Urinary Tract Infections
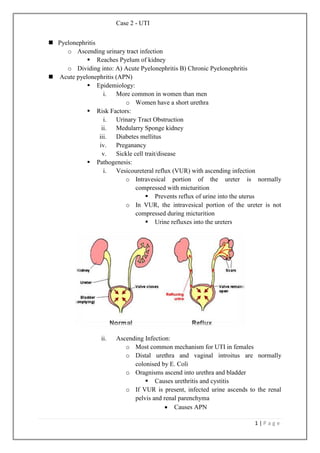
- 1. Case 2 - UTI 1 | P a g e Pyelonephritis o Ascending urinary tract infection Reaches Pyelum of kidney o Dividing into: A) Acute Pyelonephritis B) Chronic Pyelonephritis Acute pyelonephritis (APN) Epidemiology: i. More common in women than men o Women have a short urethra Risk Factors: i. Urinary Tract Obstruction ii. Medularry Sponge kidney iii. Diabetes mellitus iv. Preganancy v. Sickle cell trait/disease Pathogenesis: i. Vesicoureteral reflux (VUR) with ascending infection o Intravesical portion of the ureter is normally compressed with micturition Prevents reflux of urine into the uterus o In VUR, the intravesical portion of the ureter is not compressed during micturition Urine refluxes into the ureters ii. Ascending Infection: o Most common mechanism for UTI in females o Distal urethra and vaginal introitus are normally colonised by E. Coli o Oragnisms ascend into urethra and bladder Causes urethritis and cystitis o If VUR is present, infected urine ascends to the renal pelvis and renal parenchyma Causes APN
- 2. Case 2 - UTI 2 | P a g e Gross and microscopic findings: i. Greyish white areas of abscess formation are in the cortex + medulla ii. Microabscess formation occurs in the tubular lumens and intersstitium (Shown below) Clinical Findings: i. Spiking fever, flank pain ii. Increased frequency of urination iii. Painful urination (dysuria) Laboratory findings: i. WBC casts (key fidning) ii. Pyuria iii. Bacteriuria (usually E. Coli) iv. Haematuria Complications: i. Chronic pyelonephritis ii. Perinephric abscess iii. Renal Paillary necrosis iv. Septicemia with endotoxic shock
- 3. Case 2 - UTI 3 | P a g e Chronic Pyelonephritis (CPN) Pathogensis: i. VUR starting in young girls ii. Lower urinary tract obstruction o Produces hydronephrosis o Example: Prostatic hyperplasia Renal stones Gross and microscopic findings: i. Reflux type of CPN o U-shaped cortical scars overlying a blunt calyx o Visible with an intravenous pyelogram (IVP) ii. Obstruction type CPN o Uniform dilation of the calyces o Diffuse thinning of cortical tissues iii. Microscopic findings o Chronic inflammation Secondary scarring of the glomeruli o Tubular atrophy Tubules contain: Eosinophilic material o Resemble thyroid tissue ‘’Thyroidization’’ Note here the changes we call "thyroidization." You will see many chronic inflammatory cells in the interstitial tissue and dilated tubules containing pink staining proteinaceous goo, giving the appearance of thyroid colloid. You should note the scarring in the interstitial tissue in general and to some degree around the glomeruli. This is often associated with chronic ischemic injury of the kidney, which worsens as the process proceeds. Think diabetes and hypertension. Reference: http://medsci.indiana.edu/c602web/602/ c602web/renal/slide79.htm Clinical and laboratory findings
- 4. Case 2 - UTI 4 | P a g e i. History of recurrent APN ii. May cause hypertension o Reflux nephropathy is a cause of hypertension in children iii. May cause Chronic Renal Failure (CFR) Night Sweats: o There is no good evidence based diagnosis answer Due to the following: i. Limited number of studies on subjects with such ailment ii. No clinical trial have directly studied symptomatic relief of night sweats alone iii. History taking is the best initial diagnostic tool ( Strength of recommendation (SOR): C, based on usual practice and clinical opinion) Very common complaint for: i. Menopausal women with hot flashes ii. Most common age group in both genders (41-55 years) iii. Common causes not widely studies, mainly attributed to lymphoma, TUBERCOLOSIS, and HIV infection. o Not common in outpatient care! iv. Medications, such as: o Antidepressant (SSRIs, Venlafaxine... etc.) o Antimigranes o Antipyretics (Aspirin, acetaminophen, and NSAIDS) o Cholinergic agonists o GNRH agonists o Hypoglycaemic agents o Sympathomimetic agents o Others, alcohol, beta blockers, and calcium channel blockers to name a few! Differential diagnosis:
