A flatfoot deformity will demonstrate heel eversion that is accentuated with apparent bowing of the tendo-Achilles (Helbing sign). The too many toes sign, indicative of excessive forefoot abduction in the flatfoot, may also be noted.
- 129. POSTERIOR TIBIAL TENDON DYSFUNCTION Most common cause of adult onset acquired flat foot The components of the deformity are 1. hindfoot valgus, 2. midfoot abduction at the midtarsal joint, 3. forefoot pronation, primarily at the midtarsal joint.
- 130. • Chronic tenosynovitis (either traumatic, degenerative, or secondary to inflammatory arthritis), loss of continuity of the tendon (either complete or incomplete), and loss of the normal anatomical relationships of the tendon to its insertion or insertions (the accessory navicular or prehallux syndrome) • may render the posterior tibial tendon insufficient to perform its tasks of plantar flexion and inversion • and stabilization of the medial longitudinal arch.
- 131. •The classification system originally developed by Johnson and Strom in 1989
- 133. Teatment of stage 1
- 134. Teatment of stage 2 Conservative management of stage II disease often is successful, and most patients obtain pain relief with application of an orthotic device that has a medial post and a double upright AFO with a medial T-strap. The brace is configured to allow 20 to 30 degrees of plantar flexion and 10 degrees of ankle extension.
- 136. Teatment of stage 3 arthrodesis is indicated if conservative measures, including a double upright ankle-foot orthosis, have failed.
- 137. Treatment of stage 4 • For rigid deformities, the procedure of choice usually is arthrodesis of the ankle or tibiotalocalcaneal arthrodesis • In a select group of patients with flexible, reducible deformity, less than 10 degrees of tibiotalar tilt, and minimal lateral ankle joint arthrosis • Jeng et al. described a “minimally invasive”allograft technique for deltoid ligament reconstruction for stage IV flatfoot deformity done in conjunction with triple arthrodesis.
- 139. POSTERIOR TIBIAL TENDON RUPTURE Unilateral deformity that develops rapidly History of trauma Young patient- tendon transfer using flexor digitorum longus Elderly- splintage If this fails and symptoms are marked triple arthrodesis
Notas del editor
- 1Add history and foot notes
- 2Confirm calcaneal pitch
- 3Add indications for surgery organize 49-74
- 5Describe procedure
- 9GIVE DETAILS
- 10GIVE DETAILS
