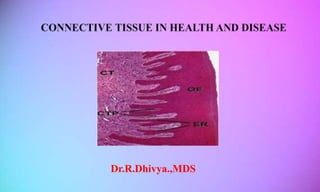
Connective Tissue in health and disease
- 2. INTRODUCTION DEFINITION CONNECTIVE TISSUE OF PERIODONTIUM Gingiva Periodontal ligament Cementum Alveolar bone CONCLUSION REFERENCES In Health and Disease
- 3. Most widespread and abundant type of tissue in the human body. Major constituent is extracellular matrix, composed of fibres, ground substance & tissue fluid. Structurally, connective tissue can be divided into 3 classes: cells, fibres & ground substance. Forms a vast and continuous compartment throughout the body and has the widest variety of functions.
- 4. A tissue of mesodermal origin that consists of various cells (as fibroblasts and macrophages) and interlacing protein fibers (as of collagen) embedded in a chiefly carbohydrate ground substance, that supports, ensheathes, and binds together other tissues, and that includes loose and dense forms (as adipose tissue, tendons, ligaments and aponeuroses) and specialized forms (as cartilage and bone). Merriam-Webster's Learner's Dictionary .
- 5. The Peridontium is defined as those tissues supporting and investing the tooth that consists of Cementum Periodontal ligament Bone lining the alveolus Part of the gingiva facing the tooth
- 6. GINGIVAL CONNECTIVE TISSUE- LAMINA PROPRIA It consists of 2 layers : 1.Papillary layer 2.Reticular layer
- 7. Extra cellular compartment Fibers -60% Ground substance -35% Cellular compartment -5% Fibroblasts -65% Mast cells Macrophages Inflammatory cells Gargiulo” et al. (1961) determined that the average mean measurements for – Sulcus depth 0.69 mm; The epithelial attachment, 0.97 mm Connective tissue attachment 1.07 mm.
- 8. Fibroblasts are of mesenchymal origin and play a major role in the development, maintenance and repair of gingival connective tissues. As with connective tissue elsewhere in the body, fibroblasts synthesize collagen and elastic fibers, as well as the glycoproteins and glycosaminoglycans of the amorphous intercellular substance.
- 9. Numerous and are responsible for the production of certain component of matrix Produce vasoactive substances which can affect the function of the microvascular system and control the flow of blood through the tissue In human periodontal disease there is an increase in the number of mast cells that may be participating either in the destructive events or in the defense mechanism of periodontal disease via secretion of cytokines.
- 10. Are present in the gingival connective tissue as components of the mononuclear phagocyte system (reticuloendothelial system) Two main groups designated : M1 "killer" macrophages M2 "repair" macrophages These histiocytes have two distinct functions: Phagocytosis Antigen presentation.
- 11. Neutrophils can be seen in relatively high numbers in both the gingival connective tissue and the sulcus Small foci of plasma cells and lymphocytes are found in the connective tissue near the base of the sulcus These inflammatory cells usually are present in small amounts in clinically normal gingiva.
- 12. Fills the space between fibers and cells Has high content of water Produced by fibroblasts some components by mast cells and others derived from blood Main constituents are PROTEOGLYCANS GLYCOPROTEINS
- 13. Glycosaminoglycans : Apart from hyaluronan, all glycosaminoglycans are sulfated to varying degrees. Chondroitin sulfate Dermatin sulphate Heparin and Heparin Sulphate Keratin Sulphate Hyaluronan Oligosaccharides
- 14. MATRIX ORGANIZERS AND SPACE FILLERS : Aggrecan Versican Large extracellular proteoglycans Perlecan Leucine rich interstitial proteoglycans Small extracellular proteoglycans Centoglycans CELL SURFACE PROTEOGLYCANS Glypicans Syndecans – 1,2,3,4 Thrombomodulin CD 44 Betaglycans PROTEOGLYCANS OF HEMATOPOIETIC CELLS Serglycin
- 15. Regulate diffusion and fluid flow through the matrix Determinants for the fluid content of the tissue Maintenance of the osmotic pressure They exert resistance towards deformation, thereby serving as regulators of the consistency of the connective tissue The important proteoglycans that are present in gingival connective tissue matrix are Chondroitin sulfate Hyaluronic acid
- 16. Any of a class of proteins which have carbohydrate groups attached to the polypeptide chain. Glycoproteins provide many functions : they give structural support to cells, help to form connective tissues. The important glycoproteins that are present in gingival connective tissue matrix are Elastin Fibronectin Laminin
- 17. The fibers of connective tissue can be divided into- Collagen The collagen fibers predominate in the gingival connective tissue and constitute the most essential components of the periodontium Reticular Present in epithelium connective tissue interface and endothelium connective tissue interface Elastic Present in association with the blood vessels Are absent in the gingiva coronal to the mucogingival junction Oxytalan Elaunin
- 18. The firmness is achieved by the gingival tissues that are composed of type I collagen Type III collagen is known as fetal collagen and is important in the early phases of wound healing and remains unmineralized. Collagen type VI is distributed with the elastin fibers along the blood vessels which imparts rigidity needed to maintain the elastic blood vessel wall from undergoing permanent deformation. The other collagen types associated with ECM are type II, V, X, XVIII which are dispersed along with type I collagen. The anchoring fibrils consisting of type VII collagen helps to reinforce epithelial attachment to the underlying tissue.
