Os Various
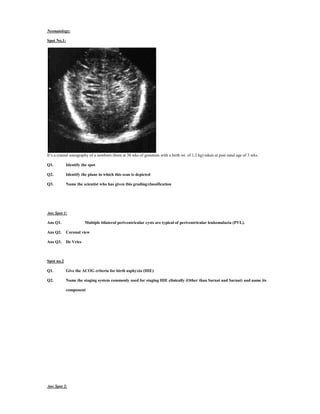
- 1. Neonatology: Spot No.1: It’s a cranial sonography of a newborn (born at 30 wks of gestation with a birth wt. of 1.2 kg) taken at post natal age of 3 wks. Q1. Identify the spot Q2. Identify the plane in which this scan is depicted Q3. Name the scientist who has given this grading/classification Ans Spot 1: Ans Q1. Multiple bilateral periventricular cysts are typical of periventricular leukomalacia (PVL). Ans Q2. Coronal view Ans Q3. De Vries Spot no.2 Q1. Give the ACOG criteria for birth asphyxia (HIE) Q2. Name the staging system commonly used for staging HIE clinically (Other than Sarnat and Sarnat) and name its component Ans Spot 2:
- 2. Ans Q1: Cord blood pH <7 with metabolic or mixed acidosis APGAR <3 at ≥ 5 minutes Seizures, Coma and hypotonia Evidence of multiorgan dysfunction Ans Q2: Levene staging (Consciousness, Seizures, Sucking or Respiration and Tone) Spot 3: Q1. Give the Brazelton stages of neonatal consciousness Q2. Name the stage in which neonatal examination should be started Ans Q1: Stage 1- Baby in deep sleep Stage 2- Baby in light sleep (REM) Stage 3- Fully awake but quite (Not moving limbs) Stage 4- Wakeful and moving limbs Stage 5- Active, alert, moving limbs and Crying (Consolabe) Ans Q2: Stage 3 Spot 4:
- 3. A Q1. Identify the stage of the ROP in given spot in ref to single long arrow (A) Q2. What is stage 0 ROP? Q3. Define rush disease Ans Q1- Satge 2 ROP- Fundus photograph showing the ridge between vascularized and avascular retina characteristic of stage 2 retinopathy of prematurity (single long arrow) Ans Q2- Stage 0 ROP- Avascular retina Ans Q3- PLUS disease that is associated with zone 1 ROP Spot 5: Q1. Give the do not resuscitate criteria as per the newer NALS guidelines Q2. Define the T piece resuscitator Q3. Give the FRC of a healthy term new born Give the compliance of a newborn Name of the scientist who has given the BPD classification Ans Q1. Ans Q2. Device which provide interrupted gas flow used to give PEEP and PIP non invasively and manually
- 4. Ans Q3. FRC- 30 ml/KG Compliance- (4-6 ml/cm H2O or 1-2 ml/kg/cm H2O) Northway’s classification Spot 6- Q1. Give the nutritional value (Calories & Protein) of following cooked items One chapatti or One Bread One Biscuit One Egg One TSF mashed potato 1 TSF cooked Dal Q2. Answer the following question Dextrose content of 1 liter Ringer lactate Na+ content of one ml of 3% NaCl Na+ content of one ml of 0.9% of NaCl Elemental Ca in 1 ml of 10% calcium Gluconate K+ content of 1 liter of Isolyte-P Ans Q1- One chapatti or One Bread- (70 calories and 2 Gms Protein) One Biscuit- (20 calories and 0.5 Gms Protein) One Egg- (80 calories and 6 Gms Protein) One TSF mashed potato- (40 calories and No Protein) 1 TSF cooked Dal- (10 calories and 0.5 gm Protein ) Ans Q2- Dextrose content of 1 liter Ringer lactate is ZERO Na+ content of one ml of 3% NaCl is 0.5 mEq Na+ content of one ml of 0.9% of NaCl is 0.15 mEq Elemental Ca in 1 ml of 10% calcium Gluconate is 9 mg K+ content of 1 liter of Isolyte-P is 20 mEq/L Spot 7:
- 5. A B Q1. Name the spot Q2. What are these chambers used for A & B (Blood cells) Q3. If doing CSF cytology for WBCs, which chambers are used for this purpose? Ans Q1- Q1. Name the spot- Neubauer Chamber Q2. What are these chambers used for A & B (Blood cells) A- WBC and B for RBC’s and platelets Q3. If doing CSF cytology for WBCs, which chambers are used for this purpose?- All 9 corners Spot 8: Q1. Identify the peripheral smear (from a febrile patient) including species with explaination Q2. Define cerebral malaria
