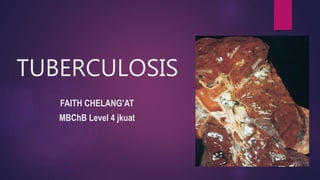
Tuberculosis by Faith Chelang'at
- 1. TUBERCULOSIS FAITH CHELANG’AT MBChB Level 4 jkuat
- 2. Tuberculosis is a communicable chronic granulomatous disease caused by Mycobacteria tuberculosis. Usually involves the lungs but also affect any other tissue in the body.
- 3. EPIDEMIOLOGY. Most common cause of death resulting from a single infectious agent according to WHO. About 1.7 billion individuals are affected worldwide. 8-10 million new cases annually. About 1.5 million deaths per year.
- 4. EPIDEMIOLOGY Tuberculosis flourishes under conditions of poverty, crowding and chronic debilitating illness. High-prevalence populations include: Immigrant from high-prevalence area Homeless or medically underserved Resident or worker in jail or long-term facility Health care worker at facility with TB Close contact to patient with active TB
- 5. EPIDEMIOLOGY High-risk populations include; HIV and other immunosuppressing conditions Chronic renal failure DM Malnourishment Malignancy Gastrectomy Biologics e.g. TNF inhibitors
- 6. ETIOLOGY Mycobacteria; Family – Mycobacteriaceae, Order - Actinomycetales. Slender rods that are acid-fast that stubbornly resist decolourization. They contain a waxy coating on the cell surface due to presence of mycolic acid. M. tuberculosis hominis - responsible for most cases of tuberculosis, the reservoir of infection found in individuals with active pulmonary disease. Transmission - direct inhalation of airborne organisms in aerosols generated by expectoration or by contaminated secretions of infected individuals. Oropharyngeal and intestinal tuberculosis acquired by drinking milk contaminated with Mycobacterium bovis. Other mycobacteria, particularly Mycobacterium avium complex, are much less virulent than M. tuberculosis and rarely cause disease in immunocompetent individuals.
- 7. PATHOGENESIS. Results in development of cell mediated immunity in a previously immunocompetent individual. This confers resistance to the organism resulting in development of tissue hypersensitivity to the tubercular antigens. The sequence of events from inhalation of the infectious inoculum is as follows;
- 8. ENTRY OF MACROPHAGES A virulent strain of mycobacterium gains entry to macrophage endosomes. This process mediated by several macrophage receptors including the macrophage mannose receptor and complement receptors that recognize several components of the bacterial cell wall.
- 9. REPLICATION IN MACROPHAGES. Once internalized the organisms inhibit normal microbicidal responses by preventing the fusion of lysosomes with the phagocytic vacuole, allowing the mycobacterium to persist and proliferate.
- 10. DEVELOPMENT OF CELL MEDIATED IMMUNITY. Occurs approximately three weeks after exposure. Processed mycobacterial antigens reach the draining lymph nodes and are presented to CD4 T cells by dendritic cells and macrophages. Under the influence of macrophage secreted IL-12 , CD4+ T cells of the Th1 subset are generated that are capable of secreting IFN- gamma.
- 11. T- CELL MEDIATED MACROPHAGE ACTIVATED AND KILLING OF BACTERIA. IFN-gamma released by the CD4+ cells is crucial for activating macrophages. Activated macrophages in turn release a variety of mediators and up-regulate expression of genes important with downstream events including; TNF-α - responsible for recruitment of monocytes, which in turn undergo activation and differentiation into epithelioid histocytes that characterize the granulomatous response. Inducible NO synthase - raises NO levels, which creates a reactive nitrogen intermediates that appear to be particularly important in killing mycobacteria and; Antimicrobial peptides (defensins) that are toxic to mycobacterial organisms.
- 12. GRANULOMATOUS INFLAMMATION AND TISSUE DAMAGE. In addition to stimulating macrophages to kill mycobacteria, the Th1 response leads the formation of granulomas and caseous necrosis.
- 14. PRIMARY TUBERCULOSIS Develops in a previously unexposed and therefore unsensitized patient. In a large majority of otherwise healthy individuals the only consequence of primary tuberculosis are the foci of scarring. Uncommonly new infection may result to progressive primary tuberculosis. This complication may happen in patients that are overly immunocompromised or who may have more subtle defects in there immune system. A clear example is in HIV-positive patients with significant immunosuppression. This is because immunosuppression results in an inability to mount a CD4+ cell mediated response that would contain the primary focus.