- 19. Densely packed collagen bundles that are anchored into the acellular extrinsic fiber cementum just below the terminal point of the junctional epithelium form the connective tissue attachment. The stability of this attachment is a key factor in limiting the migration of junctional epithelium. “Cho MI ,Garant “PR 2000
- 20. The connective tissue of the marginal gingiva is densely collagenous, containing a prominent system of collagen fiber bundles Classified into 3 groups : Gingivodental Circular Transseptal Page et al – 2 Groups Semicircular Transgingival
- 21. Periodontal ligament: The connective tissue that surrounds and attaches roots of teeth to the alveolar bone. (GTP 2001) Cellular element Extra cellular substance Fibers Ground substance
- 22. • Synthetic cells • Resorptive cells • Progenitor cells • Cells rests of Malassez • Defense cells CELLS • Fibers • Ground substances EXTRACELLULAR SUBSTANCES
- 23. 1. Synthetic cells. Fibroblasts Osteoblasts cementoblasts 2. Resorptive cells Osteoclasts cementoclasts 3. Progenitor cells 4. Epithelial rests of Malassez 5. Defense cells Neutrophils Lymphocytes Mast cells Macrophages Eosinophils
- 24. Periodontal ligament fibroblasts are large cells with an extensive cytoplasm The remodeling of collagen in the ligament is not confined to any intermediate zone, but occurs across the entire width of the ligament. Because of exceptionally high rate of turnover of collagen in the ligament, any interference in the fibroblast function by disease rapidly produces a loss of the tooth’s supporting tissue.
- 25. Functions Maintain the integrity of the lacunae and canaliculi. Open the channels for diffusion of nutrition through the bone. Play a role in removal or deposition of matrix and of calcium when required. Osteoblasts first migrate away from the bone surface into the body of periodontal ligament before eventually taking up their functional position. Osteoblasts form a cell layer over forming bone surface and act as barrier that control ion flux into out bone.
- 26. These are the cells responsible for secreting the organic matrix (mainly collagen) of cementum. As distinct layer of cells on the root surface, similar to osteoblastic layer but not regular in arrangement.
- 27. At such locations the cells occupy pits called Resorption bays or lacunae of howship. Osteoclasts are formed by fusion of mononuclear cells arising from bone marrow. They do not cover the whole of resorbing surface at any one time, rather they service a much larger area by demonstrating considerable motility.
- 28. These cells only occur in certain pathologic conditions, during resorption of deciduous teeth and when regressive forces are applied on a tooth such as orthodontic therapy. These Cementoclasts resembles Osteoclasts and are located in depressions in cementum resembling Howship’s lacuna. These cells not only resorb cementum, they can destroy dentin and enamel as well thus they are also called Odontoclasts.
- 29. If they were not present there would be no cells available to replace differentiated cells lying at the end of their life span or as a result of trauma. These are undifferentiated mesenchymal cells. These cell populations within the ligament appear to be in highest concentrations in locations adjacent to blood vessel and exhibit some of the classical cytological features .
- 30. At the time of cementum formation the continuous layer of epithelium that covers the surface of newly formed dentin breaks into lacelike stands . The epithelial rests persist as a network stands islands or tubelike structures near and parallel to the surface of the root . Their function is not clear but they could be involved in periodontal repair and generation . These cells rests can be distinguished from fibroblasts in pdl by the close packing of their cuboidal cells and their nucleus stains more deeply .
