Diagnosis of vasculitides and pseudovasculitides. A quick reference guide. Mikhail Valivach. Pavlodar. 2015.
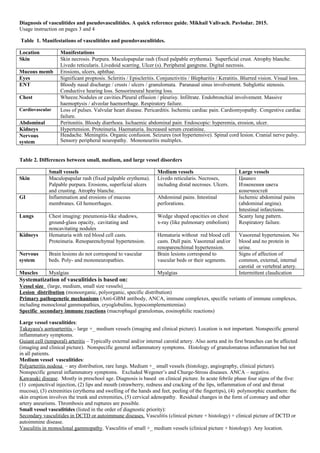
- 1. Diagnosis of vasculitides and pseudovasculitides. A quick reference guide. Mikhail Valivach, Murat Makatov. Pavlodar. 2015. Usage instruction on pages 3 and 4 Table 1. Manifestations of vasculitides and pseudovasculitides. Location Manifestations Skin Skin necrosis. Purpura. Maculopapular rash (fixed palpable erythema). Superficial crust. Atrophy blanche. Livedo reticularis. Livedoid scarring. Ulcer (s). Peripheral gangrene. Digital necrosis. Mucous memb Erosions, ulcers, aphthae. Eyes Significant proptosis. Scleritis / Episcleritis. Conjunctivitis / Blepharitis / Keratitis. Blurred vision. Visual loss. ENT Bloody nasal discharge / crusts / ulcers / granulomata. Paranasal sinus involvement. Subglottic stenosis. Conductive hearing loss. Sensorineural hearing loss. Chest Wheeze.Nodules or cavities.Pleural effusion / pleurisy. Infiltrate. Endobronchial involvement. Massive haemoptysis / alveolar haemorrhage. Respiratory failure. Cardiovascular Loss of pulses. Valvular heart disease. Pericarditis. Ischemic cardiac pain. Cardiomyopathy. Congestive cardiac failure. Abdominal Peritonitis. Bloody diarrhoea. Ischaemic abdominal pain. Endoscopic: hyperemia, erosion, ulcer. Kidneys Hypertension. Proteinuria. Haematuria. Increased serum creatinine. Nervous system Headache. Meningitis. Organic confusion. Seizures (not hypertensive). Spinal cord lesion. Cranial nerve palsy. Sensory peripheral neuropathy. Mononeuritis multiplex. Table 2. Differences between small, medium, and large vessel disorders Small vessels Medium vessels Large vessels Skin Maculopapular rash (fixed palpable erythema). Palpable purpura. Erosions, superficial ulcers and crusting. Atrophy blanche. Livedo reticularis. Necroses, including distal necroses. Ulcers. Цианоз Изменения цвета конечностей GI Inflammation and erosions of mucous membranes. GI hemorrhages. Abdominal pains. Intestinal perforations. Ischemic abdominal pains (abdominal angina). Intestinal infarctions. Lungs Chest imaging: pneumonia-like shadows, ground-glass opacity, cavitating and noncavitating nodules Wedge shaped opacities on chest x-ray (like pulmonary embolism) Scanty lung pattern. Respiratory failure. Kidneys Hematuria with red blood cell casts. Proteinuria. Renoparenchymal hypertension. Hematuria without red blood cell casts. Dull pain. Vasorenal and/or renoparenchimal hypertension. Vasorenal hypertension. No blood and no protein in urine. Nervous system Brain lesions do not correspond to vascular beds. Poly- and mononeuropathies. Brain lesions correspond to vascular beds or their segments. Signs of affection of common, external, internal carotid or vertebral artery. Muscles Myalgias Myalgias Intermittent claudication Systematization of vasculitides is based on: Vessel size (large, medium, small size vessels) Lesion distribution (monoorganic, polyorganic, specific distribution) Primary pathogenetic mechanisms (Anti-GBM antibody, ANCA, immune complexes, specific veriants of immune complexes, including monoclonal gammopathies, cryoglobulins, hypocomplementemias) Specific secondary immune reactions (macrophagal granulomas, eosinophilic reactions) Large vessel vasculitides: Takayasu's aortoarteritis – large +_ medium vessels (imaging and clinical picture). Location is not important. Nonspecific general inflammatory symptoms. Guiant cell (temporal) arteritis – Typically external and/or internal carotid artery. Also aorta and its first branches can be affected (imaging and clinical picture). Nonspecific general inflammatory symptoms. Histology of granulomatous inflammation but not in all patients. Medium vessel vasculitides: Polyarteritis nodosa – any distribution, rare lungs. Medium +_ small vessels (histology, angiography, clinical picture). Nonspecific general inflammatory symptoms. Excluded Wegener’s and Churge-Stross diseases. ANCA – negative. Kawasaki disease. Mostly in preschool age. Diagnosis is based on clinical picture. In acute febrile phase four signs of the five: (1) conjunctival injection, (2) lips and mouth (strawberry, redness and cracking of the lips, inflammation of oral and throat mucosa), (3) extremities (erythema and swelling of the hands and feet, peeling of the fingertips), (4) polymorphic exanthem: the skin eruption involves the trunk and extremities, (5) cervical adenopathy. Residual changes in the form of coronary and other artery aneurisms. Thrombosis and ruptures are possible. Small vessel vasculitides (listed in the order of diagnostic priority): Secondary vasculitides in DCTD or autoimmune diseases. Vasculitis (clinical picture + histology) + clinical picture of DCTD or autoimmine disease. Vasculitis in monoclonal gammopathy. Vasculitis of small +_ medium vessels (clinical picture + histology). Any location.
