Trigeminal neuralgia - made easy
•Descargar como PPTX, PDF•
5 recomendaciones•5,283 vistas
Denunciar
Compartir
Denunciar
Compartir
Recomendados
Recomendados
Más contenido relacionado
La actualidad más candente
La actualidad más candente (20)
Disabilities and deformities in leprosy patients and management

Disabilities and deformities in leprosy patients and management
Cranial nerve disorders Bell’s palsy (facial paralysis) ,Trigeminal Neuralgi...

Cranial nerve disorders Bell’s palsy (facial paralysis) ,Trigeminal Neuralgi...
Similar a Trigeminal neuralgia - made easy
Facial pain is associated with significant morbidity and high levels of health care utilization, and remains a diagnostic and therapeutic challenge for both clinicians and patients; these conditions are often regarded as diagnoses of exclusion
facial-pain :Diagnosis and mangement.pdf

facial-pain :Diagnosis and mangement.pdfRomissaa ali Esmail/ faculty of dentistry/Al-Azhar university
Facial pain is associated with significant morbidity and high levels of health care utilization, and remains a diagnostic and therapeutic challenge for both clinicians and patients; these conditions are often regarded as diagnoses of exclusion
facial pain :diagnosis and treatment.pptx

facial pain :diagnosis and treatment.pptxRomissaa ali Esmail/ faculty of dentistry/Al-Azhar university
Case record...Multiple sclerosis presented clinically with bilateral trigeminal neuralgia and a high cervicomedullary active demyelinating plaqueCase record..Multiple sclerosis presented clinically with bilateral trigemina...

Case record..Multiple sclerosis presented clinically with bilateral trigemina...Professor Yasser Metwally
Similar a Trigeminal neuralgia - made easy (20)
Trigeminalneuralgiaseminar2 180526065218-converted

Trigeminalneuralgiaseminar2 180526065218-converted
Trigeminal neuralgia new classification and diagnostic grading for

Trigeminal neuralgia new classification and diagnostic grading for
Case record..Multiple sclerosis presented clinically with bilateral trigemina...

Case record..Multiple sclerosis presented clinically with bilateral trigemina...
Más de drangelosmith
Más de drangelosmith (20)
Types of personalities and traitsPersonality development

Types of personalities and traitsPersonality development
Último
PEMESANAN OBAT ASLI : +6287776558899
Cara Menggugurkan Kandungan usia 1 , 2 , bulan - obat penggugur janin - cara aborsi kandungan - obat penggugur kandungan 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 bulan - bagaimana cara menggugurkan kandungan - tips Cara aborsi kandungan - trik Cara menggugurkan janin - Cara aman bagi ibu menyusui menggugurkan kandungan - klinik apotek jual obat penggugur kandungan - jamu PENGGUGUR KANDUNGAN - WAJIB TAU CARA ABORSI JANIN - GUGURKAN KANDUNGAN AMAN TANPA KURET - CARA Menggugurkan Kandungan tanpa efek samping - rekomendasi dokter obat herbal penggugur kandungan - ABORSI JANIN - aborsi kandungan - jamu herbal Penggugur kandungan - cara Menggugurkan Kandungan yang cacat - tata cara Menggugurkan Kandungan - obat penggugur kandungan di apotik kimia Farma - obat telat datang bulan - obat penggugur kandungan tuntas - obat penggugur kandungan alami - klinik aborsi janin gugurkan kandungan - ©Cytotec ™misoprostol BPOM - OBAT PENGGUGUR KANDUNGAN ®CYTOTEC - aborsi janin dengan pil ©Cytotec - ®Cytotec misoprostol® BPOM 100% - penjual obat penggugur kandungan asli - klinik jual obat aborsi janin - obat penggugur kandungan di klinik k-24 || obat penggugur ™Cytotec di apotek umum || ®CYTOTEC ASLI || obat ©Cytotec yang asli 200mcg || obat penggugur ASLI || pil Cytotec© tablet || cara gugurin kandungan || jual ®Cytotec 200mcg || dokter gugurkan kandungan || cara menggugurkan kandungan dengan cepat selesai dalam 24 jam secara alami buah buahan || usia kandungan 1_2 3_4 5_6 7_8 bulan masih bisa di gugurkan || obat penggugur kandungan ®cytotec dan gastrul || cara gugurkan pembuahan janin secara alami dan cepat || gugurkan kandungan || gugurin janin || cara Menggugurkan janin di luar nikah || contoh aborsi janin yang benar || contoh obat penggugur kandungan asli || contoh cara Menggugurkan Kandungan yang benar || telat haid || obat telat haid || Cara Alami gugurkan kehamilan || obat telat menstruasi || cara Menggugurkan janin anak haram || cara aborsi menggugurkan janin yang tidak berkembang || gugurkan kandungan dengan obat ©Cytotec || obat penggugur kandungan ™Cytotec 100% original || HARGA obat penggugur kandungan || obat telat haid 1 bulan || obat telat menstruasi 1-2 3-4 5-6 7-8 BULAN || obat telat datang bulan || cara Menggugurkan janin 1 bulan || cara Menggugurkan Kandungan yang masih 2 bulan || cara Menggugurkan Kandungan yang masih hitungan Minggu || cara Menggugurkan Kandungan yang masih usia 3 bulan || cara Menggugurkan usia kandungan 4 bulan || cara Menggugurkan janin usia 5 bulan || cara Menggugurkan kehamilan 6 Bulan
________&&&_________&&&_____________&&&_________&&&&____________
Cara Menggugurkan Kandungan Usia Janin 1 | 7 | 8 Bulan Dengan Cepat Dalam Hitungan Jam Secara Alami, Kami Siap Meneriman Pesanan Ke Seluruh Indonesia, Melputi: Ambon, Banda Aceh, Bandung, Banjarbaru, Batam, Bau-Bau, Bengkulu, Binjai, Blitar, Bontang, Cilegon, Cirebon, Depok, Gorontalo, Jakarta, Jayapura, Kendari, Kota Mobagu, Kupang, LhokseumaweCara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...Cara Menggugurkan Kandungan 087776558899
Último (20)
7 steps How to prevent Thalassemia : Dr Sharda Jain & Vandana Gupta