- 31. These cells may undergo calcification to become CEMENTICLES Loe and waerhaug (1960) After reimplantation studies observed that Ankylosis and subsequent root resorption never occurred when a periodontal ligament that contained epithelial cell rest was retained. These authors suggest that epithelial cell rest may be the factor in limiting the resorption and play a role in maintenance of periodontal space.
- 32. Neutrophils are the most abundant (40% to 75%) type of white blood cells in mammals and form an essential part of the innate immune system. Neutrophils are a type of phagocyte. Neutrophils are recruited at the site of injury within minutes following trauma, and are the hallmark of acute inflammation.
- 33. A lymphocyte is subtypes of white blood cell in a human’s immune system. These are agranulocytes. The three major types of lymphocyte are T cells, B cells and natural killer (NK) cells. Lymphocytes can be identified by their large nucleus.
- 34. Found in the ligament and are predominantly located adjacent to blood vessels. Are capable of phagocytosis. Derived from blood monocytes. It has a nucleus, horseshoe or kidney shaped with peripheral chromatin. .
- 35. These are relatively small round or oval cell having a diameter of about 12 to 15 um . These cells are characterized by numerous cytoplasmic granules called Histamine. Mast cells histamine plays a role in the inflammatory reaction and have been shown to degranulate in response to antigen – antibody reaction on their surface .
- 36. Occasionally seen in the periodontal ligament. These are granulocytes. They possess granules that consist of one or more crystalloid structures. The cells are capable of phagocytosis. Increases in case of parasitic infections.
- 37. Extracellular Substance Fibers collagen elastic reticular Ground Substances
- 38. The main types of collagen in the pdl are TYPE I and TYPE III. Type I is uniformly distributed in the ligament. Type IV and VII are associated with epithelial cell rests and blood vessels. A collagen subtype collagen XII which is a unique feature of periodontal ligament as it does not normally present in other soft tissues.
- 39. Collagen XII is thought to be involved in three dimensional architecture of periodontal ligament fibers Type XIII collagen is believed to occur within the pdl only when ligament is fully functional . Type XVIII collagen, which is a component of hemidesmosomes is also present in periodontal ligament along with the desmosomal complex of proteins.
- 40. There are three types of elastic fibers which are histochemically and ultrastructurally different. Mature Elastic fibers , Eulanin fibers and the Oxytalan fibers . Eulanin fibers and Oxytalan fibers have been described as immature elastic fibers. Mature elastic fibers consist of microfibrillar component surrounding an amorphous core of elastin protein .
- 41. These are immature collagen fibers with argyrophilic staining properties and are related to basement membrane of blood vessels and epithelial cells which lie within the periodontal ligament.
- 42. The collagen is gathered to form bundles approximately 5 um in diameter. These bundles are termed as PRINCIPAL FIBERS. Within each collagen bundle , subunits are present called collagen fibrils. Transseptal group Alveolar crest group Horizontal group Oblique group Apical group Interadicular group
- 43. The collagen bundles of the periodontal ligament are embedded into cementum and alveolar bone – similar to that of tendon inserting into bone. These fibers are called as Sharpey’s fibers. Some sharpey’s fibers are completely calcified but most contain an uncalcified central core within a calcified outer layer.