- 15. SECONDARY TUBERCULOSIS This arises from a previously infected individual, particularly when the host immunity is weakened. It is classically localized to the apex of one or both of the upper lobes. Usually manifests as cavitary lesions in the apices.
- 16. CLINICAL FEATURES Clinical manifestations take the form of ; Acute (primary)pulmonary infection Chronic(granulomatous) pulmonary disease or Disseminated miliary disease.
- 17. Pulmonary TB Productive cough, Fever Unexplained weight loss. Blood streaking of the sputum is frequently documented. May occasionally present with hemoptysis or chest pain. Other systemic symptoms include anorexia, fatigue, and night sweats
- 18. Miliary TB Characterized by 2-3 weeks of; Fever Night sweats Anorexia Weight loss Dry cough.
- 19. Extra pulmonary TB May present with the following depending on the organ involved Lymphadenitis – usually unilateral and painless. Most commonly at posterior cervical and supraclavicular sites (a condition historically referred to as scrofula). Lymph nodes are usually discrete in early disease but develop into a matted nontender mass over time and may result in a fistulous tract draining caseous material. Meningitis - present with intermittent headache or persistent for 2 to 3 weeks, may progress to coma Bony TB - The spine is the most common site for bony TB (Pott’s disease), which usually presents with chronic back pain and typically involves the lower thoracic and lumbar spine. The infection starts as a discitis and then spreads along the spinal ligaments to involve the adjacent anterior vertebral bodies, causing angulation of the vertebrae with subsequent kyphosis. Paravertebral and psoas abscess formation is common and the disease may present with a large (cold) abscess in the inguinal region.
- 20. Cutaneous TB –ulcer or wart like lesion at the site of inoculation. Genitourinary TB- include flank pain, dysuria, and frequency, epididymitis or a scrotal mass in male and may mimic pelvic inflammatory disease in women Pericarditis - Disease occurs in two forms; pericardial effusion and constrictive pericarditis. Fever and night sweats are rarely prominent and the presentation is usually insidious, with breathlessness and abdominal swelling. Peritonitis
- 22. INVESTIGATIONS Microbiology – sputum, bronchoscopy alveolar lavage and other clinical smear for acid-fast smear and culture Radiological – chest x-ray may show consolidation or patchy or nodular infiltrate or appearance of numerous small nodular lesions that resemble millet seeds in miliary TB Tuberculin skin testing (Mantoux test)- induration of more than 10mm in 48 to 72 hours Newer technologies, including ribosomal RNA probes or DNA polymerase chain reaction, allow identification within 24 hour.
- 23. TREATMENT OF TB For initial empiric treatment of tuberculosis (TB), start patients on a 4- drug regimen: Isoniazid, Rifampin, Pyrazinamide, and Either Ethambutol or Streptomycin. Standard treatment involves 6 months’ treatment with isoniazid and rifampicin, supplemented in the first 2 months with pyrazinamide and ethambutol. Fixed-dose tablets combining two or three drugs are preferred.
- 26. Indications for immediate treatment: any patient who is smear-positive, or smear-negative but with typical chest X-ray changes and no response to standard antibiotics. New-onset pulmonary TB and most cases of extra pulmonary TB – 6 months of therapy. Meningeal & spinal TB – 12 months of therapy; in these cases, ethambutol may be replaced by streptomycin. Pregnant women and malnourished patients – prescribed with pyridoxine to reduce risk of peripheral neuropathy associated with isoniazid. Patients can be assumed to be non-infectious after 2 weeks of appropriate therapy when drug resistance is not anticipated.
- 27. Baseline liver function and regular monitoring are important for patients treated with standard therapy. In the event of hepatotoxicity is appropriate to stop treatment and allow any symptoms to subside and the liver function tests (LFTs) to recover before commencing a stepwise re-introduction of the individual drugs. Indications of hospital admission: Uncertainty about the diagnosis, intolerance of medication, questionable treatment adherence, adverse social conditions or a significant risk of MDR- TB (culture-positive after 2 months on treatment, or contact with known MDR-TB). Corticosteroids and are currently recommended when treating pericardial or meningeal disease, and in children with endobronchial disease. They may confer benefit in TB of the ureter, pleural effusions and extensive pulmonary disease, and can suppress hypersensitivity drug reactions.
- 28. The effectiveness of therapy for pulmonary TB is assessed by further sputum smear at 2 months and at 5 months. Extra pulmonary TB must be assessed clinically or radiographically, as appropriate Treatment failure is defined as a positive sputum smear or culture at 5 months or any patient with a multidrug resistant strain, regardless of whether they are smear-positive or negative