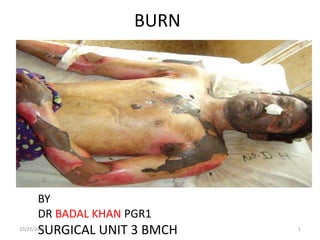
Burn classification and management
- 1. BURN BY DR BADAL KHAN PGR1 SURGICAL UNIT 3 BMCH10/22/2016 1
- 2. INTRODUCTION Majorty of burns in children are SCALDS caused by accidents with kettles,pans,hot drinks and bath water In young males burn caused by experimenting With mathes and inflamable liquides Electrical and chemical injuries occur in adults with Associated conditions such as mental disease, Epilepsy Alcohal and drug abuse 10/22/2016 2
- 3. ETIOLOGY OF BURNS DRY HEAT FLAME ELECTRICT CONTACT CHEMICAL FROSTBITE IONIZING RADIATION 10/22/2016 3
- 4. CLASSIFICATION OF BURNS 1.Depending on the percentage of burns MILD o Partial thickness burns <15% in adults and <10% In children or o Full thickness <2% o Can be treated on outpatient department 10/22/2016 4
- 5. Classification (cont……. MODERATE oSecond degree burn of 15-25% burns oThird degree burn between 2-10% burns oBurns which are not involving eyes,ears Face,hand,feet and perineum 10/22/2016 5
- 6. CLASSIFICATION (CONT……) SEVERE oSecond degree burns more then 25% in adults and More then 20% in children oAll third degree burns more then 10% oAll electrical burns and inhalation burns oBurns with fracture oBurns involving eyes,ears,feet,hands and perineum 10/22/2016 6
- 7. Classification(cont…..) 2.Depending on thickness of skin involved First degree Second degree Third degree Fourth degree Partial thickness burns I. Superficial II. deep Full thickness burns10/22/2016 7
- 8. CLASSIFICATION(CONT…..) a.First degree Epidermiss looks red and painfull No blisters formation Heals rapidly In 5-7 days by epithelialization Without scarring 10/22/2016 8
- 9. Classification(cont…..) b.2nd degree burns affected area is red,mottled,painfull Blister formation Heals in 14-21 days by epithelialization With scaring 10/22/2016 9
- 10. CLASSIFICATION(CONT……) C.3rd degree burns Affected area is painless and insensetive with Thrombosis of superficial vessels It requires grafting D.4th degree burns It involves underlying Tissues Muscles bones10/22/2016 10
- 11. Degrees of burns. Partial thickness and full thickness discuss in asessment of burn 10/22/2016 11
- 12. Pathophysiology of burn injury Most common organ affected is the skin Burn can also damage airways and lungs with life Threatening consequenses Respiratory system injuries occure if person trapped In a burning vehicle,house,car and is forced to inhale The hot and poisonous gases Hot gases burn the lining of airway above the larynx And lining start to swell later on block the airway Steam causes damage to the lower airways,respiratory Epithelium swells and detach from bronchial tree 10/22/2016 12
- 13. Pathophysiology(cont……) Metabolic poisoning Carbon monoxide is a product of incomplete combustion That is often produced by fires in a closed space is one of Many poisonous gases Co binds to hb with an affinity of 240> O2 so block Transport Of O2 Level of carboxyhaemoglobin in blood can be measure Conc >10% dangerous and need treatment with pure Oxygen for more then 24hours Hydrogen cynide causes metabolic acidosis by interefering With mitochondrial respiration10/22/2016 13
- 14. Pathophysiology(cont……) Inhalational injury caused by mainute particles within thick smoke because Of their small size and are not filtered by the upper Airwayand are carried down to lung parenchyma Stick to moist lining causes intense reaction in alveoli Causes chemical pneumonitis followed by oedema within Alveolar sac and dec gaseous exchange Bacterial pneumonia occures 10/22/2016 14
- 15. Pathophysiology(cont……) Inflamtion and circulatory changes Burn skin release of neuropeptides activation of Complement are intiated by stimulation of pain fibers and Alteration of proteins by heat Activation of hageman factor alter archidonic acid Thrombin and kallikrein pathways 10/22/2016 15
- 16. Pathophysiology(cont……) At cellular level Complement causes degranulation of mast cells Attracts neutrophils which also degranulate and releases Large amount of free radicals and proteases Mast cells also releases TNF@ which act as chemotactic Agent to inflamatory cells These inflamatory factors alter permeability of bld vessels Large protein molecules can also escape with ease Damaged collagen and extravasated proteins oncotic Pressure further increase flow of water from intravascular To extravascular space10/22/2016 16