- 44. Glycosaminoglycans Hyaluronic acid Chondroitin sulfide Dermatan sulfate Proteoglycans Versican Decorin Fibromodulin and lumican Periostin Glycoproteins Fibronectin and laminin; Nidogen Vitronectin Tenascin Thrombospondin
- 45. Calcified, Avascular mesenchymal tissue that forms the outer covering of the anatomic root. Carranza 11th edition CLASSIFICATION ACELLULAR CEMENTUM CELLULAR CEMENTUM
- 46. SHROEDER & PAGE CLASSIFICATION -1986 1.Acellular Afibrillar Cementum (AAC) 2.Acellular Exrinsic Fiber Cementum (AEFC) 3.Cellular Intrinsic Fiber Cementum (CIFC) 4.Cellular Mixed Stratified Cementum (CMSC) 5.Intermediate Cementum
- 47. Chemical Composition 45-50 % Inorganic substances 50-55% Organic substances consists of calcium phosphate in the form of hydroxy-apatite crystals collagen fibers embedded in a ground substance . Protein Polysaccharides
- 48. Three types of cells are functionally concerned with cementum : BONE FORMING CELLS Cementoblasts Cementocytes BONE RESORPING CELLS Cementoclast
- 49. Arise from the undifferentiated mesenchymal cells Synthesise collagen and protein polysaccharides- organic matrix of cementum. Mitochondrea, golgi, RER Inner cells of dental follicle: CIFC HERS- AEFC
- 50. These locate in spaces termed lacunae & have numerous cytoplasmic processes coursing in canaliculi, that are preferentially directed towards the periodontal ligament. This is how cementocytes derive their nutrition from periodontal ligament & contribute to the vitality of this mineralized tissue. While adjacent canaliculi of neighboring cells communicate frequently, the processes remain independent. Thus, the metabolites progress mostly by diffusion through the canaliculi of cellular cementum.
- 51. They are multinucleated giant cells, which are indistinguishable from osteoclasts. Responsible for root resorption that leads to primary teeth exfoliation & also in the permanent dentition in mesial surfaces in compliance with mesial migration & may occur due to occlusal trauma & orthodontic therapy.
- 52. The organic matrix of cementum is composed primarily of collagen. Predominantly type I and type III (Birkedal and Hansen et al 1977) Type I collagen plays structural as well as morphogenic role and provides scaffolding for mineral crystals It is the major component accounting for 90% of organic components in cellular cementum.
- 53. The type III collagen, which coats type I collagen fibrils, accounts for only 5%. (Rao et al 1979, Wang et al 1980) It is a less cross-linked collagen found in high concentrations during development, repair and regeneration of mineralized tissues
- 54. Type XII collagen- A fibril associated collagen with interrupted triple helices that binds to type 1 collagen and also to non collagenous proteins Trace amounts of Type XIV are also found in extracts of mature cementum, however these may be contaminants from periodontal ligament. Based on immunostaining, the cementum does not appear to have either Type V or Type VI collagen (Becker and Romanos et al 1991)
- 55. Bone sialoprotein osteopontin Fibronectin Tenascin Osteonectin - SPARC(Specific Protein Acidic Rich in Cysteine) Proteoglycan Versican, decorin, biglycan, syndecan
- 56. Alveolar bone is defined as the parts of maxilla and mandible that form and support the socket of teeth. Together with the root cementum and periodontal ligament, the alveolar bone constitutes the attachment apparatus of the teeth
- 58. Derived from multipotent UNDIFFERENTIATED mesenchymal cells or alternatively from perivascular cells (PERICYTES). Secretes both “collagenous (type 1 collagen) and non collagenous” bone matrix – OSTEOID . Osteoblasts exhibit high level of alkaline phosphatase on their outer plasma membrane - believed to contribute - initiation of bone mineralization
- 59. Most abundant bone cells . Communicate with each other and with other cells on surface of the bone via dendritic process encapsulated in canaliculi Play role in calcium homeostasis Exchange of metabolic and biochemical messages occurs between blood stream and canaliculi
- 60. Generally occur in clusters. They have prominent mitochondria, lysozomes, vacuoles and few endoplasmic reticulum. Activity is controlled by PTH They are found against the bone surface, occupying shallow depressions called Howship’s lacunae surfaces or in deep resorption cavities called cutting cones.
- 61. Similar to osteocytes – i.e., osteoblasts that do not get embedded in newly formed bone ,gets adhered to the outer surface of the bone …..when bone formation halts.
- 62. Bone 33% organic 28% collagen 5% non collagenous proteins 67% inorganic Hydroxyapatite
- 63. Type I collagen makes up about 90% of the organic matrix. Type I collagen forms fiber bundles that provide basic structural integrity to bone. In addition to this type V, III & XII are also present. Type III collagen is present in relation to Sharpey’s fibers. Type I, V & XII are produced by osteoblasts and type III is produced by fibroblasts. The remaining 10% consists of non- collagenous components 80- 90% of organic component TYPE III & XII TYPE I TYPE V(5%)
- 64. Bone sialoprotein Osteonectin - SPARC(Specific Protein Acidic Rich in Cysteine) osteopontin Glycosaminoglycans Versican Decorin and biglycan Osteocalcin Bone morphogenic proteins
- 65. CONNECTIVE TISSUE IN DISEASE
- 66. Gingivitis – perivascular extracellular matrix – collagen within foci of inflammation is degraded. Cause – MMPs produced by PMNs. Periodontitis – MMPs by PMNs , macrophages , fibroblasts and keratinocytes. Foci of inflammation may ,manifest as scarring and fibrosis.