7 steps How to prevent Thalassemia : Dr Sharda Jain & Vandana Gupta
Pune Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Pune No💰Adva...

Pune Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Pune No💰Adva...
Call Girl In Chandigarh 📞9809698092📞 Just📲 Call Inaaya Chandigarh Call Girls ...

Call Girl In Chandigarh 📞9809698092📞 Just📲 Call Inaaya Chandigarh Call Girls ...
Call Girls Kathua Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Kathua Just Call 8250077686 Top Class Call Girl Service Available
Cardiac Output, Venous Return, and Their Regulation

Cardiac Output, Venous Return, and Their Regulation
Low Cost Call Girls Bangalore {9179660964} ❤️VVIP NISHA Call Girls in Bangalo...

Low Cost Call Girls Bangalore {9179660964} ❤️VVIP NISHA Call Girls in Bangalo...
Call Girl In Indore 📞9235973566📞 Just📲 Call Inaaya Indore Call Girls Service ...

Call Girl In Indore 📞9235973566📞 Just📲 Call Inaaya Indore Call Girls Service ...
❤️Chandigarh Escorts Service☎️9814379184☎️ Call Girl service in Chandigarh☎️ ...

❤️Chandigarh Escorts Service☎️9814379184☎️ Call Girl service in Chandigarh☎️ ...
Circulatory Shock, types and stages, compensatory mechanisms

Circulatory Shock, types and stages, compensatory mechanisms
Premium Call Girls Dehradun {8854095900} ❤️VVIP ANJU Call Girls in Dehradun U...

Premium Call Girls Dehradun {8854095900} ❤️VVIP ANJU Call Girls in Dehradun U...
💚Reliable Call Girls Chandigarh 💯Niamh 📲🔝8868886958🔝Call Girl In Chandigarh N...

💚Reliable Call Girls Chandigarh 💯Niamh 📲🔝8868886958🔝Call Girl In Chandigarh N...
Cheap Rate Call Girls Bangalore {9179660964} ❤️VVIP BEBO Call Girls in Bangal...

Cheap Rate Call Girls Bangalore {9179660964} ❤️VVIP BEBO Call Girls in Bangal...
👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...

👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...
Chennai ❣️ Call Girl 6378878445 Call Girls in Chennai Escort service book now

Chennai ❣️ Call Girl 6378878445 Call Girls in Chennai Escort service book now
Premium Call Girls Nagpur {9xx000xx09} ❤️VVIP POOJA Call Girls in Nagpur Maha...

Premium Call Girls Nagpur {9xx000xx09} ❤️VVIP POOJA Call Girls in Nagpur Maha...
Chandigarh Call Girls Service ❤️🍑 9809698092 👄🫦Independent Escort Service Cha...

Chandigarh Call Girls Service ❤️🍑 9809698092 👄🫦Independent Escort Service Cha...
Kolkata Call Girls Shobhabazar 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Gir...

Kolkata Call Girls Shobhabazar 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Gir...
Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...
Kolkata Call Girls Service ❤️🍑 9xx000xx09 👄🫦 Independent Escort Service Kolka...