- 17. Pathophysiology Heat causes coagulation necrosis of skin and subcutaneous tissue. ↓ Release of vasoactive peptides ↓ Altered capillary permeability ↓ Loss of fluid → Severe hypovolaemia ↓ Decreased cardiac → Decreased myocardial output function ↓ Decreased renal blood → Oliguria flow (Renal failure) ↓ Altered pulmonary resistance causing pulmonary Oedema infection Systemic Inflammatory Response Syndrome (SIRS) ↓ Multi Organ Dysfunction Syndrome (MODS). 10/22/2016 17
- 18. ASSESSMENT OF BURNS 1.ASSESSING SIZE Burn size should be assessed in a controlled environment To avoid hypothermia In smaller burns just cut a piece a clean paper the size of patient ,s whole hand (digit and palm)which present 1% TBSA And match this to the area Another accurate way of measuring the size of burns is to draw The burn on a LUND AND BROWDER CHART Age in yrs 0 1 5 10 15 adult A head 9 8 6 5 4 3 B thigh 2 3 4 4 4 4 C leg 2 2 3 3 3 310/22/2016 18
- 19. ASSESSMENT(CONT…..) RULE OF 9 (wallace,s rule of 9 Each upper limb is 9% TBSA Each lower limb is 18% TBSA Torso 18% each side Head and neck 9% Perineum 1% In children head and neck is 18% and Lower limb is 13.5% each=13.5*2=27% 10/22/2016 19
- 20. Rule of 9 10/22/2016 20
- 21. ASSESSMENT(CONT…..) 2.Assessing depth from the history Burning of human skin is temperature and time dependent It takes 6 hours for skin maintained at 44c* for irreversible changes A surface teperature of 70c* for 1 second produce epidermal destruction Example of Exposure to hot water at 65c* 45 second exposure produce full thickness burn 15 second exposure produce deep partial thickness burn 7 second exposure produce superficial partial thikness burn 10/22/2016 21
- 22. ASSESSMENT(CONT…..) a) Superficial partial thickness burns No deeper then papillary dermis Blister formation Loss of epidermis Capillary return visible When blanched Dermis is pink and moist Pin prick sensation normal Heal without scarring In 2 weeks Treatment is non surgical 10/22/2016 22
- 23. Superficial partial thickness burns After 24 hours after burn After 2 weeks 10/22/2016 23
- 24. Superficial partial thickness burn after 3 months Pigment returning 10/22/2016 24
- 25. ASSESSMENT(CONT…..) b)Deep partial thickness burn Damage to deeper parts of dermis Epidermis is usually lost Fixed capillary staining Colour does not blanch with pressure Sensation is reduced Pt is unable to distinguish sharp from blunt pressure Takes 3 or more weeks to heal without surgery Leads to hypertrophic scarring 10/22/2016 25
- 26. ASSESSMENT(CONT…..) c) Full thickness burns Whole of the dermis destroyed Hard and leathery feel No capillary return Often thrombosed vessels can be seen under The skin These are completely anesthetised No pain and no bleeding 10/22/2016 26
- 27. Causes of death in burns a. Hypovolaemia and shock b. Renal failure c. Pulmonary oedema and ARDS d. Septicaemia e. Multiorgan failure 10/22/2016 27
- 28. Full thickness burn Wraped in cling film 10/22/2016 28
- 29. Deep partial thickness burn tangential shaving to remove dead dermis Dermis remove layer by layer untill bleeding 10/22/2016 29
- 30. Hypertrophic scarring following a deep dermal burn. After 3 or more weeks 10/22/2016 30
- 31. Management of burns Management of burns is consist of prehospital care & hospital care 10/22/2016 31
- 32. Management of burns Prehospital care Stop the burning process Stop,drop and roll is a good method of extinguishing Fire Cool the burn wound This provide analgesia and slow the delayed micro- -vascular damage which occure after a burn injury Cooling should be for minimum 10 mintues and up to One hour to avoid hypothermia Give oxygen Give oxygen especialy if there is altered level concious_ -ness level10/22/2016 32
- 33. Management of burns Elevate Sitting a patient up with a burned airway may prove life Saving Elevation of burned limbs reduce swelling and discomfort Check for other injuries A standard ABC check followed by a secondary survey Patients burned in explosions may have head and spine injuries And other life threatening problems 10/22/2016 33