- 67. In gingiva – collagen becomes more soluble. Type I and III are lost at the foci of inflammation. Collagen ratios are altered. Type V increased and more than type III. New type Type I trimer are also found in inflammed gingiva.
- 68. Destruction carried out by MMPs especially from PMNs and macrophages. Imbalance between activated MMPs and endogenous inhibitors.- Reynolds and Meikle 1997 Proteoglycans are affected but the damage is less than that of collagen. Dermatan sulfate decreases Chondroitin sulfate increases.
- 69. Degradation of proteoglycan core proteins and hyaluronic acids are characteristic feature of inflammed gingival connective tissues. (Bartold and page 1986) PDL manifests changes in distribution of glycosaminoglycans Major change is increase in presence of chondroitin sulphate. Changes to the hard tissue matrix of bone and cementum differ significantly due to their different anatomical location.
- 70. Complication of medication Matrix elements are lost during gingivitis but accumulated in gingival overgrowth. Excessive accumulation of Connective tissues - especially collagen is affected. Types I , III , V and VI collagens and fibronectin are present. Collagen type I and type III ratio are altered. Collagen type III is increased.
- 71. In healthy – noncollagenous matrix 7 % In phenytoin induced overgrowth - 20 % Ballard and Butler 1974 Higher contents of hexosamine , uronic acid , glycosaminoglycans and proteoglycans , and also glucocorticoid receptors. Reason for accumulation in gingival overgrowth Decreased levels of matrix degrading enzymes in these lesions. Or induction of matrix production.
- 72. Age related changes Change occurs in collagen synthesis Decreased collagen sollubility Increased cross linking However collagens of gingiva and pdl – high turnover with advancing age. Type I and type III usually increases with age. Anticollagenase tissue inhibitor appears in lesion.
- 73. Mechanisms of periodontal tissue destruction Enzyme mediated damage by host cells Tissue degrading enzymes from bacterial cells Phagocytosis of matrix components Free radicals in tissue destruction Effect of Soluble mediators on connective tissue cells
- 74. MMPs – degrade interstitial or basement membrane collagens - laminin , fibronectin , core proteins of proteoglycan. Produced by PMNs , macrophages , fibroblasts , keratinocytes and endothelium. Activated by plasmin
- 75. Cell type MMP type Inducers Fibroblast MMP- 1 2 3 IL-A,B;TNF-A;PDGF Keratinocytes MMP – 1 2 9 10 LPS;TGF-A Monocytes,Endothel ial cells MMP – 1 2 3 9 LPS PMN MMP 8 9 LPS
- 76. Plasminogen – plasmin. Activated by u – PA ( Plasma membranes ) and t – PA ( fibrin surfaces ). At site of inflammation plasminogen activating system is high. Affects matrix macromolecules other than collagen . Also affects collagen by activating MMPs.
- 77. Inhibitors Alpha 1 proteinase inhibitor Alpha 2 macroglobulin Alpha 2 antiplasmin PAI 1 and PAI 2. PAI 2 is an important inhibitor of tissue proteolysis in periodontal tissues. (Kinnby 1994) In periodontitis plasmin is formed at sites of inflammation, activates the proMMPs into proteases which are specific for elastin and collagen, also responsible for the degradation of fibrin and extracellular matrix (ECM) Buduneli N, 2005
- 78. Microbial collagenases Enzymes with trypsin like activities. Regulates MMPs by activating them or degrades the inhibitors. Acts as antigens – cytokine production Inflammed gingiva – hydrolytic enzymes beta glucuronidase , aryl sulfatase , hyaluronidase , chondroitinase. The substrate for above enzymes are hyaluronan and proteoglycan. Breakdown of glycosaminoglycan chains.
- 79. Fibroblasts and macrophages – degradative pathway for collagen. Requisite – proteolytic digestion prior to cell ingestion of collagen. Phagosome + lysosome (cathepsin L) Cells defective in phagocytic process may lead to tissue overgrowth. Mechanism still unclear.
