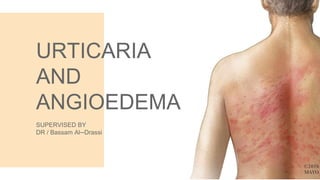
Urticaria
- 1. URTICARIA AND ANGIOEDEMA SUPERVISED BY DR / Bassam Al─Drassi
- 2. URTICARIA AND ANGIOEDEMA Urticaria is composed of wheals (transient edematous papules and plaques, usually pruritic and caused by edema of the papillary body), The wheals are superficial and well defined. Angioedema is a larger edematous area that involves the dermis and subcutaneous tissue and is deep and ill defined. Urticaria and angioedema are thus the same edematous process but involve different levels of the cutaneous vascular plexus: papillary and deep. Urticaria and/or angioedema may be acute recurrent or chronic recurrent. Definition Is avascular reaction of the skin it is a common skin disease characterized by wheals(red or white) associated with the sensations of itching or burning .
- 3. Incidence : 15-23% of the population may have had this condition during their lifetime. Urticaria/angioedema is not a disease but a cutaneous reaction pattern Epidemiology URTICARIA AND ANGIOEDEMA
- 4. Immunologic lgE-medlated urticarial Complement-mediated urticaria Autoimmune urticaria Immune contact urticaria Physical Dermographism Cold urticaria Solar urticaria Cholinergic urticaria Pressure angioedema VIbratory angioedema Classification Urticaria due to mast cell- releasing agents Pseudoallergens ACE Inhibitors Nonimmune contact urticaria Idiopathic urticaria Urticaria associated with vascular / connective tissue autoimmune disease
- 5. Urticaria is mediated through immune (allergic) or nonimmune mechanisms. Lesions result from the release from mast cells of biologically active substances, particularly histamine, which produce vasodilatation and increased vascular permeability. Several pathways are recognized: IgE-mediated (type I) hypersensitivity is the best understood mechanism; antigen cross-links immunoglobulin (Ig) E molecules on the surface of mast cells, resulting in degranulation with release of vasoactive agents. Complement activation can produce dermal oedema, as in hereditary angioedema or urticaria associated with circulating immune complexes. Direct release of histamine from mast cells, in a nonimmune manner, is caused by some drugs, e.g. opiates and contrast media. Blocking of the prostaglandin pathway from arachidonic acid, by some drugs such as aspirin and non-steroidal anti-inflammatory agents, promotes urticaria by accumulating vasoactive leukotrienes. Pathogenesis URTICARIA AND ANGIOEDEMA
- 6. 1. Drugs: are the most frequent cause of acute urticaria, penicillin & related antibiotics are the most frequent offenders. Urticaria reaction can occur 14 days after course of treatment has stopped. Non allergic release of Histamine by (asprin, NSAIDs, opiates, polymyxin,ciprofloxacin, rifampicin, vancomycin). 2. food: are a frequent cause of acute urticaria where as in chronic urticaria is less frequent factor. The most allergic foods are chocolate, shellfish, nuts, peanuts, tomatoes, strawberries, melons, cheese, garlic, onions, eggs, milk, and spices. 3. Food additives: natural food addictives synthetic additives Etiological factors URTICARIA AND ANGIOEDEMA
- 7. 4. Infections"acute urticaria may be associated with upper respiratory tract infections, especially streptococcal infections . Localized infections in tonsils, tooth, sinuses, prostate, urinary bladder and kidney ."Chronic viral infections such as hepatitis B & C" Helimenthes may cause urticaria these are (ascaris, ankylostomas, strangyloids, filarial, echinococcus schistosoma & liver flukes 5. Emotional stress:Persons under sever emotional stress may have more marked urticana. 6. Menthol: It is found in mentholated cigarettes, candy, cough drops, aerosol sprays & topicalmedications. 7.Neoplasms:Urticana has been associated with carcinoma & Hodgkin's diseases . URTICARIA AND ANGIOEDEMA Etiological factors
- 8. 8. Inhalants:Grass pollens, house dust mites , formaldehyde . 9. Alcohol:The mechanisms of indirect mast cell stimulation are unknown. 10. Hormonal causes:- Endocrine tumors Ovarian pathology Oral contraceptive use 11. Physical causes (physical urticaria):Cold, pressure, vibration, cholinergic (triggered by heat, exercise or emotional stress), sunlight, water, exercise. Etiological factors URTICARIA AND ANGIOEDEMA
- 9. Clinical manifestation Skin lesion Sharply defined wheals , small <1cm to large >8cm, erythematous or white with an erythematous rim, round, oval, , annular, serpiginous caused by confluence and resolution in one area and progresslon In another . Iesions are pruritic and transient.
