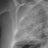
Avm.23.11
- 2. Nguyen Ngoc Anh, F, 9 years old, A13 Clinical diagnosis: seizure.
- 3. Clinical findings Pre-history: cerebral hemorrhage. No fever, no headache, no vomitting. No paralysis seizure: 1 months before being hospitalized.
- 6. DSA >>>> AVM Treated by embolization.
- 7. Definition Vascular abnormality constituted by a complex, tangled wed of afferent arteries and draining veins linked by an abnormal dysplastic intervening capillary bed Contrast with a AVF which has direct fistulous connection without intervening nidus
- 8. Etiology Initially thought to be congenital May be due to aberrant vasculogenesis and angiongenesis in embryonic Failure of the embryonic vascular plexus to fully differentiate and develop a mature capillary bed in affected area. It is likely that a combination of congenital predisposition and extrinsic factors lead to their generation
- 9. Epidemiology In the US general population is 1.4/100,000 per year No sexual preference Mean age of presentation: 20 – 40 Account for 3% stroke and 33% primary intracranial bleeding in young adults. 1/10 have aneurysms.
- 10. Angioarchitecture Arterial feeder Nidus Draining vein Intervening gliotic parenchyma
- 12. Arterial feeder Single or multiple Pial, perforating or dural Direct feeders supply as terminal branch Indirect feeder supply.
- 13. Nidus The AVM nidus is a compact plexiform of dysplastic, thin-walled vessels connecting feeding arteries to draining veins. An AVM nidus can either be globular or conical in shape; may be compact or diffuse. Within the nidus, arterial blood is shunted directly into draining veins without passage through a normal high – resistance arterial capillary network.
- 14. AVM syndromes Sturge – Weber syndrome. Rendu-Osler-Weber syndrome: autosomal-dominant syndrome of multiple visceral, mucosal and cerebral vascular malformation. Wyburn-Manson syndrome: unilateral retinal angiomatosis and cutaneous hemangioma in an ipsilateral trigerminal distribution, AVM located in midbrain.
- 15. Distribution Based on autopsy findings: Cerebral hemisphere: 60 – 70% Cerebellum: 11 – 18 % Brainstem: 13 – 16 % Deep seated: 8 – 9 %
- 16. Clinical symptoms Hemorrhage (54%) Seizures (46%) Headache (35%) Neurological deficits Asymptomatic Pediatric: hydrocephalus, heart failure
- 17. Factors increasing the Risk of Bleeding Most common symptom Nidus: 82% in small AVM 29% in medium – sized AVM 12% in large AVM Location: deep locations Basal ganglia Periventricular Intraventricular
- 18. Factors increasing the Risk of Bleeding Deep venous drainage Venous stenosis Single draining vein Feeding artery pressures Hemorrhage before
- 19. Types and size of AVM Micro AVM: < 1cm Small AVM: 1 – 3 cm Moderate AVM: 3 – 6 cm Large AVM: > 6 cm
- 20. CT Scan imaging CT is usually the first imaging modality used to rule out hemorrhage Parenchyma calcifications are observed in 20% of cases. Multi - slice CT Scan angiography
- 21. AVM diagnosis Clinical symptoms CT scanner MRI DSA
- 22. CT Scan CT is usually the first imaging modality used to rule out hemorrhage Calcification: 20% CT angiography: dynamic contrast
- 23. CT Scan
- 24. MRI On T1 and T2W images: plexiform flow void phenomenon. T1W with gadolinium: vessels are enhanced. Measure the size and the anatomic location of the nidus. MR angiography: with and without contrast
- 25. MRI
- 26. MRI
- 27. DSA Gold standard to evaluate AVM Selective angiongraphy is always necessary to make a decision to plan the treatment
- 29. Different diagnosis Venous malformation Cavernoma AVF Telangectasia
- 31. Classification ( Spetzler Martin) Size of nidus – Small (<3cm): 1 – Medium (3-6cm): 2 – Large (>6cm): 3 Eloquence area – Yes: 1 – No: 0 Deep venous drainage – Yes: 1 – No: 0
- 33. Spetzler Martin grading Grading AVMs according to their degree of surgical difficulty and risk of surgical morbidity and mortality There are 5 grades Low grade AVM: Grade I, II, Medium grade: Grade III High grade AVM: Grade IV, V
- 34. Management Observation: large AVM, no bleeding before Surgery Embolization Radiosurgery Combination treatment
- 35. Surgery The most effective treatment: small and superfacial AVM. Pediatric: > 5 years old. Remove large, life-threatening hematoma.
- 36. Embolization First described in 1960 by Luessenhope and Spence A rapidly evolving technique Embolic agent: histoacryl with lipiodol, onyx... Complete obliteration by embolization alone: 40-60% AVM Multiple sessions are required most of cases AVM aneurysm.
- 37. Aims of embolization Curative embolization Palliative embolization Partial embolization Pre-operation embolization Pre-radio surgery embolization
- 38. Complication Incomplete embolization Intracranial hemorrhage Ischemia Gluing of micro catheter Perfusion pressure breakthrough
- 39. Radiosurgery AMVs are inoperable Deep AVMs Diffusion AVMs
- 41. Tool for treatment: pros and cons Embolization Surgery Radiosurg Low procedural invasivity 2 1 3 Occlusion capacity 1-2 3 2 Speed of efficacy 2-3 3 1 Long-term reliability 2-3 3 3 Independent from size 3 2 1 Independent from brain functionality 3 1 2 Independent from angio-archi 1 2 3 Independent from flow 1 3 2
- 42. Thanks for your attention!
- 43. General recommendation SM grade Deep perfo vessel Size 1st choice 2nd choice 1 and 2 Sx Rx 3 Absent Sx Rx 3 Present < 3 cm Rx Px 3 Present >3 cm Px Rx + Ex 4 and 5 Absent Ex + Sx Px 4 and 5 Present Px Rx + Ex