- 80. ROS high in cells undergoing respiratory bursts. Consequence of electron transport chain or metabolism. MPO and NADPH Arachidonic acid metabolism Tissue destruction when produced in excess.
- 81. Superoxide radical – direct toxic action on cells. Pathogenesis of inflammation induced tissue destruction. Hydroxyl radical – short lived , hydrogen peroxide –long lived. HOCL – activation of collagenases and gellatinases. Potential to play role in matrix destruction in inflammed periodontitis. Eg oxygen derived free radial may depolymerize gingival proteoglycans and hyaluron , activate neutrophil collagenase , and thus initiate matrix degradation. (sorsa 1989)
- 83. THANK YOU
Notas del editor
- DEFINITIONS Is the part of oral mucosa that covers the alveolar processes of jaw and surrounds the neck of teeth. Carranza Is that part of masticatory mucosa covering alveolar processes and the cervical portions of teeth. Lindhe A PAPILLARY LAYER subjacent to the epithelium which consists of papillary projections between the epithelial retepegs A RETICULAR LAYER contiguous with the periosteum of alveolar bone
- An ability for site directed migration (chemotaxis) Attachment to various substrata Gingival fibroblasts are phenotypically heterogeneous, and these fibroblast subpopulations may play different roles in tissue maintenance, regeneration and pathologies. They have a typical elongated or spindle shape and, consistent with their high level of synthetic activity, have prominent rough endoplasmic reticulum and golgi apparatus. Their cytoplasm is usually rich in numerous mitochondria vacuoles and vesicle. As with connective tissue elsewhere in the body,fibroblasts synthesize collagen and elastic fibers, as well as the glycoproteins and glycosaminoglycans of the amorphous intercellular substance. Apart from regulating matrix synthesis and remodelling, fibroblasts possess two other properties critical to their function An ability for site directed migration (chemotaxis) Attachment to various substrata
- bone-marrow-derived, granule-containing immune cells that are found in all connective tissue Mast cells are able to phagocytose, process and present antigens as effectively as macrophages. In human periodontal disease there is an increase in the number of mast cells that may be participating either in the destructive events or in the defense mechanism of periodontal disease via secretion of cytokines.
- Macrophages are professional phagocytes and are highly specialized in removal of dying or dead cells and cellular debris. When a macrophage ingests a pathogen, the pathogen becomes trapped in a phagosome, which then fuses with a lysosome. Within the phagolysosome, enzymes and toxic peroxides digest the pathogen. Macrophages are versatile cells that play many roles. As scavengers, they rid the body of worn-out cells and other debris. Along with dendritic cells, they are foremost among the cells that present antigens, a crucial role in initiating an immune response. As secretory cells, monocytes and macrophages are vital to the regulation of immune responses and the development of inflammation; they produce a wide array of powerful chemical substances (monokines) including enzymes, complement proteins, and regulatory factors such as interleukin-1. At the same time, they carry receptors for lymphokines that allow them to be "activated" into single-minded pursuit of microbes and tumour cells. Macrophages are essential for wound healing.[20] They replace polymorphonuclear neutrophils as the predominant cells in the wound by two days after injury.[21] Attracted to the wound site by growth factors released by platelets and other cells, monocytes from the bloodstream enter the area through blood vessel walls.[22] Numbers of monocytes in the wound peak one to one and a half days after the injury occurs. Once they are in the wound site, monocytes mature into macrophages. The spleen contains half the body's monocytes in reserve ready to be deployed to injured tissue In spite of a spectrum of ways to activate macrophages, there are two main groups designated M1 and M2. M1 macrophages, M1 "killer" macrophages are activated by LPS and IFN-gamma, and secrete high levels of IL-12 and low levels of IL-10. In contrast, the M2 "repair" designation (also referred to as alternatively activated macrophages) broadly refers to macrophages that function in constructive processes like wound healing and tissue repair, and those that turn off damaging immune system activation by producing anti-inflammatory cytokines like IL-10. These histiocytes are part of the immune system by way of two distinct functions: phagocytosis and antigen presentation. Phagocytosis is the main process of macrophages and antigen presentation the main property of dendritic cells (so called because of their star-like cytoplasmic processes).
- Proteoglycans describe a family of macromolecules composed of one or more glycosaminoglycans covalently bound to protein core.