- 34. Management of burns Indications for admission in burns Susected airway or inhalational injury Any burn require fluide resusciation Any burn in extreme of ages All electrical and chemical burns Any burn which require surgery Burn of any significance to hands,face,feet or perineum Suspicious of non accidental injury 10/22/2016 34
- 35. Management of burns Hospital care Admit the patient Airway control Breathing and ventilation Circulation Disability Exposure with environment control Fluid resuscitation Assess the %age,degree and type of burn Keep the patient in clean environment Sedation and proper analgesia 10/22/2016 35
- 36. Management of burns A.AIRWAY CONTROL Burned airway creates problems by swelling and can completely Occlude the airway Secure airway with an endotracheal tube until swelling subsided which is Usually 48 hours Delayed diagnosis of airway burn make difficult to intubate the Patient in presence of lyrangeal oedema so cricothyroidectomy Should be done Early intubation of suspected airway burn is the treatment of Choice in such patients 10/22/2016 36
- 37. Management of burns B.BREATHING A progressive increase in respiratory rate and effort ,anxiety Rising pulse and confusion with decreasing o2 saturation These symptoms take 24 hours to 5 days to appear Treatment starts as soon as possible including Physiotherapy Nebulisers Warm humidified oxygen 10/22/2016 37
- 38. Management of burns Fluide resuscitation Iv volume must be maintained following a burn in order to provide sufficient circulation to perfuse not only the organs but also the peripheral tissues,especially damaged skin Iv resuscitation is appropriate for any child with a burn greater Then 10% and 15%for TBSA for adults If oral resuscitation is to be commenced then water is given Should not be salt free It is appropriate to give oral rehydration with a solution such as DIORALYTE* Most common fluid used is ringer lactate 10/22/2016 38
- 39. Management of burns Fluid volume is relatively constant in proportion to the area Of body burned therefore there are formulate that calculate The approximate volume of fluid needed for the pt of a given Body weight with a given %age of the body burned Formulas to calculate the fluid replacement 1.parkland regime (commonly used) 4ML/%burn/kg body weight/24 hours 4*50*60=12000ml in 24 hours Half this volume is given in the frist 8 hours Second half is given in the subsequent 16 hours Others 1. Evan,s formula 2. Muir and barclay 3. Modified brook formula10/22/2016 39
- 40. Management (cont…) Fluids used Crystalloid resuscitation Ringer lactate is the most commonly used crystalloid These are as effective as colloids for maintaining intra- -vascular volume Less expensive In children Dextrose saline given for maintanaince 100ml/kg for 24 hours for frist 10kg 50ml/kg for 24 hours for next 10kg 20ml/kg for 24 hours for each kg above 20kg body weight 10/22/2016 40
- 41. Management (cont…) hypertonic saline it produces hyperosmolarity and hypernatremia Reduces shift of intracellular water to extracellular space Advantages Include less tissue oedema and a resultant decrease in Escharotomies and intubations 10/22/2016 41
- 42. Management (cont…) Colloid resuscitation Plasma proteins are responsible for the inward oncotic Pressure that counteracts the outward capillary hydrostatic Pressure. Without proteins there will be oedema Proteins should be given after frist 12 hours of burn before This time proteins will leak out of cells Given through muir and barclay formula 0.5*%age bsa burn*weight=one portion Periods of 4/4/4, 6/6, 12 hours respectively One portion to b given in each period 10/22/2016 42
- 43. Management (cont…) Monitoring of resuscitation The key to monitoring of resuscitation is urinary output Output should be between 0.5ml and 1.0ml/kg/hour If urine output is below this infusion rate should increase By 50% If still output is inadequate then a bolus of 10ml/kg given 2ml/kg/hr urinary output signals decrease in the rate of Perfusion Haematocrit measurement is a usefull tool in confirming Suspected under or overhydration 10/22/2016 43