- 2. Monoclonal gammopathy revealed by electrophoresis. Goodpasture syndrome. Glomerulonephritis +_ pneumonitis. Other organs are not affected. Anti-GBM antibody. Vasculitis limited to gloneruli (glomerulonephritis). Histological proof. Immune deposits in immunofluorescence. Variants are determined in accordance with glomerulonephritis classification. Vasculitis limined to skin. Small +_ medium vessels. Histological proof. Variants include ANCA-associated and immune complex vasculitides. Isolated CNS vasculitis. Small +_ medium vessels. Angiography +_ histology. ANCA-negative. Henoch-Schonlein purpura (IgA vasculitis): Small +_ medium vessels (histology). Various distribution. Prevailing deposition of IgA (immunofluorescence). Wegener's granulomatosis. Small +_ medium vessels (histology). Various distribution with mandatory participation of upper or lower airways. In most patients ANCA-positivity. Immune deposits are not characteristic but if present do not exclude WG. Churge-Strauss syndrome. Small +_ medium vessels (histology). Various distribution with mandatory astma.Mandatory eosinophilia (in histology and/or in blood >10% and/or in sputum >25%)/ In most patients ANCA-positivity. Immune deposits are not characteristic but if present do not exclude CSS. Microscopic polyangiitis. Small +_ medium vessels (histology). Various distribution. No eosinophilia. No granulomatosis. Mandatory ANCA-positivity. Cryoglobulinemic vasculitis. Small +_ medium vessels (histology). Various distribution. Cryoglobulinemia. Deposition of IgG and/or IgM (immunoluorescence). ANCA – negative. Hypocomplementemic vasculitis. Small +_ medium vessels (histology). Various distribution. Low C3 or C4. Deposition of IgG and/or IgM (immunoluorescence). ANCA – negative. Hypersensitivity vasculitis. Small +_ medium vessels (histology). Various distribution. Deposition of IgG and/or IgM (immunoluorescence). ANCA – negative. Table 3. Pseudovasculitides Pathogenetic mechanism Nosologies Key signs Endothelial infections (endothelitis) EBV Inflammatory angiopathy +EBV in blood PCR or very high antibodies in ELISA CMV Inflammatory angiopathy +EBV in blood PCR or very high antibodies in ELISA HSV 1 and 2 Inflammatory angiopathy +HSV in blood PCR or very high antibodies in ELISA VZV Inflammatory angiopathy + VZV in blood PCR or very high antibodies in ELISA Micro- embolism Septic embolism Inflammatory angiopathy + detected source of bacterial embolia Atheroembolism (unstable atheromatous plaques of aorta or large vessels) Signs of occlusion medium +_ small vessels in a patient > 45 y.o. Onset after endovascular intervention, after anticoagulants, and rarely spontaneously. Imaging signs of aortal atherosclerosis with unstable plaques. Atheroemboli detected in histology or fundoscopy. Classical triade: livedo reticularis + renal failure + eosinophilia. Another triade: livedo reticularis + pain in lower extremities + preserved pulse. Atrial myxoma Occlusion of medium +_ small vessels. Atrial tumor detected by ultrasound. Metabolic vascular damages Diabtic angiopathy Signs of small vessel angiopathy with various distribution + microalbumin or protein in urine and/ or retinal angiopathy in a patient with high blood glucose/ Homocystenemia Occlusion of medium +_ small vessels + high blood homocystein. Calciphylaxis Occlusion of medium +_ small vessels + vascular calcification detected by histology or x-ray. Causes: hyperparathyroidism, chronic renal failure, diabetes, etc. Thrombophilias DIC syndrome (chronic) Occlusion of medium +_ small vessels + high d-dimer + manifestations of one of diseases that can cause DIC. Paraneoplastic hypercoagulation A variant of chronic DIC caused by malignancy. Intake of estogens or anabolic steroids. Occlusion of medium +_ small vessels + high d-dimer + intake of estrogens or anabolic steroids. Antiphospholipid syndrome Occlusion of medium +_ small vessels + high d-dimer + antiphospholipid antibodies Thrombotic thrombocytopenic purpura Occlusion of medium +_ small vessels with various distribution (the brain is affected more than kidneys) + thrombocytopenia + anemia with schistocytosis and reticulocytosis. Hemolytic uremic syndrome Occlusion of medium +_ small vessels with various distribution (kidneys are affected more than the brain) + thrombocytopenia + anemia with schistocytosis and reticulocytosis. Tests mandatory for diagnosis and