- Chondroitin sulfide is a proteoglycan that occupies a large solvent space in the interstitial spaces of the extracellular matrix. It is composed of disaccharide units of „O‟ sulfated N-acetyl galactosamine and D-glucoronic acid. The sulphation may take place at the C-4 and C-6 of the N-acetyl galactosamine. Accordingly, the molecule is termed as chondroitin-4-sulfate, chondroitin-6-sulfate.Their concentration is greatest in mineralized tissues, for example cartilage and bone.16 Hyaluronic acid is a large glycosaminoglycan present in most connective tissues and is especially abundant in embryonic tissues and cartilage.17The functions of hyaluronic acid are tissue hydration, cell- surface matrix interactions, tissue development, cell-migration, aggregation with aggrecan, CD44 and other components of matrix.18
- . FN may influence the migration of fibroblasts and play a crucial role inmaintaining structural integrity of CT Plays a role in the alignment of collagen fibers Elastin is a rubber like protein secreted by fibroblasts and smooth muscle cells. Elastin aids the blood wall vessel to expand and to facilitate an increase in the volume of blood. Elastin is a negligible component of gingival connective tissue and accounts about 6% of the total tissue protein. Ultrastructurally, elastin fibers composed of two morphologic components: an amorphous elastin component constituting 90% of the mature fiber and a 10 to 12nm diameter microfibrillar component. For an elastic fiber to form, the glycoproteins and several microfibril associated glycoproteins are initially secreted and accumulated into microfibrils. The microfibrils then provide a scaffold for the deposition of elastin and assembly of elastic fibers. Immature elastic fibers consisting only of microfibrillar subunits are referred to as oxytalan fibers.11 Fibronectin is a chief glycoprotein present in gingival connective tissue. It is produced by hepatocytes and fibroblasts and is considered as a principal protein of ECM as it binds the cells to the ECM essential for connective tissue turnover in the gingiva. Fibronectin is a large dimer of two similar 230-270 Kd polypeptide subunits which are connected by disulfide bonds at the C-terminus. Through these associations, fibronectin is involved in the cell attachment, migration, differentiation, and growth.12, 13 . It is a large glycoprotein (900 kDa) containing 3 polypeptide chains linked by disulfide bonds to form an asymmetric cross-structure. It is produced by the epithelial cells and helps attachment to the type IV collagen of the lamina densa layer through nidogen. In embryonic tissues, laminin is the first extracellular protein noticed, and in mature tissues it is commonly found as the major non-collagen component in basement membranes. The laminins are involved in a variety of biological functions, including cell attachment, cell proliferation and cell differentiation
- The collagen fibers predominate in the gingival connective tissue and constitute the most essential components of the periodontium. Cementoblasts and osteoblasts are cells which also possess the ability to produce collagen. RETICULIN FIBERS: Present in epithelium connective tissue interface and endothelium connective tissue interface ELASTIC FIBERS: Present in association with the blood vessels Are absent in the gingiva coronal to the mucogingival junction OXYTALAN FIBERS Are scarce in gingiva and are immature fibers Present numerously in periodontal ligament Course mainly parallel to long axis of tooth ELAUNIN
- functions
- Compared with most connective tissues, the periodontal ligament is highly cellular.
- Most predominant cell type of periodontal ligament. Found between the fibers of the periodontal ligament, where they are surrounded by fibers & ground substance. STRUCTURE: Ovoid or elongated cells oriented along the principal fibres. Large cells with an extensive cytoplasm Associated with protein synthesis & secretion (e.g. RER, several Golgi complex, & many secretary vesicles) (11) They have a well-developed cytoskeleton . Adherens and gap junctions, reflecting the functional demands placed on the cells. Aligned along the general direction of the fiber Extend cytoplasmic processes that wrap around them. The collagen fibrils of the bundles are continuously being remodeled by the fibroblasts.
- Bone forming cells derived from osteoprogenitor cells. Responsible for laying down the organic matrix of bone including the collagen fibers. Alkaline phosphatase present in osteoblasts is responsible for its mineralization
- These resorb bone and tend to be large and multinucleated but can also be small and mononuclear . Multinucleated osteoclasts are formed by fusion of precursor cells similar to circulating monocytes. These when viewed in light microscope are cells occupy bays in bone or surround end of bone spicule . The part of plasma membrane lying adjacent to bone that is being resorbed is raised in characteristic folds and is termed the ruffled or striated border. The ruffled border is separated from the rest of plasma membrane by a zone of specialized membrane that is closely applied to the bone the underlying cytoplasm of which tends to be devoid of organelles and has been called the clear zone . The area of bone that is sealed off by virtue of active pumping of protons by the osteoclast into this environment .