- 44. Management (cont…)Treating the burn wound Dressings Paraffine guaze Hydrocolloids (duoderm) Biological dressings synthetic (biobrane) natural (amniotic membrane) Full-thickness and deep dermal burns need antibacterial dressings to delay colonisation prior to surgery Open method Silver sulfadiazine application without dressings commonly Used in burns of face,head and neck. Closed method Dressing done to soothen and to protect the wound To reduce the pain As an absorbent 10/22/2016 44
- 45. Management (cont…) Treating the burn wound (cont…… Tangential excision Can be done within 48 hours with skin grafting in patients with less Then 25% burn Usually done in deep dermal burns Dead dermis is removed layer by layer Untill fresh bleeding occurs Later skin grafting done 10/22/2016 45
- 46. Treating the burn wound (cont…… Treating the burn wound (cont…… escharotomy Circumferential full-thickness burns to the limbs require emergency Surgery The tourniquet effect of this injury is easily treated by incising the whole length of full-thickness burns. This should be done in the mid-axial line, avoiding major Nerves The burn needs to be cleaned and the size and depth need to be Full thickness burns and deep partial-thickness burns that will requireoperative treatment will need to be dressed with an antibacterialdressing to delay the onset of colonisation of the wound10/22/2016 46
- 47. A full-thickness burn to the upper limb with a mid-axial escharotomy. The soot and debris have been washed off. 10/22/2016 47
- 48. Topical agent advantages problems Silver sulfadiazine 1 % -Antiseptic (G +ve and G –ve -Soothening, good penetration - Hydration and softening of eschar occurs -Neutropenia, pseudoeschar -- Causes wound maceration Sulfamylon – 5% - (Mafenide acetate) Antipseudomonal, anticlostridial - Penetrates very well in to tissues Very irritant,painful Causes acidosis Silver nitrate – 0.5% - Antiseptic Stains burn area Povidone iodine (5%) - Used on granulation tissue - after eschar separation Irritant Painfull Not used in partial burns Silver sulphadiazine and cerium nitrate - Boosts cell mediated immunity and forms sterile eschar10/22/2016 48
- 49. Additional aspects of treating burn patient Analgesia Oral form of paracetamol and nsaids in superficial burns Iv opiates for large burns Im should not be given in over 10% of TBSA as absorption is Unpredictable Short acting analgesia given before dressing Energy balance Feeding should start within 6 hrs of injury to reduce gut mucosal damag Burns patients need extra feeding A nasogastric tube should be used in all patients with burns over 15% of TBSA and 10% in case of children Burn injuries are catabolic in the acute episode. Removing the burn and achieving healing stops the catabolic drive 10/22/2016 49
- 50. Additional aspects of treating burn patient control of infection Patients with major burns are immunocompromised, pathogenic and opportunistic bacteria and fungi enter via the burn wound,cathetars and iv lines They have compromised local defences in the lungs and gut due to oedema Sterile precautions must be rigorous Swabs should be taken regularly A rise in white blood cell count, thrombocytosis and increased catabolism are warnings of infection Nursing care Physiotherapy Psychological support10/22/2016 50
- 51. SURGERY FOR THE ACUTE BURN Any deep partial-thickness and full-thickness burns except those that are less than about 4 cm2, need surgery A topical solution of 1:500 000 adrenaline also helps to reduce bleeding, deep dermal burns, the top layer of dead dermis is shaved off until punctate bleeding is observed and the dermis can be seen to be free of any small thrombosed vessels Full-thickness burns require full-thickness excision of the Skin Postoperative management of these patients obviously requires careful evaluation of fluid balance and levels of haemoglobin. 10/22/2016 51