differential diagnosis: Blood test with leukocyte count and ESR, Urine test, Blood plasma electrophoresis for protein fractions, Blood tests for ANCA, ANA, RF, d-dimer, glucose, creatinine, cryoglobulins. Additional tests in special situations: Cutaneous lesions: Biopsy, histology, immunofluorescence for immune deposits; Cutaneous lesions + ANCA-negativity: Blood complement C3 and C4; Nephritis: Renal biopsy, histology, immunofluorescence for immune deposits, Anti-GBM antibody; Age >45 y.o. + lesions of lower extremities: Imaging of aorta for unstable atheromatous plaques , fundoscopy;Chronic renal failure or signs of hyperparathyroidism or diabetes: X-ray of affected soft tissue for vascular calcification .
- 3. How to use the quick reference guide I am M.D. Mikhail Valivach, who has worked with vasculitides for more than 10 years. There are numerous vascular diseases. The problem with diagnosis is due to the fact that different vascular diseases affecting the same organ can have similar clinical manifestations. And the same vascular disease in different patients having different organ involvement can show different clinical pictures. Vascular diseases can be divided into five groups depending on their pathogenetic mechanisms: (1) vascular infections, (2) vasculitides, (3) metabolic angiopathies, (4) embolism, (5) thrombophilic disorders. Each of these groups includes large lists of different nosologies. In addition, many manifestations of vascular disorders are similar with infections and other diseases. Thus, to perform diagnosis of vascular diseases one should keep in mind numerous criteria and data. To make this task easier I have created a quick reference guide for myself. I hope that this guide will be useful to other doctors too. The guide contains several tables that help to orient quickly in clinical situation. I have done my best to make these tables as short as possible to make it possible to place them on two sides of an A4 sheet. Table 1. Manifestations of vasculitides and pseudovasculitides contains a list of symptoms of vascular disorders of different locations. This list has been taken from the Birmingham Vasculitis Activity Score (BVAS) with some modifications (seehttps://www.rarediseasesnetwork.org/vcrc/documents/BVAS%20Assessment%20Training%20Manual.pdf ). If you are not familiar with this subject you can find useful details and illustrations in my presentation “Manifestations of vasculitides and pseudovasculitides” on the address http://www.slideshare.net/MikhailValivach/manifestations-of-vasculitides-and-pseudovasculitides or find it through yahoo.com using key words Valivach Manifestations of vasculitides and pseudovasculitides. If you are going to work with vasculitides professionally, you should start from drilling these symptoms. You should recognize them automatically. Size of affected vessels is an important diagnostic criterion of vasculitides. Vessels are divided into large, medium and small. Large vessels include aorta and its first branches. These vessels have cartilage in their wall. More distal arteries have a muscular layer instead of cartilage. They are called muscular type or medium size arteries. The most distant arteries, arterioles and capillaries have no muscular layer. These are small size vessels. The first criterion of vasculitis classification is the size of affected vessels. Imaging techniques including contrast angiography, sonograpy, MRI and CT are the most reliable methods of detection of large vessel damages. Contrast angiography is the most sensitive method to reveal changes in the medium size vessels. One can see small aneurisms, dilations and narrowing of vessels. It is also possible to detect medium vessel changes with histology but one needs a deep biopsy. Small vessel affection is evidently detected only by histology. In addition to imaging techniques, there are also indirect clinical signs of damages of different size vessels. They are shown in Table 2 “Differences between small, medium, and large vessel disorders”. It is important to remember that large vessel vasculitides can also affect medium vessels. Medium size vasculitis can spread to small vessels. And small vessel vasculitis can also affect medium size vessels. To reliably keep in mind the table it is useful to apply it to clinical situations several times. Besides I can recommend to see my presentation on pseudovasculitides. It