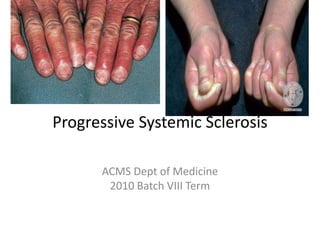
Progresive systemic sclerosis
- 1. Progressive Systemic Sclerosis ACMS Dept of Medicine 2010 Batch VIII Term
- 2. PSS: Definition • Systemic sclerosis (previously called 'scleroderma') is a generalised disorder of connective tissue affecting- • The skin • Internal organs and • Vasculature.
- 3. PSS: Hallmark The clinical hallmark is the presence of • Sclerodactyly in combination with • Raynaud's phenomenon or • Digital ischaemia
- 4. PSS: Epidemiology • The peak age of onset is in 4th & 5th decades • Overall prevalence is 10-20 per 100 000 • 4:1 female: male ratio
- 5. PSS: Classification It is subdivided into • Diffuse cutaneous systemic sclerosis (DCSS) • Limited cutaneous systemic sclerosis (LCSS) • Many patients with LCSS have features which are phenotypically grouped into the 'CREST' syndrome (calcinosis, Raynaud's, oesophageal involvement, sclerodactyly, telangiectasia).
- 6. PSS: Classification It is subdivided into • Diffuse cutaneous systemic sclerosis (DCSS) • Limited cutaneous systemic sclerosis (LCSS) • Many patients with LCSS have features which are phenotypically grouped into the 'CREST' syndrome (calcinosis, Raynaud's, oesophageal involvement, sclerodactyly, telangiectasia).
- 10. PSS: Etiopathology • Unknown, • No consistent genetic, geographical or racial associations. • Environmental factors are important in isolated cases that result from exposure to –silica dust, –vinyl chloride, –hypoxy resins and –trichloroethylene.
- 11. PSS: Etiopathology Early in the disease there is • Skin infiltration by T lymphocytes • Abnormal fibroblast activation • That leads to increased production of extracellular matrix in the dermis, primarily type I collagen. • This results in symmetrical thickening, tightening and induration of the skin (sclerodactyly).
- 12. PSS: Etiopathology Early in the disease there is –Skin infiltration by T lymphocytes and –Abnormal fibroblast activation • In addition to skin changes there is arterial and arteriolar narrowing due to intimal proliferation and vessel wall inflammation. • Endothelial injury causes release of vasoconstrictors and platelet activation, resulting in further ischaemia.
- 13. PSS Clinical Features and Diagnoais • Systemic sclerosis is predominantly a clinical diagnosis based on the presence of sclerodactyly. • Most patients are ANA-positive, and • Approximately 30% of patients with diffuse disease and • 60% with limited disease have antibodies to topoisomerase 1 and centromere respectively.
- 14. • Cutaneous changes Raynaud's phenomenon is universal and may precede other clinical features.
- 15. • Systemic sclerosis. Hands showing tight shiny skin, sclerodactyly, flexion contractures of the fingers and thickening of the left middle finger extensor tendon sheath
- 16. PSS: Skin Disease • The initial phase of skin disease is characterised by non-pitting oedema of the fingers and flexor tendon sheaths. • Subsequently, the skin becomes shiny and taut, and distal skin creases disappear. • There is usually erythema and tortuous dilatation of capillary loops in the nail-fold bed, readily visible with an ophthalmoscope. • The face and neck are usually involved next, with thinning of the lips and radial furrowing. In some patients skin thickening stops at this stage.
- 17. PSS: Skin Disease • Skin involvement restricted to sites distal to the elbow or knee (apart from the face) is classified as 'limited cutaneous disease' or CREST syndrome. • Involvement proximal to the knee and elbow and on the trunk is classified as 'diffuse cutaneous disease'.
- 18. PSS: Skin Disease In extremities- • Intimal fibrosis and vessel wall inflammation may combine to cause critical tissue ischaemia, skin ulceration on pressure points • Localised areas of infarction and • Pulp atrophy at the fingertips.
- 19. PSS: Musculoskeletal features • Arthralgia, morning stiffness and flexor tenosynovitis are common. • Restricted hand function is due to skin rather than joint disease and erosive arthropathy is uncommon. • Muscle weakness and wasting are usually due to myositis.
- 20. PSS: GI FEATURES • Gut involvement is common. • Smooth muscle atrophy and fibrosis in the lower two-thirds of the oesophagus lead to acid reflux with erosive oesophagitis. • Since this may progress to further fibrosis, adequate treatment of reflux (proton pump inhibitors) is important. • Dysphagia and odynophagia (painful dysphagia) may also occur.
- 21. PSS: GI FEATURES • Involvement of the stomach causes early satiety and occasionally outlet obstruction. • Recurrent occult upper GI bleeding may indicate a 'watermelon stomach' (antral vascular ectasia), which occurs in up to 20% of patients. • Small intestine involvement may lead to malabsorption, bacterial overgrowth and intermittent bloating, pain or constipation. • Dilatation of large or small bowel due to autonomic neuropathy may cause pseudo- obstruction.
- 23. PSS: Cardiorespiratory features • Pulmonary involvement is a major cause of morbidity and mortality. • Fibrosing alveolitis mainly affects pts with diffuse disease, esp those with antibodies to topoisomerase 1. • Pulmonary hypertension is a long-standing complication. It is 6X more prevalent in limited than diffuse disease. • The clinical features are rapidly progressive dyspnoea (more than ILD), RHF and angina with- • often rapidly progressing digital ischaemia.
- 24. PSS: Cardiorespiratory features Treatment strategies include • Vasodilators • Continuous infusions of epoprostenol • The oral endothelin 1 antagonist bosentan and • Heart-lung transplantation.
- 25. PSS: Renal features • Main cause of death is hypertensive renal crisis (rapidly developing malignant hypertension and renal failure). • Treatment is by ACE inhibition even in presence of renal impairment. • Hypertensive renal crisis is more likely in patients with diffuse rather than limited disease. • It is also more prevalent in patients with topoisomerase 1 antibodies. • Clinicians use prophylactic ACE Is for diffuse disease to prevent this manifestation.
- 26. PSS: Management and prognosis Five-year survival is approx70%. Risk factors for a poor prognosis include • Older age • Diffuse skin disease • Proteinuria • High ESR • A low gas transfer factor for carbon monoxide (TLCO) and • Pulmonary hypertension
- 27. PSS: Management and prognosis • Self-management to maintain core body temperature and avoid peripheral cold exposure is important. • Infection of ulcerated skin should be treated with prompt antibiotic therapy. • Antibiotics penetrate poorly into the skin lesions of systemic sclerosis and therefore need to be given at higher dose for longer periods (e.g. flucloxacillin 500 mg 6-hourly for 14 days).
- 28. PSS: Management and prognosis • Calcium antagonists (e.g. nifedipine, amlodipine) or angiotensin II receptor antagonists (e.g. valsartan) may be effective for Raynaud's symptoms. • For severe digital ischaemia, intermittent infusions of epoprostenol may be helpful.
- 29. PSS: Management and prognosis • Corticosteroids and cytotoxic drugs are indicated in patients with myositis or alveolitis. • No agent has been shown to arrest or improve skin changes.
Notas del editor
- P450, a mechanism that is less likely to produce toxic intermediates. Adva-27a is an excellent inhibitor of Topoisomerase II with an IC50 of ... Topoisomerases (type I: EC 5.99.1.2, type II: EC 5.99.1.3) are enzymes that regulate the overwinding or underwinding of DNA. The winding problem of DNA ...
