Cirrhosis Causes, Symptoms, Diagnosis & Treatment
- 1. Fghيلبيل ODAI RJOUB (STUDENT) - HEBRON UNIVERSITY- BIOLOGY DEPARTMENT-
- 2. Cirrhosis: is a serious chronic disease , is widespread disruption of normal liver structure by fibrosis and the formation of regenerative nodules that is caused by any of various chronic progressive conditions affecting the liver (such as long-term alcohol abuse or hepatitis). Cirrhosis is derived from Greek word kirros=orange or tawny and osis=condition
- 3. -WHO definition :a diffuse process characterized by liver necrosis and fibrosis and conversion of normal liver architecture into structurally abnormal nodules that lack normal lobular organization.
- 5. Causes: A wide range of diseases and conditions can damage the liver and lead to cirrhosis. The most common causes are: Alcohol abuse Hepatitis( A,B,C) Use of drugs Hepatic congestion from severe right sided heart failure Constrictive pericarditis Valvar diseases Wilsons diseases Infiltrative diseases( amyloidosis, glycogen storage diseases,haemochromatosis)
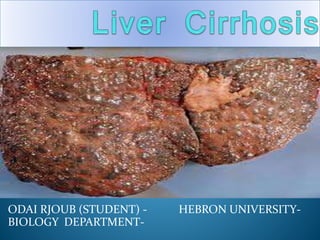
- 8. Pathology of cirrhosis: nodularity(regenerating nodules). fibrosis(deposition of dense fibrous septa)- fragmentation of sample. abnormal liver architecture hepatocyte Abnormalities : pleomorphism ,dysplasia , hyperplasia Gross pathology : irregular surface ,yellowish Color , small ,firm Nodules surrounde d by fibrous tissue Normal Cirrhosis
- 9. Four types of cirrhosis: 1. Alcoholic (Laennec’s) Cirrhosis – Associated with alcohol abuse – Preceded by a theoretically reversible fatty infiltration of the liver cells –Widespread scar formation 2. Postnecrotic Cirrhosis – Complication of toxic or viral hepatitis – Accounts for 20% of the cases of cirrhosis – Broad bands of scar tissue form within the liver
- 10. 3.Biliary Cirrhosis – Associated with chronic biliary obstruction and infection – Accounts for 15% of all cases of cirrhosis 4. Cardiac Cirrhosis – Results from longstanding severe right-sided heart failure
- 11. CLINICAL FEATURES (symptoms): • Hepatomegaly (although liver may also be small) Jaundice • Ascites • Circulatory changes – Spider telangiectasia, palmar erythema, cyanosis • Endocrine changes – Loss of libido, hair loss – Men: gynecomastia, testicular atrophy, impotence – Women: breast atrophy, irregular menses, amenorrhea
- 12. • Hemorrhagic tendency Bruises, purpura, epistaxis, menorrhagia • Portal hypertension Splenomegaly, collateral vessels, variceal bleeding, fetor hepaticas • Hepatic (portosystemic) encephalopathy • Other features Pigmentation, digital clubbing
- 13. Complications: Portal hypertension Ascites Hepatic encephalopathy Spontaneous bacterial peritonitis Renal failure Infection Hepatocellular carcinoma
- 14. Diagnosis of cirrhosis: 1. clinical 2. laboratory 3. radiologic 4. liver biopsy 5. Endoscopy
- 15. 1.clinical: Any patient with chronic liver disease Chronic abnormal aminotransferases and/or alkaline phosphatase Physical exam findings: Stigmata of chronic liver disease (muscle wasting, vascular spiders, palmar erythema) Palpable left lobe of the liver Small liver span Splenomegaly Signs of decompensation (jaundice,ascites,asterixis)
- 16. 2.laboratory: · Liver insufficiency · Low albumin (< 3.8 g/dL) · Prolonged prothrombin time (INR > 1.3) · High bilirubin (> 1.5 mg/dL) · Portal hypertension · Low platelet count (< 175 x1000/ml) · AST / ALT ratio > 1
- 17. 3.Radiologic: ultrasound, CT, or MRI scans. Observed: · Small nodular liver · Intra-abdominal collaterals · Ascites · Splenomegaly · Colloid shift to spleen and/or bone marrow Yes No Yes No Liver
- 18. 4.liver biopsy: a small sample of liver cells are extracted and examined under a microscope. The biopsy can confirm cirrhosis and its cause. 5. Endoscopy: a long, thin tube with a light and video camera at the end goes down the patient's food pipe (esophagus) and into their stomach. The doctor looks out for swollen blood vessels (varices), a hallmark sign of cirrhosis.
- 19. Treatment of liver cirrhosis: Treatment for cirrhosis varies based on what caused it and how far the disorder has progressed. Some treatments your doctor might prescribe include: beta blockers or nitrates (for portal hypertension) quitting drinking (if the cirrhosis is caused by alcohol) banding procedures (used to control bleeding from esophageal varices) intravenous antibiotics (to treat peritonitis that can occur with ascites) hemodialysis (to purify the blood of those in kidney failure) lactulose and a low protein diet (to treat encephalopathy) Liver transplantation is an option of last resort, when other treatments fail. All patients must stop drinking alcohol. Medications, even over-the- counter ones, should not be taken without consulting your doctor.
- 20. General management: Good nutrition Avoid protein excess Low salt diet Alcohol abstinence Avoid NSAID and sedatives & opiates Cholestyramine for pruritus
- 21. Specific treatment :(liver transplantation) Indications for liver transplantation cholesteric forms of cirrhosis PBC Alcoholic cirrhosis cirrhosis due to hepatitis C Alpha1Antitrypsin deficiency Haemochromatosis
- 22. Signs of liver in suffiency pointing to the need for liver transplant: Sustained or increased jaundice TB >100 Umol/l Ascites Hepatic encephalopathy not responding to medical therapy hypoalbuminemia <30g/l Fatigue and lethargy affecting the quality of life Intractable itching Recurrent variceal bleeding
- 23. Statistics: • > 50% of liver disease in the US is directly related to alcohol consumption • Of the estimated 15 million alcoholics in the USA 10-20% have or will develop cirrhosis • Growing number of cases related to chronic hepatitis C • 4th leading cause of death in people between 35 and 54 years of age Direct correlation between alcohol consumption in any geographic area and the death rate from cirrhosis in that area