contains many illustrations. For training you can compare these illustrations with Table 2 and try to determine which size vessels are affected. Go to http://www.slideshare.net/MikhailValivach/pseudovasculitides-mikhail- valivach-2015 or find it through yahoo.com using key words Valivach Pseudovasculitides. The part “Systematization of vasculitides” gives a short information on the subject. You can see more details in my presentation “Systematization and diagnosing of vasculitides” (http://www.slideshare.net/MikhailValivach/systematization-and-diagnosis-of-vasculitides-mikhail-valivach ). You can find it through yahoo.com using key words Valivach Systematization and diagnosing of vasculitides. One should remember that in those cases of small vessel vasculitides where biopsy is available it mandatory should be made. Histology is the only evident proof of vasculitis. Histology reveals the character of inflammatory infiltrate. Immune deposits are determined by direct immunofluorescence. I would like to draw your attention that the items Primary pathogenetic mechanisms and Specific secondary immune reactions are describing diagnostic criteria only of small vessel vasculitides. Determination of these mechanisms is possible only through histology and direct immunofluorescence.
- 4. Considering skin biopsy one should remember that inflammatory reactions in vessels are transient and one reaction is followed by another. For example, neutrophilic infiltrate that is an important diagnostic criterion is changed by lymphocytes in a few days and even hours. The sign of previous neutrophilic infiltrate in the form of nuclear debris (leukocytoclasis) will stay for a short time and then disappear. Later lymphocytic infiltrate will disappear too. Only changes of vascular architecture will be left. It is critically important to determine correctly the time and location of biopsy. To do this see my “Guide on skin biopsy” http://www.slideshare.net/MikhailValivach/guide-on-skin-biopsy- mikhail-valivach . You also can find it through yahoo.com using key words valivach guide on skin biopsy. Technique of punch biopsy you can see in youtube.com “the punch biopsy dermeducation” (https://www.youtube.com/watch? v=gd7j-wYwryY ). Immune deposits can be detected by direct immunofluorescence. Immune deposits are a very short term event and their detection depends on the time of biopsy. For more details on skin biopsy I recommend you an excellent article “Cutaneous Vasculitis Update: Diagnostic Criteria, Classification, Epidemiology, Etiology, Pathogenesis, Evaluation and Prognosis by J. Andrew Carlson, Bernard T. Ng, Ko-Ron Chen. ARTICLE in AMERICAN JOURNAL OF DERMATOPATHOLOGY· JANUARY 2006”. You can download this article from the address http://www.researchgate.net/publication/7453727_Cutaneous_Vasculitis_Update_Diagnostic_Criteria_Classification_Epidemiology_Etiology_Pathogenesis_Eval uation_and_Prognosis Below “Systematization of vasculitides” you see description of vasculitides. Vasculitides are listed in the order of diagnostic priority. When you examine your patient you can find that he corresponds to criteria of two or even more vasculitides. The vasculitis that is mentioned first is the most appropriate in such cases. Detailed information on diagnosis of vasculitides is given in my presentation “Systematization and diagnosis of vasculitides” (http://www.slideshare.net/MikhailValivach/systematization-and-diagnosis-of-vasculitides-mikhail-valivach ). Or search for it through yahoo.com using key words valivach systematization and diagnosis of vasculitides. If your patient has the symptoms listed in Table 1 but does not correspond to criteria of a vasculitis, please refer to Table 3 “Pseudovasculitides”. The table gives key signs for each nosology. Lack of these signs is sufficient to reject diagnosis but their presence is not sufficient to confirm diagnosis. Detailed data on pseudovasculitides you can see in my presentation “Pseudovasculitides” (http://www.slideshare.net/MikhailValivach/pseudovasculitides-mikhail- valivach-2015 ). You can find it through yahoo.com using key words valivach pseudovasculitides. Thank you for your attention! Hope that my short reference guide will be useful for you. Mikhail Valivach, MD. Kasakhstan, Pavlodar. December 2015. Dear colleagues, with questions and suggestions you can address to Mikhail Valivach valivach@mail.ru