- 10. Angioedema skin colored, transient enlargement of portion of face (eyelids, Ups, or tongue ) and Drug induced angioedema extremity, or other sites resulting from subcutaneous edema. Clinical manifestation Diatribation Usually regional or generalized. Locallzed in solar, pressure, vibration and cold urticaria/angioedema and contined to the site of the trigger mechanism .
- 11. Clinical types Evolves over days to weeks < 6 w . Acute onset and recurring over <30 days . Usually large wheals are often associated with angioedema often IgE dependent with atopic diathesis related to foods, parasites, and penicillin. Also, complement mediated in serum sickness like reactions (whole blood Immunoglobulins and penicillin). ACUTE URTICARIA
- 12. Urticaria and / or angioedema alasting more than 6 weeks Recurring over > 30 days. Small and latge wheals . Rarly IgE ddependent. Etiology unknown In 80% and therefore oonsidered idiopathic. Chronic idiopathic urticaria affects adults predominantly and is approximately twice as common in women as In men. Up to 40% of patients with chronic urticaria of >6 months' duration still have urticaria 10 years later. Clinical types CHEONIC URTICARIA
- 13. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS IgE Medlated Lesions in acute IgE-mediated urticaria result from antigen induced release of biologically active molecules from mast cells . Released mediators increase venular permeability and modulate the release of biologically active molecules from other cell types. Often with atopic baclcground. Antigens: food (milk. eggs. wheat. shellfish, nuts),therapeutic agents, drugs. Immunologic Urticaria Complement Mediated Acute urticarial . By way of immune complexes activating complement and releasing anaphylatoxins that induce mast cell degranulation. Serum sickness, administration of whole blood and immunoglobulins.
- 14. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS Autoimmune Common, chronic. Autoantibodies against IgE. Positive autologous serum skin test. Clinically, patients with these autoantibodies . Immunologic Urticaria Immunologic Contact Urticaria Usually in children with atopic dermatitis sensitized to invironmental allergens (grass and animals) .
- 15. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS Dermographism Linear urticarial lesions occur after stroking or scratching the skin. They itch and fade in 30 min. About 4.2% of the normal population have it. Physical urticaria
- 16. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS Cold Urticaria Usually in children or young adults . Urticarial lesions confined to sites exposed to colcd occurring within minutes after rewarming. "Ice cube" test (application of an ice cube for a few minutes to skin) causes wheal. Physical urticaria
- 17. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS Solar Urticaria Is a rare allergic reaction to sun exposure. The condation causes an itchy rash or hives that appear on any skin that has been exposed to sun. The more skin that is exposed to sunlight , the more reaction will be. Histamine is one of the mediators. Physical urticaria
- 18. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS Cholinergic urticaria Exercise to the point of sweating provokes typical small, papular, highly pruritic urticarial lesion . Occurring within 30 min of vigorous exercise . May be accompanied by wheezing. Physical urticaria
- 19. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS Pressure Angioedema Erythematous swelling induced by sustained pressure (buttock swelling when seated, hand swelling after hammering, foot swelling after walking). Delayed (30 min to 12 h). Painful . May persist for several days, and interferes with quality of life. No laboratory abnormalities, fever may occur. Physical urticaria
- 20. SPECIAL FEATURES/AS RELATED TO PATHOGENESIS VIbration Angioedema May be familial (autosomal dominant) or sporadic. Rare , it is believed to result from histamine release from mast cells caused by a vibrating stimulus rubbing a towel across the back produces lesions. But direct pressure (without movements) does not. Physical urticaria
- 21. Pseudoallergens agents Urticaria/angioedema and even anaphylaxis like symptoms may occur with radio contrast media and as a consequence of intolerance to salicylatcs, fuod preservatives and additives (e.g benzo:lc acid and sodium benzoate) Also to ACE inhibitors. Urticaria due to mast cell-releasing agents Histamine derived from mast cells In the skin is considered the major mediator. Caused by direct effects of exogenous urticants penetrating into skin or blood vessels. Localized to the site of contact. Sorbic acid, benzoic acid in eye solutions and foods. URTICARIA AND ANGIOEDEMA Chronic idiopathic urticaria Nonimmune contact urticaria
- 22. Urticarial lesions may be associated with systemic lupus erythematous and Sjogren syndrome. However, in most instances, they represent Urticarial vasculitis Urticaria associated with vascular/connective tissue autoimmune disease Urticarial vasculitis Urticarial vasculitis often has an acute onset with widespread urticarial lesions that are unusual as they persist for more than 24 h and fade leaving purpura. Systemic abnormalities and low complement levels may be found._ URTICARIA AND ANGIOEDEMA
- 23. Diagnosis URTICARIA AND ANGIOEDEMA Questions to be asked to a patient with urticarial: Are the Hives associated with any foods or new foods added? Is the patient take any regular medication or have any new medicines, ask about (aspirin, NSAIDs, antibiotics). Does the patient have any recent or chronic infections. Are the Hives caused by physical stimuli (heat,cold,pressure). Does the patient have any chronic medical conditions. Is the urticaria associated with substances inhaled. Is the urticaria associated with insect bites.
