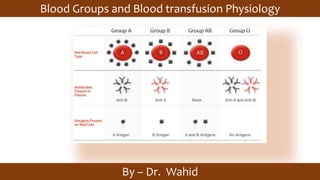
Blood Groups and Transfusion Guide
- 1. Blood Groups and Blood transfusion Physiology By – Dr. Wahid
- 2. ▪ABO and Rh systems and their clinical significance. ▪Incompatibilities in Rh systems ▪Blood transfusions - basis of blood typing, Cross matching ▪Complications of Blood transfusions (transfusion reactions)
- 3. ABO blood group system ▫First ever blood transfusion was made dog to dog by British physician Richard Lower in 1665. ▫Austrian immunologist Karl Landsteiner discovered the ABO blood group System in 1901. In 1910 he won Nobel prize for medicine for this discovery. In 1940- Karl Landsteiner and Alexander S Wiener reported another Rh blood group.
- 4. Importance of knowing about blood group system 1. Safe blood transfusion that may be life saving. 2. To prevent hemolytic disease of new born (Rh compatibility in newborn) 3. To solve the legal disputes related to parenting claimant. 4. To study the Mendelian laws of genetics.
- 5. ABO blood group system The ABO blood group antigens are complex oligosaccharide chains that differ in their terminal sugar and project above the RBC surface. following types of abs may develop- type A: anti-B abs, type B: anti-A abs, type O : both & type AB: neither.
- 6. Landsteiner’s Law 1. If a certain agglutinogen is present on the surface of RBCs, the corresponding agglutinin must be absent in the plasma. 2. If a certain agglutinogen is absent on the surface of RBCs, then corresponding agglutinin must be present in the plasma.
- 7. ABO blood types Relative frequency of different blood types: • O 47% • A 41% • B 09% • AB 3% (World) ABO blood group system- Relative frequency
- 8. Inheritance of ABO blood group system ▪The ABO locus has three main allele forms: A, B, & O. The A and B genes found on chromosome 9 and are inherited one gene (allele) from father and one from mother. 1.Homozygous A 2. Heterozygous A Genotype A/A Genotype A/0 Phenotype A Phenotype A
- 9. Blood Group Antigen Antibody Can donate to Can receive A A Anti-b A A B B Anti-A B B AB Ab None AB A, B, AB O. O none AB A, B, AB O. 0 The antigen of the donor and the antibody of recipient is considered at the time of transfusion.
- 10. Universal Donor and Recipient / ABO blood group Universal Donor : O-ve and Universal Recipient AB+ve
- 11. Blood group Genotype A AA, AO B BB, O AB AB O OO
- 12. ▪The Rh factor, named for the rhesus monkey because it was first studied using the blood of this animal. ▪85% of whites are D-positive & 15% are D-negative; over 99% of Asians are D-positive. ▪ Antibodies to Rh antigens can be involved in hemolytic transfusion reactions and antibodies to the Rh(D) and Rh antigens confer significant risk of hemolytic disease of the fetus and newborn. Rh blood group system
- 13. It contains proteins on the surface of red blood cells. After the ABO blood group system, it is the most likely to be involved in transfusion reactions. The Rh blood group system consists of 49 defined blood group antigens,among which the five antigens D, C, c, E, and e are the most important. There is no d antigen. Rh(D) status of an individual is normally described with a positive (+) or negative (–) suffix after the ABO type (e.g., someone who is A+ has the A antigen and Rh(D) antigen, whereas someone who is A– has the A antigen but lacks the Rh(D) antigen). The terms Rh factor, Rh positive, and Rh negative refer to the Rh(D) antigen only.
- 14. The hemolytic condition occurs when there is an incompatibility between the blood types of the mother and fetus. There is also potential incompatibility if the mother is Rh negative and the father is positive. When any incompatibility is detected, the mother often receives an injection at 28 weeks gestation and at birth to avoid the development of antibodies towards the fetus. The disorder in the fetus due to Rh D incompatibility is known as erythroblastosis fetalis. •Hemolytic comes from two words: "hema" (blood) and "lysis" (solution) or breaking down of red blood cells •Erythroblastosis refers to the making of immature red blood cells •Fetalis refers to the fetus. Erythroblastosis fetalis.
- 15. Prevention When the condition is caused by the Rh D antigen-antibody incompatibility, it is called Rh D Hemolytic disease of the newborn or Rh disease. Here, sensitization to Rh D antigens (usually by feto-maternal transfusion during pregnancy) may lead to the production of maternal IgG anti-D antibodies which can pass through the placenta This is of particular importance to D negative females at or below childbearing age, because any subsequent pregnancy may be affected by the Rh D hemolytic disease of the newborn if the baby is D positive. The vast majority of Rh disease is preventable in modern antenatal care by injections of IgG anti-D antibodies (Rho(D) Immune Globulin). The incidence of Rh disease is mathematically related to the frequency of D negative individuals in a population, so Rh disease is rare in old-stock populations of Africa and the eastern half of Asia, and the Indigenous peoples of Oceania and the Americas, but more common in other genetic groups, most especially Western Europeans, but also other West Eurasians, and to a lesser degree, native Siberians, as well as those of mixed-race with a significant or dominant descent from those (e.g. the vast majority of Latin Americans and Central Asians).
- 16. other's Rh factor Father's Rh factor Baby's Rh factor Precautions Rh positive Rh positive Rh positive None Rh negative Rh negative Rh negative None Rh positive Rh negative Could be Rh positive or Rh negative None Rh negative Rh positive Could be Rh positive or Rh negative Rh immune globulin injections
- 17. Hemolytic disease of the newborn (Erythroblastosis Fetalis) 1. Hydrops fetalis-baby may die in utero. 3. If mother has received anti D abs injection at time of Ist delivery, this causes neutralization of baby’s Rh+ve RBCs, and immune system does not activate to produce abs. 2. Erythroblastosis fetalis
- 18. Symptoms and signs in the newborn: • Anemia that creates the newborn's pallor (pale appearance). • Jaundice or yellow discoloration of the newborn's skin, sclera or mucous membrane. This may be evident right after birth or after 24–48 hours after birth. This is caused by bilirubin (one of the end products of red blood cell destruction). • Enlargement of the newborn's liver and spleen. • The newborn may have severe edema of the entire body. • Dyspnea (difficulty breathing)
- 19. MNSs blood group system, classification of human blood based on the presence of various substances known as M, N, S, and s antigens on the surfaces of red blood cells. This system, first discovered in 1927, has many distinct phenotypes and is of interest in genetic and anthropological studies of human populations.
- 20. There are more than 40 antigens in the MNSs blood group system. The system consists of two pairs of codominant alleles, designated M and N (identified in 1927) and S and s (identified 1947 and 1951, respectively). The alleles M and N are usually distributed in populations in approximately equal frequencies. However, the S and s alleles have varying frequencies, with the S allele occurring in about 55 percent of whites and 30 percent of blacks, and the s allele occurring in roughly 90 percent of individuals in both populations. Antibodies to the M and N antigens rarely cause incompatibility reactions. However, antibodies to S, s, and several can cause transfusion reactions and erythroblastosis fetalis
- 21. Thank you