Alternative Routes of Administration for Oral Medications
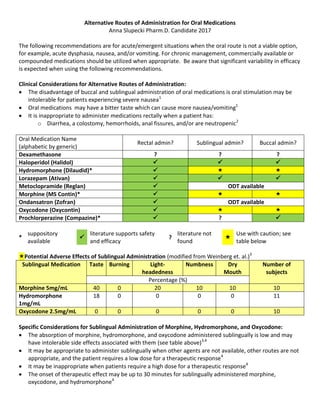
- 1. Alternative Routes of Administration for Oral Medications Anna Slupecki Pharm.D. Candidate 2017 The following recommendations are for acute/emergent situations when the oral route is not a viable option, for example, acute dysphasia, nausea, and/or vomiting. For chronic management, commercially available or compounded medications should be utilized when appropriate. Be aware that significant variability in efficacy is expected when using the following recommendations. Clinical Considerations for Alternative Routes of Administration: The disadvantage of buccal and sublingual administration of oral medications is oral stimulation may be intolerable for patients experiencing severe nausea1 Oral medications may have a bitter taste which can cause more nausea/vomiting1 It is inappropriate to administer medications rectally when a patient has: o Diarrhea, a colostomy, hemorrhoids, anal fissures, and/or are neutropenic2 Oral Medication Name (alphabetic by generic) Rectal admin? Sublingual admin? Buccal admin? Dexamethasone ? ? ? Haloperidol (Halidol) Hydromorphone (Dilaudid)* Lorazepam (Ativan) Metoclopramide (Reglan) ODT available Morphine (MS Contin)* Ondansatron (Zofran) ODT available Oxycodone (Oxycontin) Prochlorperazine (Compazine)* ? * suppository available literature supports safety and efficacy ? literature not found Use with caution; see table below Potential Adverse Effects of Sublingual Administration (modified from Weinberg et. al.)3 Sublingual Medication Taste Burning Light- headedness Numbness Dry Mouth Number of subjects Percentage (%) Morphine 5mg/mL 40 0 20 10 10 10 Hydromorphone 1mg/mL 18 0 0 0 0 11 Oxycodone 2.5mg/mL 0 0 0 0 0 10 Specific Considerations for Sublingual Administration of Morphine, Hydromorphone, and Oxycodone: The absorption of morphine, hydromorphone, and oxycodone administered sublingually is low and may have intolerable side effects associated with them (see table above)3,4 It may be appropriate to administer sublingually when other agents are not available, other routes are not appropriate, and the patient requires a low dose for a therapeutic response4 It may be inappropriate when patients require a high dose for a therapeutic response4 The onset of therapeutic effect may be up to 30 minutes for sublingually administered morphine, oxycodone, and hydromorphone4
- 2. Clinical Evidence Supporting Recommendation Dexamethasone: No literature was available on the efficacy or safety of administration rectally, sublingually, or buccally Haloperidol: Increasing concentrations of haloperidol increases the buccal drug absorption1 Halperidol tablets can be administered rectally and dosed the same as for oral administration7 Hydromorphone: Hydromorphone has an acceptable rectal bioavailability8 Lorazepam: Sublingual lorazepam given on an empty stomach and held under the tongue for 15 minutes has evidence of safety and effectiveness1 For sublingual administration, lorazepam can be dosed the same as for oral administration7 Rectally administered lorazepam has prolonged absorption5 Lorazepam has an acceptable rectal bioavailability8 Buccal administration of lorazepam has not been associated with specific adverse events11 Metoclopramide: Metoclopramide may be administered rectally5,6,7,8 Morphine: The rate of morphine’s diffusion across the rectal membrane is dependent on hydration2,6 The rectal absorption of morphine is equivalent to oral morphine2,8 For rectal administration, morphine dose conversion is 1:1 from oral, but some patients may need a dose reduction due to sedation7 Do not crush MS Contin tablets; crushing tablets could lead to overdose10 No local adverse side effects have been associated with rectal administration of morphine10 There is considerable variability among patients on absorption and metabolism2 Morphine is not readily absorbed in the oral cavity and some patients may report bitter taste, burning, and purititis2 Ondansatron: Ondansatron can be administered as a retention enema and has similar efficacy to oral administration6,8 Oxycodone: Safety and efficacy of rectally administered oxycodone is comparable to oral administration2,8 Oxycodone oral solution is safe and effective to administer rectally6 Prochlorperazine: Prochlorperazine extended release tablets given rectally have a duration of action of approximately 12 hours6 It may be mixed with water, but may not be required9 Prochlorperazine has an acceptable rectal bioavailability but has a delayed onset of action8,9 Whole or crushed tablets can be effectively absorbed within a reasonable time period9 Rectal irritation after rectal tablet administration has been reported9 Buccal administration of prochlorperazine is better than placebo at reducing nausea12
- 3. References 1. Thompson D, DiMartini A. Nonenteral Routes of Administration for Psychiatric Medications. Psychosomatics. 1999; 40(3):185-192. doi:10.1016/S0033-3182(99)71234-X. 2. Mercadante S. When oral morphine fails in cancer pain: the role of the alternative routes. The American Journal of Hospice & Palliative Care. Nov/Dec 1998; 333-342. 3. Weinberg, D. S., Inturrisi, C. E., Reidenberg, B., Moulin, D. E., Nip, T. J., Wallenstein, S., Houde, R. W. and Foley, K. M. (1988), Sublingual absorption of selected opioid analgesics. Clinical Pharmacology & Therapeutics, 44: 335–342. doi:10.1038/clpt.1988.159 4. Warren D. Practical Use of Rectal Medications in Palliative Care. Journal of Pain and Symptom Management. 1996; 11(6):378-386 5. Warren D. Practical Use of Rectal Medications in Palliative Care. Journal of Pain and Symptom Management. 1996; 11(6):378-386. 6. Davis MP, Walsh D, LeGrand S, Naughton M. Symptom control in cancer patients: the clinical pharmacology and therapeutic role of suppositories and rectal suspensions. Support Care Cancer. 2002; 10:117-138. Doi:1007/s00520-001-0311-6. 7. PL Detail-Document, Giving Meds by Alternative Routes. Pharmacist’s Letter/Prescriber’s Letter. Februrary 2015. Access date: 9/9/16. 8. Samala RV, Davis MP. Palliative care per rectum. Fast Facts and Concepts. September 2012;257. Available at: http://www.mypcnow.org/blank-rskfm. 9. Brashler K. On-Demand Clinical News, Prochlorperazine (Compazine) and Promethazine (phenergan) Tablets; Pharmacokinetic Properties and Rectal Absorption. ProCare HospiceCare. Jul/Aug 2014. Available at: https://phc.procarerx.com/docs/ondemand/2014/HospiceCare%20Newsletter%20July-August.pdf. 10. Maloney CM, Kesner RK, Klein G, Bockenstette J. The rectal administration of MS Contin ®: Clinical implications of use in end stage cancer. The American Journal of Hospice & Palliative Care. 1989; Jul/Aug:34-35. 11. Anderson, M., Tambe, P., Sammons, H. et al. Eur J Clin Pharmacol (2012) 68: 155. doi:10.1007/s00228-011- 1109-1 12. Zhang, Hao, Zhang, Jie, & Streisand, James B. (2002). Oral mucosal drug delivery: Clinical pharmacokinetics and therapeutic applications. Clinical Pharmacokinetics, 41(9), 661-80