- 52. Delayed reconstruction and scar management is common for large Full thickness burns Eyelids must be treated before exposure keratitis arises Transposition flaps and Z-plasties with or without tissue expansion are useful Full-thickness grafts and free flaps may be needed for large or difficult areas Hypertrophy is treated with pressure garments to be worn for 6-18 months Smaller areas of hypertrophy, silicone patches will speed scar maturation,as will intralesional injection of steroid. Pharmacological treatment of itch is important 10/22/2016 52
- 53. Effects of burn Shock due to hypovolaemia Renal failure(toxins from burn&myoglobin) Pulmonary oedema,resp infections,ARDS,resp failure Infection by staph aureus,pseudomonas,klebsella leads to Septicemia Fungal and viral infections of dangerous type can occure GIT: Hypovolaemia, ischaemia of mucosa, erosive gastritis—Curling’s ulcer (seen in burns > 35%). Fluid and electrolyte imbalance. immunosuppression predisposes to severe opportunistic infection. Eschar formation and its problems like defective circulation, ischaemia when it is circumferential. Electrical injuries often cause fractures, major internal organ injury, convulsions. 10/22/2016 53
- 54. Effects of burn(cont…..) Inhalation burn causes pulmonary oedema, respiratory arrest, ARDS. Chemical injury causes severe GIT disturbances like erosions, perforation, stricture oesophagus (alkali), pyloric stenosis (acid), mediastinal injury. Other problems DVT, pulmonary embolism bed-sores, severe malnutrition with catabolic status, Toxic shock syndrome: It is a life-threatening exotoxin mediated disease caused by Staphylococcusaureus. It is common in children, presents with rashes, myalgia, diarrhoea, vomiting, and multiorgan failure with high mortality . 10/22/2016 54
- 55. Effects of burn(cont…..) Development of contracture is a late problem. It leads to ectropion, microstomia, disability of different joints, defective hand functions, growth retardation causing shortening COMPLICATIONS OF BURNS CONTRACTURE Ectropion of eyelid causing keratitis and corneal ulcer. Disfigurement in face. Narrowing of mouth microstomia. Contracture in the neck causing restricted neck movements. Disability and nonfunctioning of joints due to contracture Hypertrophic scar and keloid formation. 10/22/2016 55
- 56. COMPLICATIONS OF BURNS CONTRACTURE Marjolin’s ulcer It is a very well-differentiated squamous cell carcinoma occurring in a scar ulcer due to repeated breakdown (unstable scar of long duration). • It is locally malignant. • As there are no lymphatics in the scar, so there is no spread to lymph nodes. • As there are no nerves in the scar it is painless. • It has raised and everted edge with induration. • Biopsy confirms the diagnosis. Treatment Radiotherapy is not given for Marjolin’s ulcer. Treatment is either wide excision or amputation. It is curable. Once it spreads out of the scar tissue it behaves like any other squamous cell carcinoma and so can spread to regional lymph nodes10/22/2016 56
- 57. Marjolin’s ulcer developed over burns contracture 10/22/2016 57
- 58. Contracture at different parts of body chest and neck 10/22/2016 58
- 59. Contracture at different parts of body Severe contracture at knee joint causing deformity Contracture at face 10/22/2016 59
- 60. Complication of contracture Hypertrophic scar Keloid formation 10/22/2016 60
- 61. Treatment of burn contracture • Release of contracture surgically and use of skin graft or “Z” plasty or different flaps. • Proper physiotherapy and rehabilitation is essential. • Pressure garments to prevent hypertrophic scars. • Management of itching in the scar using aloe vera, antihistamines and moisturizing creams. 10/22/2016 61
- 62. Prevention of development of contracture • Joint exercise in full range during recovery period of burns • Pressure garments for a long period • Topical silicon sheeting • Saline expanders for scars 10/22/2016 62
- 63. NON THERMAL INJURIES Electrical burns Chemical burn Cold injuries Ionising radiation 10/22/2016 63
- 64. Non thermal(cont……) Electrical burns 1000v Low tension injuries Low tension injuries do not have enough energy to cause Significant destruction Entry and exit points normally in the fingers suffers small Deep burns may damage underlying nerves and vessels Ac creates a tetany within muscles so patient unable to Release the device untill the power was turned off May interfere with normal cardiac pacing and can cause Cardiac arrest 10/22/2016 64
