portal doppler ppt .pptx
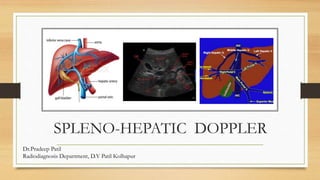
- 1. SPLENO-HEPATIC DOPPLER Dr.Pradeep Patil Radiodiagnosis Department, D.Y Patil Kolhapur
- 2. DOPPLER OF NORMAL PORTAL SYSTEM •Normal US of portal system •Principles of doppler US •Adjusting spectral doppler US •Normal portal vein •Normal hepatic veins •Normal hepatic artery
- 3. Antegrade- flow in the forward direction with respect to its expected direction in the circulatory system Retrograde - flow in the reverse direction with respect to its expected direction in the circulatory system Antegrade versus Retrograde WRT circulatory system WRT transducer
- 6. Arterial Resistance •High-resistance arteries have an RI > 0.7 low-resistance arteries have an RI of 0.55–0.7
- 8. Flow Patterns and Waveform Findings
- 9. CAUSES OF SPECTRAL BROADENING Artifical • Large sample volume • High gain Physiologic • Normal small vessel (hepatic arteries) • Normal turbulence (bifurcation) Pathologic • Compressed vessels (eg.hepatic veins in cirrhosis) • Turbulent flow (post stenotic flow)
- 10. Upstream and downstream Up-stream refers to blood that has not yet passed a reference point Downstream refers to blood that has already passed the reference point.
- 11. GOALS OF DOPPLER • Detection flow in a vessel • Detection direction of flow • Detection type of flow : -Arterial or venous -Normal or abnormal • Measurement of flow velocity
- 12. EACH EXAMINATION SHOULD BE PERFORMED WITH •Gray – scale US •Color Dopler •Power Dopler •Spectral dopler
- 13. Color box size/overlay Color box should be as small and superficial as possible
- 14. Changing color baseline to avoid aliasing
- 15. Inversion of color flow
- 16. Obtain waveform at end of normal breath – out • Take normal breath • Take normal breath out • Stop breathing • Then obtain a waveform
- 17. PORTAL VEIN The portal vein is formed by the confluence of the splenic and superior mesenteric veins. It provides approximately 70% of the incoming blood to the liver. • Normal blood flow velocity is 13-23 cm/sec with an average of 18 cm/sec. • Flow velocity is commonly somewhat phasic because rocking motion of the liver caused by motion of the heart moves the portal vein under the Doppler sample volume. • Slight phasicity may also be evident related to respiration. • Normal blood flow direction is into the liver. Any reversal of blood flow direction is abnormal and usually indicative of portal hypertension. • The portal vein is normally <13 mm in diameter. Increased diameter suggests portal hypertension.
- 20. Abnormal (pathologic) portal venous flow usually manifests in one of four ways: 1. Increased pulsatility (pulsatile waveform) 2. Slow portal venous flow 3. Hepatofugal (retrograde) flow 4. Absent (aphasic) portal venous flow
- 21. Increased pulsatility of portal vein • Portal hypertension • Tricuspid regurtation • Right heart failure • Arterio-portal vein fistula
- 22. Slow portal venous flow Normal= 16-40 cm/sec Abnormally slow flow occurs when back pressure limits forward velocity. Slow flow is diagnostic for portal hypertension (PSV <16cm/sec). Portal hypertension is caused by cirrhosis in the vast majority of cases. The most specific findings for portal hypertension are development of portosystemic shunts (eg, a recanalized umbilical vein) and slow or reversed (hepatofugal) flow. Splenomegaly and ascites are nonspecific.
- 23. Hepatofugal (retrograde) flow •Hepatofugal flow occurs when back pressure exceeds forward pressure, with flow subsequently reversing direction. •This results in a waveform that is below the baseline. • As with slow flow, this finding is diagnostic for portal hypertension from whatever cause
- 24. Absent (aphasic) portal venous flow • Absent flow in the portal vein may be due to stagnant flow (portal hypertension) or occlusive disease. • Not all cases of absent flow represent occlusive disease-like in portal HTN.