Kolkata Call Girls Service ❤️🍑 9xx000xx09 👄🫦 Independent Escort Service Kolka...
Trigeminal neuralgia - made easy
- 1. TRIGEMINAL NEURALGIA DR. ANGELO SMITH M.D WELLING HEALTHCARE PRIVATE LTD
- 4. INCIDENCE Also called tic douloureax Uncommon cranial nerve disorder More common in women @ 50-60 years of age – 3:2 ratio. Trigeminal nerve is 5th cranial nerve (CNV) And has both motor and sensory branches; mostly maxillary and mandibular branches involved.
- 6. Causal Factors Initiating pathologic events include: nerve compression by tortuous arteries of the posterior fossa blood vessels demyelinating plaques herpes virus infection infection of teeth and jaw
- 7. Pathophysiology Classical (idiopathic) form There is no known cause for the, however, studies point to an underlying vascular pathology as a cause by irritation over the trigeminal (Gasserian) ganglion. Age of onset – 52 – 58 yrs Symptomatic (secondary) form, There are known common causes affecting the CNV Compression of the trigeminal ganglion Demyelinating Disorder (axonal hyper excitability) Age of onset – 30 – 35 yrs
- 8. Compression of the Trigeminal Ganglion Vascular Tortous atherosclerotic branch of the basilar artery Basilar artery aneurysm Cerebello-Pontine Angle (CPA) Mass Meningioma Chordoma Neurinoma Metastatic (nasopharyngeal Ca)
- 9. Demyelinating Disorder #2 (axonal hyperexcitability) Multiple sclerosis (MS) – plaques at the nerve root entry After nerve injury Post-trauma Post-dental procedure Post-mandibular trauma
- 10. Demyelinating Disorder #3 (axonal hyperexcitability) Post-infectious Herpes zoster Tympanomastoiditis Dental carries (micro abscesses and pulp degeneration) Inflammatory Connective tissue disease (Sjogren’s Disease)
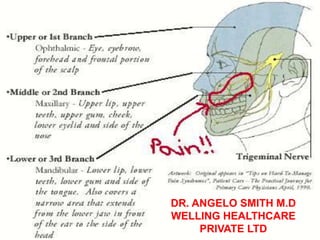
- 11. Clinical manifestations Abrupt onset with excruciating pain!! Pain described as burning, knifelike, or lighting like shock in the lips, upper or lower gums, cheek, forehead, or side of the nose. Patient may twitch, grimace, frequent blinking and tearing of eye (tic) may occur. Affects the face near the nose or mouth (trigger points)
- 13. Clinical manifestations Attacks may be brief (2 or 3 minutes) Unilateral Episodes may be initiated by triggering mechanism of light cutaneous stimulation as a specific point (trigger zone) along nerve branches. With no demonstrable sensory nor motor deficits Attacks may be restricted to 1 or 2 divisions of the trigeminal nerve Usually involves the 2nd branch (maxillary) and/or 3rd branch (mandibular) division.
- 14. Precipitating stimuli Chewing, brushing teeth, hot or cold blast of air on the face, washing the face, yawning, or talking. Patient may eat improperly, neglect hygiene practices, wear cloth over face, withdraw from interaction with others.
- 17. Differential Diagnosis: 1. Demyelinating (MS) Neurology 2. CPA tumors Neurosurgery 3. Nasopharyngeal and Para nasal pathology ENT 4. Dental Pathology Dentistry 5. Herpes zoster Neurology 6. Classical Medications Neurosurgery 7. Unstable angina Cardiology
- 18. Diagnostic studies Need to rule out other neurological causes of facial and cephalic pain. CT scan will rule out brain lesions, vascular malformations. LP and MRI will r/o MS. There is no specific diagnostic test for TN.
- 19. General Algorithm FACIAL PAIN Clinical Symptomat ic Referre d
- 20. Therapeutic Options Pharmacologic Antiepileptic drugs Anticonvulsant drugs have been used in the management of pain since the 1960s and the clinical impression is that they are useful for chronic neuropathic pain, especially when the pain is lancinating or burning. Non-antiepileptic drugs Surgical
- 21. Antiepileptic Drugs (AED) Carbamazepine Phenytoin Gabapentin Pregabalin Clonazepam Sodium Valproate/Divalproex Lamotrigine Oxcarbazepine
- 22. TN Pain Carbamazepine + Baclofen Carbamazepi ne Pregabalin Carbamazepine + Gabapentin Phenytoin Phenytoin + Baclofen Clonazepam Sodium Valproate Lamotrigine Oxcarbazepine Surgical Treatment AED +/- Painless for 6 weeks Taper dose in 4 weeks With recurrence
- 23. Non-Antiepileptic Drugs Baclofen Tocainide Pimozide Chloripramine Amitriptyline Tizanidine Proparacaine
- 24. Non-pharmacologic: Surgical Peripheral Neurectomy supraorbital, infraorbital and mental nerves Intracranial trigeminal rhizotomy portio major Glycerol gasserian gangliolysis Microvascular decompression Stereotactic radiosurgery Radiofrequency rhizotomy