- 6. Ans Q1- Peripheral smear showing Plasmodium Falciparum Numerous RBC infected, frequently 2 parasites (rings) per RBC Infected RBC not enlarged. Ring stage small, no large trophozoites or schizonts seen Ans Q2- Cerebral malaria is defined as Fever Glasgow coma scale <8 or coma lasting >30 minutes after a seizure Asexual parasite in blood Spot 9: Study this Arterial blood gas report of a 2 day old, 1400 gram neonate, treated with surfactant, on the ventilator for RDS. On the following settings: PIP 27cm H2O, PEEP 5cm H2O, Rate: 35/min, FiO2: 0.4, TI: 0.4 sec ABG- pH 7.57, PaCO2 22 mmHg, PaO2 156mmHg, HCO3- 11mMol/L Q1. Give the complete diagnosis Q2. Name one ventilator setting which would normalize the blood gases Q3. Name three long term complications that can occur in this neonate due to the blood gas abnormalities Ans: 1. Uncompensated respiratory alkalosis with hyperoxia 2. Reduce PIP (Peak inspiratory pressure) 3. Retinopathy of prematurity, bronchopulmonary dysplasia, periventricular leukomalacia Spot 10- Study this arterial blood gas report of a 4 year old child in the ICU with feeble peripheral pulses. pH- 7.28, PaCO2 32 mmHg, PaO2 87 mmHg, HCO3- 12 mMol/L, Base excess: -8 mMol/L Q1. Give the complete ABG diagnosis and possible cause of the abnormality Q2. Name the most appropriate corrective measure for this child Q3. Calculate the predicted carbon dioxide level for this level of bicarbonate
- 7. Ans: 1. a. Uncompensated metabolic acidosis b. Shock 2. Fluid bolus 3. 12 x 1.5 + 8 + 2 = 24-28mmHg Spot 11: Q1. A patient with UMN type lesion of the lower limbs and normal upper limbs is found to have an abscess in x-ray spine (Lateral) at first thoracic vertebrae what will be his level of lesion as per the spinal segments? Q2. Define hemiplegia, Double hemiplegia, Quadriplegia, Diplegia and Pentaplegia Ans: Q1. Third thoracic spine injury (T1-6= Add two to the vertebral lesion) Cervical- add 1, T7-9= Add 3 At T10= L1 and L2 are present T11= L3 and L4 T12= L5 and sacral segments Q2. Hemiplegia- One half of body is involved (Arms >> Legs) Double hemiplegia- All 4 limbs but difference in right and left side Quadriplegia- Paralysis of all four limbs, both arms and both legs, as from a high spinal cord accident Diplegia- Primarily affecting legs but may also involve arms Pentaplegia- Four limbs involvement with neck involvement Spot 12:
- 8. Q1. Identify the pattern of inheritance in the given Pedigree with explanation Q2. Why does this happen like this? Q3. Give 2 examples of this pattern Ans: Q1. Mitochondrial inheritance All the offsprings born to an affected female are affected Affected Males don’t pass on the disease Q2. Because sperms doesn’t contain mitochondria Q3. Leigh disease and MELAS (Mitochondrial Encephalopathy with Lactic Acidosis and Stroke like syndromes) Spot 13: This 2 yr old male child is residing in an over crowded slum and the lesions shown below are itching in nature. Lesions were also there in the groins, male genetalia and between the buttocks. Q1. Spot the diagnosis and name the etiological agent for this Q2. Treatment for this Ans: Q1. Scabies and sarcoptes scabei (Mite) Q2. 5% permethrin cream for local application x 10 hrs All family members to be treated simultaneously All linen and cloths to be boiled put out in the sun and subjected to hot iron Tt May be repeated 2 wks later (Oral ivermectin after 5 yrs of age) Spot 14: 7 yr old male child presented with sudden onset explosive watery diarrhea with abdominal distension, flatulence and epigastric cramps with out any blood or mucus in the stool. Stool examination of this child was consistent with the following
- 9. Q1. What is the diagnosis? Q2. Schedule for stool microscopic examination Q3. Source for diagnosis other than stool Q4. Drug used in treatment (At least 3) Ans: Q1. Acute symptomatic Giardiasis (Asymptomatic carriage form is the most common form) Q2. At least 3 stool specimen collected on alternate days (Detection rate up to 90%) because there is intermittent shedding of giardial cyst Q3. Duodenal aspirate or Biopsy/Fecal ELISA for antigen detection Q4. Metronidazole, Albendazole, Tinidazole, Furazolidine and Quanicrine Spot 15: 8 yr old male child presented to the emergency department with inability to get up from bed but once made to stand can stand and even walk with an ataxic gait. Q1. Spot the diagnosis; Give the criteria’s for diagnosis Q2. Diagnostic modality Q3. Treatment modalities Ans:
- 10. Q1. Juvenile Dermatomyositis Criteria- Bohan and Peter Heliotrope discoloration of upper eyelid Symmetrical proximal weakness Elevated muscle enzyme levels- AST,ALT,CK and Aldolase EMG evidence of myopathy Muscle Biopsy showing myonecrosis Q2. MRI, EMG and Muscle biopsy Q3. IV Methyl prednisolone followed by oral steroids x 2 yrs Unresponsive child may respond to Oral Methotrexate