- 25. • Another feature of occlusive portal vein thrombosis (especially the non acute variety) is the development of collateral vessels in or around the occluded portal vein; this condition is referred to as cavernous transformation. • Cavernous transformation tends to be a marker for bland thrombus, since these collateral vessels usually take a long time to develop.
- 26. Congestion index of portal vein Normal value 0.07=/- 0.03 cmm.sec CI > o.o8 portal hypertension
- 27. Portal vein flow volume
- 28. Hepatic veins • The bulk of hepatic venous flow is antegrade ,although there are moments of retrograde flow Antegrade flow is away from the liver and toward the heart; thus, it will also be away from the transducer and, therefore, displayed below the baseline. • Pressure changes in the RA will be transmitted directly to the hepatic veins.
- 30. A wave It is generated by increased right atrial pressure resulting from atrial contraction. The a wave is an upward-pointing wave with a peak that corresponds to maximal retrograde hepatic venous flow. In physiologic states, the peak of the a wave is above the baseline, and the a wave is wider and taller than the v wave
- 31. S wave Its initial downward-sloping portion is generated by decreasing right atrial pressure, as a result of the “sucking” effect created by the downward motion of the atrioventricular septum. Note that the tricuspid valve remains closed. The lowest point occurs in midsystole and is the point at which negative pressure is minimally opposed and antegrade velocity is maximal.
- 32. V Wave The upward-sloping portion is generated by increasing right atrial pressure resulting from continued systemic venous return. ( valve is closed) The peak of the wave marks the opening of the tricuspid valve and the transition from systole to diastole.
- 33. D Wave Its initial downward-sloping portion is generated by decreasing right atrial pressure. The subsequent rising portion results from increasing RA pressure generated by the increasing right ventricular blood volume
- 35. Damping index of HV waveform Minimumn velocity of downward HV DI = ------------------------------------------------ Maximum velocity of downward HV
- 37. Abnormal hepatic venous flow usually manifests in one of ways : Increased pulsatility (pulsatile waveform) Decreased phasicity (decreased pulsatility) and spectral broadening. Absent (aphasic) hepatic venous flow
- 38. There are two conditions that can create a pulsatile hepatic venous waveform: Tricuspid regurgitation Right sided heart failure without TR Tricuspid regurgitation decreased S wave/ retrograde a-S-v complex tall a and v waves Pulsatile waveform Increased pulsatility (pulsatile waveform) Tricuspid regurgitation
- 39. There are two conditions that can create a pulsatile hepatic venous waveform: Tricuspid regurgitation Right sided heart failure without TR Right sided heart failure without TR: The primary abnormality is too much blood volume on the systemic venous side. Tall a and v waves. S and D waves – normal(tricuspid valve is competent) Increased pulsatility (pulsatile waveform) Right sided heart failure without TR
- 40. • During late systole, when there should normally be continued systemic venous return against a closed tricuspid valve (rising portion of the v wave), the incompetent valve allows large amounts of retrograde flow. This results in the other finding in tricuspid regurgitation, namely, an abnormally tall v wave. • Toward end diastole, when the right atrium contracts, there is a much higher blood volume (and thus, pressure) than normal, resulting in a tall a wave
- 41. Decreased phasicity (decreased pulsatility) and spectral broadening. • Pathologic causes of nonphasicity - cirrhosis, hepatic vein thrombosis (Budd-Chiari syndrome), hepatic veno-occlusive disease, and hepatic venous outflow obstruction. • As disease severity progresses and the veins become more compressed by fibrotic constriction or parenchymal edema, they lose their ability to accommodate retrograde flow. • Decreased venous compliance is seen as a waveform with a proportional loss of phasicity. • Spectral broadening is due to the narrowed caliber of compressed hepatic veins
- 42. This finding is diagnostic for venous outflow obstruction (Budd-Chiari syndrome). Absent (aphasic) hepatic venous flow
- 46. RI >0.7 ( usually non specific )
- 47. RI<0.55
- 48. TRANSJUGULAR INTRAHEPATIC PORTOSYSTEMIC SHUNTS INDICATIONS severe portal hypertension with refractory variceal bleding or ascites. Hepatorenal syndrome Hepatic hydrothorax Hepatic vein occlusion (budd-chiari syndrome) ULTRASOUND IS A TIME TESTED TOOL FOR EVALUATION OF TIPS
- 49. SIGNS OF TIPS MALFUNCTION Direct evidence • Shunt velocity <90cm/sec or >190cm/sec. • Temporal increase or decrease in shunt velocity >50cm/sec. Indirect evidence Main portal venous velocity <30cm/sec. Collateral vessels (recurrent , new or increased ) Ascites (recurrent ,new or increased ) Right – left portal venous flow reversal (ie , hepatofugal to hepatopetal)
- 51. EVALUATION OF HEPATIC VEIN IN LIVER TRANSPLANT • Standard modality for evaluating the liver after transplantation to quickly and cost – effectively diagnose complications and prevent graft loss. • The presence of a triphasic waveform had a 98% negative predictive value for hepatic vein stenosis. • A persistent triphasic hepatic vein waveform virtually excludes hepatic vein stenosis.