- 5. Case 2 - UTI 5 | P a g e Tuberculosis (TB) o Epidemiology and pathophysiology: Contracted by inhalation of Myobacterium tuberculosis Characteristics: i. Strict aerobe, acid fast (due to mycolic acid in cell wall) Screening: i. Purified Protein derivative (PPD) intradermal skin test o Does NOT distinguish active from inactive disease Primary TB: i. Subpleural location o Upper part of the lower lobes or lower part of the upper lobes ii. Usually resolves o Produces a calcified granuloma or area of scar tissue o May be a nidus for secondary TB Secondary (reactivation) TB: i. Due to reactivation of a previous primary TB site ii. Invovles one or both apices in upper lobes of respiratory lung
- 6. Case 2 - UTI o Ventilation (oxygenation) is greatest in the upper lobes o Decrease incidence of TB in mountain people Used to be previous treatment before advent of 6 | P a g e strong antibiotics Increased antibiotics resistance M. TB strains brought back mountain less oxygenation regimen o Cavitary lesion due to release of cytokines from memory T Cells iii. Clinical findings: o Fever o Drenching night sweats o Weight loss iv. Complications: o Miliary spread in lungs due to invasion into the bronchus or lymphatics o Miliary spread to extrapulmonary sites Due to invasion of pulmonary vein tributaries Kidney is the most common extrapulmonary site Also called: tuberculosis cutis acuta generalisata o Massive hemoptysis o Bronchietctasis o Scar carcinoma o Granulomatous hepatitis o Spread to vertebra (Pott’s disease) Referred Pain:
- 7. Case 2 - UTI o Pain originating in a visceral structure may be referred to and felt in a somatic 7 | P a g e structure o Several proposed theories in explaining its mechanism i. Convergence – projection theory of visceral pain o Suggest that two different afferent segments terminate at the same spinal cord level and end there. o Converging nociceptive inputs into same synaptic interneuron or second order neuron o Transmitted to higher brain centers through the same dorsal horn and intermediate grey matter ii. Concept of referred pain o Second order GSA are continuously being activated by GVA first order neurons o Thereby, lowering threshold of stimulation of 2nd order neurons o Nociceptive inputs is relayed to its somesthetic cortex o It normally receives normally somatic information from other areas, such as upper limb o The brain interprets such information as if it was coming from somewhere else o Thus, it’s a problem of the terminal end (i.e., somatosensory cortex) that interprets the signals not the stimulus or receptor that establish localisation of such sensations None Proven to be true!!! o Still unknown o Expanded interest in research after World War II Due to i. Generalised painful sensations from phantom limb pain of soldiers ii. Increased incidence of myocardial infarcts with the blooming economic prosperity o Been known as early as 1880’s o Best example: Angina pectori i. Pain sensation arising in heart muscle ii. Experience as pressure in chest, back , arm iii. All from regions served by the same segmental spinal nerve o Can be manifested as a toothache, and neck pain Due to same embryological loci derivation Patients may visit a dentist, but they have underlying heart problems GO TO A CARDIOLOGIST!!! o Other areas (related to the case): i. Suprapubic pain: Prostate hyperplasia
- 8. Case 2 - UTI 8 | P a g e ii. left flank tenderness : pylonephrititis Urine analysis: o Gold standard in initial work up of kidney function A diagnostic tool i. Ordered at intervals as a rapid method o Helps monitor organ’s Function Status Response to treatment ii. Commonly ordered due to UTI’s symptomps: o Abdominal pain o Back pain o Dysuria, or frequet urination o Haematuria iii. Can be useful in monitoring certain conditions o Interpretation of the results: i. Visual examination: o Urine colour, clarity, and concentration Normal: shades of yellow From very pale to dark amber
