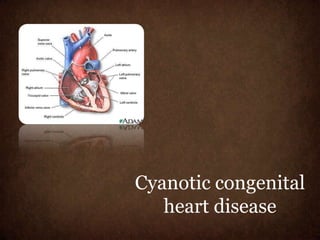
Classification of Congential Heart Diseases and cyanotic heart disease
- 2. Classification of congenital heart diseases Group I : Group II: Group III: Left to right shunts Right to lefts shunts Obstructive lesions
- 3. Left to right shunts • Atrial Septal Defect • Ventricular Septal Defect • Patent Ductus Arteriosus
- 4. Right to Left Shunts 1) Tetralogy of Fallot 2) 3) Tricuspid atresia Ebstein’s anomaly 4) Transposition of Great Vessels 5) Truncus Arteriosus 6) Total Anomalous Pulmonary Venous Return (TAPVR)
- 5. Obstructive Lesions • Aortic stenosis • Coarctation of the Aorta • Pulmonic Stenosis
- 6. Cyanotic heart disease Right to Left Shunt
- 7. Who is this guy?
- 8. ÉTIENNE-LOUIS ARTHUR FALLOT! • a French physician, 1888 Fallot accurately described in detail the four anatomical characteristics of tetralogy of Fallot.
- 9. Tetralogy OF Fallot • Most common cyanotic heart disease! 75%!
- 11. TOF 4 component! Imagine this is a HEART!
- 12. TOF 1) Vetricular Septal Defect
- 13. TOF 1) Vetricular Septal Defect 2) Pulmonic Stenosis
- 14. TOF 1) Vetricular Septal Defect 2) Pulmonic Stenosis 3) Overriding of dextroposed aorta
- 15. TOF 1) 2) 3) 4) Vetricular Septal Defect Pulmonic Stenosis Overriding of dextroposed aorta Right Ventricular hypertrophy
- 16. TOF 1) 2) 3) 4) Vetricular Septal Defect Pulmonic Stenosis Overriding of dextroposed aorta Right Ventricular hypertrophy Concentric R ventricular hypertrophy without cardiac enlargement
- 17. TOF 1) 2) 3) 4) Vetricular Septal Defect Pulmonic Stenosis Overriding of dextroposed aorta Right Ventricular hypertrophy Concentric R ventricular hypertrophy without cardiac enlargement Increase in right ventricular pressure*
- 19. RV and LV pressures becomes identical
- 20. RV and LV pressures becomes identical There is little or no L to R shunt
- 21. Hence, VSD is silent RV and LV pressures becomes identical There is little or no L to R shunt
- 22. Right ventricle into pulmonary artery across pulmonic stenosis producing ejection systolic murmur Hence, VSD is silent RV and LV pressures becomes identical There is little or no L to R shunt
- 23. Hence, the more severe the pulmonary stenosis
- 24. Hence, the more severe the pulmonary stenosis The BIGGER the Left to RIGHT shunt
- 25. Hence, the more severe the pulmonary stenosis The BIGGER the Left to RIGHT shunt Less flow into the pulmonary artery
- 26. Hence, the more severe the pulmonary stenosis The BIGGER the Left to RIGHT shunt Less flow into the pulmonary artery Shorter the ejection systolic murmur
- 27. Hence, the more severe the pulmonary stenosis The BIGGER the Left to RIGHT shunt Less flow into the pulmonary artery Shorter the ejection systolic murmur More cynosis because of less flow to the lung!