- 24. Wheals + angioedema Duration of individual hive 4 h-36 h 24-48 h with either bruising, severe arthralgia, fever, C4 30 min to 2 h History physical Stimulus physical challenge Phyaical urticaria Course > 6 wk Course < 6 wk Consider drugs, foods, food skin testing. Infection(partIculary inchildren) Other identifiable stimulus Thyroid functionTests Anti-microsomal antibody Antithyroglobulin antibody Autologous skin test In vttro-antl-lgE receptore Acute urticaria / angioedema Positive Negative Chronic autoimmune urticaria Chronic Idiopathic urticaria Skin biopsy Positive Urticarial vaecutltla Diagnosis
- 25. Diagnosis URTICARIA AND ANGIOEDEMA LABORATORY EXAMINATIONS SEROlOGY hcraeS rof Hepatitis B-associated antigen . Assessment of the complement system. Assessment of specific lgB antibodies . Serology for lupus and Sjogren syndrome . HEMATOLOGY The erythrocyte sedimentation rate (BSR) is often elevated in urticarial vasculitis , and there may be hypocomplementemia . Transient eosinophilia in urticaria from reactions to foods, parasites, and drugs .
- 26. Diagnosis URTICARIA AND ANGIOEDEMA LABORATORY EXAMINATIONS COMPLEMENT STUDIES Screening for functional C1 inhibitor in HAE . ULTRASONOGRAPHY For early diagnosis of bowel involvement in HAE If abdominal pain is present, this may indicate edema of the bowel . PARASITOLOGY Stool specimen for presence of parasites .
- 27. Course URTICARIA AND ANGIOEDEMA The course of an urticarial reaction depends on its cause. If the urticaria is allergic, it will continue until the allergen is removed, tolerated or metabolized. Most such patients clear up within a day or two, even if the allergen is not identified. Urticaria may recur if the allergen is met again.
- 28. Complications URTICARIA AND ANGIOEDEMA Urticaria is normally uncomplicated. Although its itch may be enough to interfere with sleep or daily activities and to lead to depression. In acute anaphylactic reactions oedema of the larynx may lead to asphyxiation. Oedema of the trachea bronchial tree may lead to asthma.
- 29. TREATMENT URTICARIA AND ANGIOEDEMA LEARNING POINTS The treatment of choice is to find the cause and eliminate it. You can learn more about the cause from the history than from tests. Most patients with hives clear up quickly even if the cause is not obvious. Use antihistamines in relatively high doses. Avoid aspirins and systemic steroids in chronic urticaria. Do not promise patients that all will be solved by allergy tests.
- 30. TREATMENT URTICARIA AND ANGIOEDEMA In general, antihistamines are the mainstays of symptomatic treatment . Cetirizine 10 mg/day and loratadine 10 mg/day, both with half-lives of around 12 h, are useful. If necessary, these can be supplemented with shorter acting antihistamines, e.g. hydroxyzine 10–25 mg up to every 6 h and acrivastine 8 mg three times daily. Alternatively they can be combined with a longer acting antihistamine as chlorpheniramine 12 mg sustained release tablets every 12 h.
- 31. TREATMENT URTICARIA AND ANGIOEDEMA H2-blocking antihistamines (e.g. cimetidine) may add a slight benefit if used in conjunction with an H1 histamine antagonist. Chlorpheniramine or diphenhydramine are often used during pregnancy because of their long record of safety but cetirizine, loratidine and mizolastine should be avoided. A tapering course of systemic corticosteroids may be used, but only when the cause is known and there are no contraindications
- 32. Some types of urticaria and their management Cold urticarial Avoid cold Protective clothing Antihistamines Solar urticarial Avoid sun exposure Protective clothing Sunscreens and sun blocks Beta-carotene Antihistamines Cholinergic urticarial Avoid heat Minimize anxiety Avoid excessive exercise Anticholinergics Antihistamines Tranquillizers Dermographism Avoid trauma Antihistamines Hereditary angioedema Avoid trauma Attenuated androgenic steroids as prophylaxis Tracheotomy may be necessary Hypersensitivity urticarial Remove caus Antihistamines (H1 + H2) Sympathomimetics Systemic steroids (rarely justified) Avoid aspirin-containing drugs