- 65. Electrical burns(cont…..) high tension injuries 3 sources of damage 1) The flash 2) The flame 3) The current When a high tension line is earthed it can arc over the pt And causes a flash burn Extremely rapid heating of the air causes an explosion That propel the victim backward It is always a major burn There is a wound of entry and wound of exit Major internal organ injuries occures Convulsions can develope10/22/2016 65
- 66. Electrical burns(cont…..) Management Depending on injury it is managed accordingly Patient should always be admitted and should be assessed by i. ECG ii. u/s abdomen iii. Chest x-ray iv. Ct scan head sometimes v. Cardiac enzyme analysis Acidosis is common so bicarbonate infusion needed Fractures and dislocations common so managed accordingly Release of myoglobin can cause renal tubular damage and renal Failure so manitol is used to prevent myoglobin induced renal failure (compartment syndrome) 10/22/2016 66
- 67. Wound of entry in an electric burn. Electric burn 10/22/2016 67
- 68. Electrical burns(cont…..) An exit wound of a high-tension injury, Amputation and cover with the lateral portion of the second toe. 10/22/2016 68
- 69. Chemical burns There are 70000 different chemicals in regular use within industry Occasionally these cause burns There are two aspects to a chemical injury 1. Physical destruction to the skin 2. Systemic absorption The initial management of any chemical injury is copious lavage With water but some need to be remove physically eg.phosphorus A component of millitary devices The more common injuries are caused by either 1. Alkalis 2. acids 10/22/2016 69
- 70. Chemical burns(cont…) After copious lavage, the next step in themanagement of any chemical injury is to identify the chemical and its concentration and to elucidate whether there is any underlying threat to the patient’s life if absorbed systemically Alkali burns occur in oral cavity and oesophagus which leads to multiple oesophageal strictures. Alkalis alkalis are more destructive and especially when come in contact With eyes Commonly used alkalis are sodium hydroxide,lime,bleach They cause fat sponification,fluide loss,release of alkali proteinase 10/22/2016 70
- 71. Chemical burns(cont…) Acids Acid burn occurs in skin, soft tissues and GIT. In GIT, Burns affecting the fingers and caused by dilute acid are relatively common. The initial management is with calcium gluconate gel topically severe burns or burns to large areas of the hand can be subsequently treated with Bier’s blocks containing calcium gluconate 10 per cent gel it is common in stomach either due to nitric acid or sulphuric acid which may lead to severe gastritis or pyloric stenosis. Other acids are formic acid, hydrofluoric acid. They cause metabolic acidosis, renal failure, ARDS, haemolysis. Acidaemia should be corrected by IV sodium bicarbonate. 10/22/2016 71
- 72. Cold injuries Cold injuries are principally divided into two types 1. Acute cold injuries from industries 2. Frost bite inflammatory reaction is not as marked. The tissue is more resistant to cold injury than to heat injury The assessment of depth of injury is more difficult, Frostbite injuries affect the peripheries in cold climates cold injury produces delayed microvascular damage similar to that of cardiac reperfusion injury. The initial treatment is with rapid rewarming in a bath at 42°C. The level of damage is difficult to assess surgery usually does not play a role in its management10/22/2016 72
- 73. Ionising radiation These injuries can be divided into 1. Localised 2. Whole body exposure The management of localised radiation damage is usually Conservative until the true extent of the tissue injury is apparent. If damage have caused an ulcer, then excision and coverage with vascularised tissue is required. A patient who has suffered whole-body irradiation and is suffering From acute desquamation of the skin has received a lethal dose of Radiation which can cause a particularly slow and unpleasant death Dose may be lethal and may not be lethal Giving iodine tablets, the management of these injuries is supportive 10/22/2016 73