- 28. Hence, • Severity of cyanosis is directly proportional to the severity of pulmonic stenosis • Intensity of the systolic murmur is inversely related to the severity of pulmonic stenosis
- 29. Congestive failure never occur* because… Right ventricle is effectively decompressed because of the ventricular septal defect. * exception
- 30. Congestive failure never occur* because… Right ventricle is effectively decompressed 1) Anemia because of the ventricular septal defect. 2)Infective Endocarditis 3)Systemic hypertension 4)Unrelated myocarditis complicating TOF 5)Aortic or pulmonary valve regurgitation * exception
- 31. Pulmonary obstruction results in delayed P2
- 32. Pulmonary artery pressure reduce Pulmonary obstruction results in delayed P2
- 33. P2 become soft or inaudible Pulmonary artery pressure reduce Pulmonary obstruction results in delayed P2
- 34. (Second Sound) S2= A2 + P2 Since P2 is inaudible, hence S2 = A2 + P2 [S2 is single sound] P2 become soft or inaudible Aorta is displace anteriorly too, A2 become LOUD! Pulmonary artery pressure reduce Pulmonary obstruction results in delayed P2
- 35. • Ascending aorta in TOF is large, results aortic ejection click
- 36. • Diastolic interval is clear • No S3 • No S4
- 37. Concentric right ventricular hypertrophy reduce the distensibility of the right ventricle during diastole
- 38. Concentric right ventricular hypertrophy reduce the distensibility of the right ventricle during diastole “a” waves become prominent in JVP* *but not too tall
- 39. Clinical Picture • Symptomatic any time after birth • Paroxysmal attacks of dyspnea – – – – – – – – Anoxic spells Predominantly after waking up Child cry Dyspnea Blue Lose conscious Convulsion Frequency varies from once a few days to many attack everyday
- 40. “tet spell” • lethal, • unpredictable episodes • The mechanism – spasm of the infundibular septum, which acutely worsens the RV outlet obstruction.
- 41. • Dyspnea on exertion • Exercise intolerance
- 42. • Sitting posture – squatting – Compensatory mechanism – Squatting increases the peripheral vascular resistance, – which diminishes the right-to-left shunt – increases pulmonary blood flow.
- 43. • Cyanosis during feeding – Poor feeding – fussiness, tachypnea, and agitation. – Birth weight is low. – Growth is retarded. – Development and puberty may be delayed.
- 44. • Rarely, patient remain asymptomatic into adult life.
- 45. Physical examination • • • • Clubbing + Cyanosis (Variable) Squatting position Scoliosis – Common bulging left hemithorax
- 46. • Prominent “a” waves JVP • Normal heart size – Mild parasternal impulse • Systolic trill (30%)
- 47. • S1 normal • S2 single – only A2 heard – P2 soft & delayed: INAUDIBLE • Murmur – Shunt murmur (VSD) absent – Flow murmur: Ejection systolic, the smaller the flow the shorter the murmur • Ejection aortic click
- 48. • Retinal engorgement • Hemoptysis
- 49. ECG • ECG
- 50. ECG • ECG
- 52. ECG • Right axis deviation (+120° to +150°) • Right or combined ventricular hypertrophy • Right atrial hypertrophy • Partial or complete right bundle branch block (especially true of patients after surgical repair)
- 54. • Coeur en sabot (boot-shaped heart) secondary to uplifting of the cardiac apex from RVH and the absence of a normal main pulmonary artery segment
- 55. • Normal heart size due to the lack of pulmonary blood flow and congestive heart failure
- 57. • Right atrial enlargement • Right-sided aortic arch (20-25% of patients) with indentation of leftward-positioned tracheobronchial shadow
- 58. Echocardiography • Reveals a large VSD • overriding aorta • variable degrees of right ventricular outflow tract (RVOT) obstruction
- 59. Course and Complication 1) Each anoxic spell is potentially fatal 2) Polycytemia 1) Cerebrovascular thrombosis 3) Anoxic infaction of CNS 1) Neurological complication
- 60. 4) LUNG is an awesome filter. 1) Bypassing it may not be a good idea! 2) TOF, venous blood from gut, peripheral system by pass the lung and re-enter circulation 3) Hence TOF can cause: 1) Brain Abcess 2) Infective endocarditis 3) Paradoxical embolism
- 61. Management of anoxic spell 1) Knee chest position 2) Humified O2 3) Be careful not to provoke the child 1) Especially you are bad at gaining IV access 2) Ask for help from someone more experience 3) Permit the baby to remain with mother 4) Morphine 0.1 -0.2 mg/Kg Subcutaneous 5) Correct acidosis – Sodium Bicarb IV
- 62. 6) Propanolol 1) 0.1mg/kg/IV during spells 2) 0.5 to 1.0 mg/kg/ 4-6hourly orally 7) Vasopressors: Methoxamine IM or IV drip 8) Correct anemia 9) GA is the last resort