- The ligament contains epithelial cells that are found close to the cementum . They are more numerous in older individuals and more numerous in children . These cells may proliferate to form cysts and tumors. These cells may undergo calcification to become CEMENTICLES
- In periodontal ligament macrophages play dual role:- 1. Phagocytosing dead cells 2. Secreting growth factor that regulate the proliferation of adjacent fibroblasts
- More than 70 % of pdl is TypeI . Type III collagen accounts for about 20 % of collagen fibers
- Oxytalan fibers are bundles of microfibrills. These fibers are approximately 0.5μm to 2.5 μm in diameter. They tend to run in axial direction one end being embedded in cementum or possibly bone, and other in the wall of blood vessels. They have found to be thicker and more numerous in teeth that are subjected to high load.
- Transseptal group : These fibers extend inter proximally over the alveolar crest and are embedded in the cementum of adjacent teeth. They are reconstructed even after destruction of the alveolar bone has occurred in periodontal disease. Resist tooth separation, mesial or distal. Alveolar crest group: Alveolar crest fibers extend obliquely from the cementum just beneath the junctional epithelium to the alveolar crest. Fibres also run from the cementum over alveolar crest and to the fibrous layer of the periosteum covering alveolar bone They prevent the extrusion of teeth and resist lateral movements of tooth.(7) Their incision does not significantly increase tooth mobility. Horizontal group These group of fibers extend at right angles to the long axis of the tooth from -> the cementum to the alveolar bone. Resist horizontal and tipping forces. Oblique Group Oblique fibers, the largest group in the periodontal ligament, extend from the cementum in a coronal direction obliquely to the bone. They bear the brunt of vertical masticatory stress and transform them into tension on to the alveolar bone. It is the largest prinicpal fibre group They resist apically directed masticatory forces Apical group The apical group radiate from the cementum to the bone at the fundus of the socket. They do not occur on incompletely formed roots. Functions- They prevent tooth tipping,resist forces of luxation . Inter radicular fibers These fibers fan out, from the cementum to the teeth on the furcation areas of multirooted teeth. They resist forces of luxation and roatation.
- These fibers level to concentrate on the crestal region. Orientation is similar to that of adjacent periodontal ligament bundles. The Bone adjacent to the periodontal ligament that contains a great number of sharpeys’ fibers are called as Bundle bone.
- Cementum is a mesenchymal tissue that covers the root surface of the tooth. It enables attachment for the periodontal ligament to the root surface and hence an integral part of periodontium
- In the apical 1/3rd,cementoblasts trapped in rapidly calcifying cemental matrix, later, differentiate into cementocytes
- Osteoblasts secrete type I collagen, small amount of type V collagen, osteonectin, osteopontin, RANKL, osteoprotegerin, Proteoglycans, latent proteases and growth factors including bone morphogenic proteins. Osteoblasts exhibit high levels of alkaline phosphatase -cytochemical marker. Bone resorbing factors that act via the osteoblast are parathyroid hormone, vitamin D3, interlukin -1 and tumor necrosis factor. RANKL - osteoclast differentiation Cbfa1 - regulates the expression of OPG (osteoprotegerin).
- Osteoblasts flatten, when bone is not forming and extend along the bone surface and hence the name. They are present on periosteal as well as endosteal surfaces
- RANKL/OPG balance is an important factor in regulating bone resorption in periodontal and periapical environments. Osteoclast differentiation and activation are driven by the interaction of RANK (receptor activator of nuclear factor-kB) with its ligand, RANKL. Osteoprotegerin, OPG, is a decoy receptor of RANKL that inhibits RANK-RANKL engagement. In homeostatic conditions (left side), RANKL and OPG levels are thought to be in balance so that there is limited osteoclastogenesis and bone resorption. With an inflammatory stimulus, the RANKL/OPG ratio increases in periodontal and periapical tissues and leads to stimulation of osteoclast activity and pathologic bone resorption.