- 9. Case 2 - UTI 9 | P a g e o Sometimes blood can contaminate it Due to haemorroids Woman’s mensturation Other causes (many pathologic) o Depth of urine: Crude indicator of its concentration Pale yellow or colourless Diluted urine (aka, water loss) Dark yellow Concentrated highly osmotic urine o Seen In first morning urine o With dehydration o Or during a fever o Clarity Different termss: Clear Slighly cloudy Cloudy Turbid Normal: clear or cloudy Substances can cause cloudy urine o Prostatic fluid o Sperm o Mucous o Cells from skin o Normal urine crystals Or Bacteria needs attention!! ii. Chemical examination: o Using prepared test strips Normal plastic strips holding small squares of test pads paper They absorb urine once dippped Chemical reactionoccurs Pad colour changes within seconds to minutes Timing is important in diagnosis May result in errors o Best use automated instruments to read Change of colour approximated amount of existing substance Example:
- 10. Case 2 - UTI o Slight color – small [protein] o Dark color - large [protein] 10 | P a g e o Frequent chemical tests: Specific Gravity: Indicates urine concentration o No abnormal values Comparison between dissoloved substances and water Test pad o Upper limit (1.035) o Lower limit (1.002) Underlying causes: o Lack of concentration and dilution (e.g., CRF) o First sign of intrinsic renal disease pH: No abornamal values Indicates acidic or alkaline pH Determined by: o Diet - Low carb diet = Alkaline - High protein diet = Acidic o Proteus infection: Alkaline urine, urease converts urea into ammonia Can cause crystals due to acidity or alkalinity o Crystals forming in kidney, are called ‘’calculus’’ Protein: Elevated in urine, proteinuria o Early sign of kidney disease o Normal, little or no protein Detects albumin (not globulins) SSA: detects albumin and globulins Albuminuria: dipstick and SSA have same results Disorders that cause it: o That can cause high protein level in blood
- 11. Case 2 - UTI o Disorders causes destruction of 11 | P a g e RBC’s o Inflammation o Vaginal secretion that get into urine Glucose: Not normally present in urine When present, called: glucosuria Results from: 1) Excessive high glucose level in blood, diabetes militus 2) Reduction in renal threshold, normal pregnancy and glucosuria Ketons: Not normally found in urine o Intermediate products of fat metabolism Present in high amounts, called: ketonuria Can be an early indication of insufficient insulin Causes: o Diabetic ketoacidosis o Starvation o Ketogenic diets o Severe exercise o Exposure to cold o Carbohydrates loss, (frequent vomitting) Test only detects acetone and AcAc (not β-OHB) Blood: Always pathologic in urine Sometimes chemically can be negative, but microscopically found positive o When it happens We test for ascorbic acid ( vitamin C) It results into falsely low, or falsely negative High levels are called: o Hemoglobinuria
- 12. Case 2 - UTI 12 | P a g e o Hematuria o Or Myoglobinuria Underlying causes: o Intravascular haemolytic anaemia o Renal calculus o Infection o Cancer o Crush injuries Discussed later in more details, under Haematouria section Leukocyte esterase: An enzyme present in WBC’s Normally there are few WBC’s in urine o High levels, will result in this screening test positive Presence of esterase in neutrophils (pryuria) Sterile pryuria (neutrophils present but negative standard urine culture) Underlying causes: o Infection o Chlamydia trachomatis urithritis o Renal tuberclusis Nitrite: Bacteria convert nitrate into nitrite in urine When bacteria present, they cause UTI, leading to increase of nitrites Postive test is an indication of UTI Underlying cause: o Nitrate reducing uropathogens ex- E.coli Billirubin: Not normal present Produced by liver from haemoglobin of dead circulating RBcs When present, called: Bilirubinuria Underlying cause: o Viral hepatitis o Obstructive jaundice Urobilonogen: Present in urine in low concentration o Derivavitive of bilirubin