- 63. Palliative Surgery • Blalock-Taussig shunt • Pott procedure • Waterston shunt
- 64. Blalock Taussig Shunt • Subclavian artery – Pulmonary artery anastomosis
- 65. Modified Blalock Taussig Shunt • Goretex graft
- 68. • Palliative operation prolong life • Increase exercise tolerance
- 69. Definitive operation • Closing the VSD • Resecting infundibular • 90% can return almost normal life after operation • Complication: – – – – – RBBB Residual VSD Residual Pulmonary stenosis Pulmonary regurgitation (pulmonary valve excised) Risk 5%
- 70. Transposition of Great Areries (TGA) • Aorta originating from the right ventricle, and pulmonary artery originating from the left ventricle • Accounts for 5-7% of all congenital heart disease
- 71. TGA • Survival is dependent on the presence of mixing between the pulmonary and systemic circulation • Atrial septal defect is essential for survival • 50% of patients have a VSD • Usually presents in the first day of life with profound cyanosis • More common in boys
- 72. TGA • Exam : • cyanosis in an otherwise healthy looking baby • Loud S2 ( aorta is anterior ) • CXR : • Egg on side • Narrow mediastinum
- 73. TGA .. Acute Management • PGE-1 with no supplemental O2 Maintain ductus arteriosus patency, this will increase the effective pulmonary blood flow, and thence increase the left atrial pressure, therefore inhance the left to right shunt at the atrial level • Balloon atrial septostomy Life saving procedure in the presence of inadequate atrial septal defect
- 74. TGA .. Surgical Management • Arterial switch – with re-implantation of the coronary artery to the new aortic site. • Atrial switch : – the old style surgery – Redirecting the pulmonary and systemic venous return to result in a physiologically normal state – The right ventricle remains the systemic ventricle – Rarely needed
- 75. Truncus Arteriosus • The presence of a common trunk that supply the systemic, pulmonary and coronary circulation • Almost always associated with VSD • 1.2-2.5% of all congenital heart disease
- 76. Truncus Arteriosus • There are different anatomical tupes of truncus arteriosus • This is relevant for surgical repair
- 77. Truncus Arteriosus • Generally patients have increased pulmonary blood flow • Degree of cyanosis is mild and may not be evident clinically until late stage with pulmonary vascular disease • Presenting feature is congestive heart failure (tachypnia, hepatomegally)
- 78. Truncus Arteriosus • Exam is significant for – Single S2 – Ejection click of the abnormal truncal valve – Systolic murmur of truncal valve stenosis if present – Diaastolic murmur of truncal valve insufficiency – Gallop • CXR : Cardiomegally , increased pulmonary circulation
- 79. Managment • Acute management – No O2 to minimize pulmonary blood flow – Diuretics – Afterload reduction to inhance systemic blood flow •Surgical management: complete repair with VSD closure and conduit placement between the right ventricle and pulmonary arteries •Long term problems : –truncal valve dysfunction –RV conduit obstruction
- 80. Trcuspid Atresia • Complete absence of communication between the right atrium and right ventricle • About 3 % of congenital heart disease
- 81. Tricuspid Atresia • There is an obligate interatrial communication • Usually associated with VSD • The pulmonary blood flow is dependent on the size of the VSD • Pulmonary blood flow can be increased or decreased causing variable presenting symptoms • If there is no VSD ( also called Hypoplastic right ventricle) the pulmonary blood flow is dependent on the PDA
- 82. Tricuspid Atresia- presentation • The presentation will depend on the amount of pulmonary blood flow – If the PBF is decreased, the main presenting symptom is cyanosis – If the PBF is increased the presentation is that of congestive heart failure • CXR will also reflect the amount of pulmonary blood flow
- 83. Tricuspid Atresia- EKG Very characterestic : Left axis deviation
- 84. Management PBF Decreased PGE-1, and minimal supplemental O2 to maintain ductal patency Increased No O2 Afterload reduction Diuretics
- 85. Surgical Management Single ventricle paliation • First stage : to establish a reliable source of PBF – Aorta to pulmonary artery shunt ( BT shunt) – Pulmonary arterial banding in cases of increased PBF • Second stage: Glenn Anastomosis ( superior vena cava to pulmonary artery • Third stage : Fontan anastomosis ( Inferior vena cava to pulmonary artery
- 86. Total Anomalous Pulmonary Venous Return (TAPVR)
- 88. Radiography
- 91. Thank You