- 52. EVALUATION OF HEPATIC VEIN IN LIVER TRANSPLANT Loss of a triphasic waveform was found to be nonspecific for rejection . • Cholangitis • Hepatitis • Fibrosis • Lymphoproliferative disorder • Juxta hepatic fluid collections Transient spectral blunting may be seen in immediate post op period because of edema .
- 54. MAIN INDICATIONS OF SPLENIC DOPPLER Differential diagnosis of splenomegaly (acute and chronic infections, haematological and immunological diseases, portal hypertension, storage diseases) Differential diagnosis of reduced splenic size (hyposplenia/asplenia) Diffuse alterations of the spleen (diffuse benign or malign infiltration, systemic inflammatory or infectious diseases) Vascular alterations (thrombosis, infarction, aneurysm) Trauma Focal lesions of the spleen
- 55. SPLENIC VEIN • The splenic vein drains the spleen and receives inflow from the inferior mesenteric vein. The splenic vein joins the superior mesenteric vein posterior to the neck of the pancreas to form the portal vein. • The splenic vein shows low velocity forward flow toward the liver. Reversal of blood flow direction is seen with advanced portal hypertension. • Slight respiratory variation is common. • Normal diameter of the splenic vein is <10 mm. Increase in diameter is a sign of portal hypertension.
- 58. TAKE HOME MESSAGE • An understanding of the basic principles of vascular doppler US is required to suuessfully perform liver doppler US • Pathologic conditions such portal hypertension , right sided heart failure , and tricuspid regurgitation have characteristic effects on doppler waveforms. • Doppler US remains the “ WORKHORSE” modality for the evaluation of TIPS patency. • Standard modality for evaluating the liver after transplantation to quickly and cost – effectively diagnose complications and prevent graft loss.
Notas del editor
- For example, antegrade flow moves away from the heart in the systemic arteries and toward the heart in the systemic veins. antegrade flow may be either toward or away from the transducer, depending on the spatial relationship of the transducer to the vessel; therefore, antegrade flow may be displayed above or below the baseline, depending on the vessel being interrogated.