- 13. Case 2 - UTI 13 | P a g e Underlying causes: o Obstructive jaundice o Viral hepatitis o Extravascular haemolytic anemia (e.g., spherocytosis) iii. Microscopic examination: o Cells: Bacteria Red blood cells (hematuria) Neutrophils (pyuria) Oval fat bodies Underlying causes: o UTI (commonly) o Renal stones o Cancers (bladder, renal) o Infection o Benign prostatic hyperplasia o Sterile pyuria o Renal tubular cells with lipid (nephrotic syndrome) o Casts Hyaline RBC’s WBC’s Renal tubular cell Fatty Waxy (refactile, acellular) Haematuria o Definition: More than three red blood corpuscles are found in centrifuged urine per high power field microscopy (>3RBC/HP). Aetiology: i. Diseases of urinary system (most common cause) o Vascular arteriovenous malformation arterial emboli or thrombosis arteriovenous fistular nutcracker syndrome renal vein thrombosis loin-pain hematuria syndrom coagulation abnormality excessive anticoagulation o Glomerular
- 14. Case 2 - UTI IgA nehropathy thin basement membrane disease (Alport 14 | P a g e syndrome) other causes of primary and secondary glomerulonephritis o Interstitial allergic interstitial nephritis analgesic nephropathy renal cystic diseases acute pyelonephritis tuberculosis renal allograft rejection o Uroepithelium malignancy vigorous excise trauma papillary necrosis cystitis/urethritis/prostatitis (usually caused by infection) parasitic diseases (e.g. schistosomiasis) nephrolithiasis or bladder calculi o Multiple sites or source unknown Hypercalciuria ii. System disorders: o Haematological disorders: aplastic anemia leukemia allergic purpura hemophilia ITP (idiopathy thrombocytopenic purpura) o Infection: infective endocarditis septicemia epidemic hemorrhagic fever (Hantaan virus) scarlet fever (-hemolytic streptococcus) leptospirosis (leptospire) filariasis (Wuchereria bancrofti, Brugia malayi) o Connective tissue diseases systemic lupus erythematous (SLE) polyarthritis nodosa o Cardiovascular diseases
- 15. Case 2 - UTI 15 | P a g e hypertensive nephropathy chronic heart failure renal artery sclerosis o Endocrine and metabolism diseases gout diabetes mellitus iii. Diseases of adjacent organs to urinary tract o Appendicitis o salpingitis o carcinoma of the rectum o carcinoma of the colon o uterocervical cancer iv. Drug and chemical agents o Sulfanilamides o anticoagulation o cyclophosphamide (CTX) o mannito v. miscellaneous o exercise o “idopathic” hematuria Clinical Features: i. Colour: o Depends on amount of RBC’s in urine Ph value Normal: o Yellow colour o 6.5 ii. pH: o Acidic: more darker (brown or black) o Alkaline: red
- 16. Case 2 - UTI Red urine, indicative of its alkalinity Dark urine, indicative of its acidity 16 | P a g e A) Red cast in urine B) RBC’s in urine
- 17. Case 2 - UTI 17 | P a g e Drugs: o Fluroquinolones: 1st generation: - Nalidxic acid 2nd generation : i. Aprofloxicin ii. Norfloxicin iii. Ofloxoicin 3rd generation: larofloxicin 4th generation: Moxifloxacin Fatal Have broad spectrum activity (gram (+) , and gram (-)) Inhibit DNA replication by interfering with Topoisomerase II, IV Drug of Choice: o For resistant tuberclusis patient o Isoniazid: Prodrug that must be activated by bacterial catalylase o Enzyme present in M. TB o Known as kat G. o Form a complex inhibits fatty acid synthesis Decreases synthesised mycolic acid No bacterial wall o Side effects: Rash
- 18. Case 2 - UTI 18 | P a g e Hepatitis Anemia Peripheral neuropathy Mild CNS disturbances o Rifampin: Inhibit DNA dependant RNA polymerase o By binding to B-subunit of RNA o Prevents transcription to RNA o Thus, no translation to proteins Side effects: i. Hepatotoxicity (most common) ii. Respiratory distress iii. Abdominal pain iv. Nausea v. Vomitty vi. Cramps vii. Diarrhoae viii. Flue-like syndrome o Pyrazinamide: Prodrug that is a activated by pyrazanmaidase Present in M. Tuberclosis Forms pyrozonic acid Inhibits FAS Distubes bacterial wall Side effects: i. Most common: arthlagia ii. Most severe: hepatotoxicity o Ethambatol: Bacteriostatic o Obstruct of cell wall synthesis (TB) o Disturbs arabinogalactin synthesis By inhibiting arabynosyl transeferase Important in bacterial wall synthesis References: o Robbins o http://medsci.indiana.edu o Up-to-date o http://www.edrep.org o http://acutemed.co.uk o http://en.diagnosispro.com/ o http://www.nlm.nih.gov o http://jfponline.com