- Phasic is another word for cyclic; its absence or presence (and degree) may be qualified…..NOT QUANTIFIED Phase is a stage, or portion, of a phasic process; the number of phases may be quantified As long as there is flow, there is some form of phasicity. If there is mild undulation (shallow slopes and a small vertical range between inflections), as in normal veins, the waveform is described as phasic. If there is marked undulation (steep slopes and a wide vertical range between inflections), as in normal arteries, the waveform is described as pulsatile
- the flow pattern is described as “biphasic” if two sounds are heard during each cycle and as “triphasic” if three sounds are heard. More recently, sonologists have held that phase is defined in terms of discrete flow components in either direction
- Spectral broadening is seen when the waveform is no longer traceable with a marker or pencil In other words the spectral window starts to fill in. 1)Artificially 2)physiologically(in small vessel) 3)pathologically
- From the perspective of the stenosis, transducer A is located upstream. At the position of transducer A, a downstream stenosis is detected. From the perspective of the stenosis, transducer B is located downstream. At the position of transducer B, an upstream stenosis is perceived
- Sos – sinosidual obstruction syndrome Tips – trans juglular intrahepatic porto-systemic shunt
- In severe portal hypertension, there is a period of time during the disease course when flow is neither hepatopetal nor hepatofugal, but stagnant. This results in absent portal venous flow and puts the patient at increased risk for portal vein thrombosis. The most reliable distinguishing gray-scale US feature of malignant thrombus is the combination of an echogenic filling defect with an adjacent liver mass Arterialization (of the portal venous waveform)
- Even in pathologic states, the a wave remains wider than the v wave,bwhich represents the best way to initially orient oneself on the waveform. The only time this rule breaks down is in cases of severe tricuspid regurgitation.
- The position of the peak of the v wave varies from above to below the baseline in normal states
- Normal value : <0.6 Severe portal hypertension : >0.6
- In early systole, when the atrioventricular septum is descending and would normally create a large burst of negative right atrial pressure, creating the deepest antegrade wave (S wave), the incompetent valve instead relieves all or part of the vacuum effect. The result is an S wave that is no longer as deep as the D wave. When severe TR, flow can switch to retrograde, resulting in an S wave that is above the baseline, merging with the a and v waves
- The tall a wave is due to increased right atrial pressure toward end diastole, generated by the larger-than-normal volume contained by the RA as it contracts. The tall v wave is due to increased right atrial pressure toward end systole, due to the larger-than-normal volume the right atrium contains while still trying to accommodate continued systemic venous return
- Types OTBO obstruction: ( Obstruction d/t thrombus – hypercoagulable state) type (I) with obstruction of the IVC (±HV), radicular type (II) with obstruction of HV, venoocclusive type (III) with obstruction of small centrilobular veins. large intrahepatic collateral vein bypassing the occluded hepatic veins.
- End stage liver disease
- hepatic arterial RI is not useful for diagnosing cirrhosis or predicting its severity inflammatory edema, arterial compression by regenerative nodules, and arterial compression by stiff noncompliant (fibrotic) parenchyma, have been thought to increase resistance hepatic arterial buffer response” (compensatory small artery proliferation and increased numbers of arteriolar beds) and arteriovenous shunting, are thought to decrease resistance
- Normal functioning TIPS . On a spectral doppler US image , the colour doppler image shows the cephalic end of a TIPS in blue The waveform is below the baseline , a finding that corresponds to antegrade flow. Normally functioning TIPS spectral doppler image shows the caudal end of the TIPS in red . The waveform is above the baseline (antegrade flow)
- Transient dampening of the hepatic vein waveform in 51 yr old man after orthotopic liver transplantation . Duplex doppler image obtained 1 day after surgery shows the waveform of the middle hepatic vein . The spectrum is in the correct direction , posteriorly toward the IVC : however , the waveform is blunted the pt continued to do well clinically Duplex doppler image obtained 1 day later shows a normal waveform of the middle hepatic vein.
- (a) The splenic vein can be imaged behind the body and tail of the pancreas in B-mode. Transverse section through the upper abdomen. (b) Colour Doppler of the flow in the splenic vein in a transverse section through the upper abdomen. The flow in the splenic vein (SV) along the pancreatic tail is directed towards the transducer and therefore displayed red. Close to the pancreatic head, the flow in the splenoportal confluence (SPC) is directed away from the transducer and therefore displayed blue. The aorta (DAO), the inferior vena cava (IVC), right renal artery (RA) and the superior mesenteric artery (SMA) are shown.
- (c) Spectral Doppler of the flow in the splenic vein shows an antegrade flow with a time average maximal velocity (TAMAX) of 30.7 cm/s and a mean time average velocity (TAMEAN) of 16.6 cm/s. Transverse section through the upper abdomen. (d) Longitudinal section through the middle upper abdomen shows the pancreatic body (P) and the splenic vein (SV). The stomach is marked with “S”