Presentation on nephrotic syndrome
•Descargar como PPTX, PDF•
22 recomendaciones•12,854 vistas
nephrotic syndrome
Denunciar
Compartir
Denunciar
Compartir
Recomendados
Recomendados
Chronic glomerulonephritis is a kidney disorder caused by slow, cumulative damage and scarring of the tiny blood filters in the kidneys. These filters, known as glomeruli, remove waste products from the blood.
Chronic Glomerulonephritis - Symptoms, Diagnosis, Treatment of Chronic Glomer...

Chronic Glomerulonephritis - Symptoms, Diagnosis, Treatment of Chronic Glomer...Lazoi Lifecare Private Limited
Más contenido relacionado
La actualidad más candente
Chronic glomerulonephritis is a kidney disorder caused by slow, cumulative damage and scarring of the tiny blood filters in the kidneys. These filters, known as glomeruli, remove waste products from the blood.
Chronic Glomerulonephritis - Symptoms, Diagnosis, Treatment of Chronic Glomer...

Chronic Glomerulonephritis - Symptoms, Diagnosis, Treatment of Chronic Glomer...Lazoi Lifecare Private Limited
La actualidad más candente (20)
Chronic Glomerulonephritis - Symptoms, Diagnosis, Treatment of Chronic Glomer...

Chronic Glomerulonephritis - Symptoms, Diagnosis, Treatment of Chronic Glomer...
Destacado
Destacado (11)
Similar a Presentation on nephrotic syndrome
Similar a Presentation on nephrotic syndrome (20)
Approach To The Management Of Hyperbilirubinemia In Term

Approach To The Management Of Hyperbilirubinemia In Term
Approach To The Management Of Hyperbilirubinemia In Term

Approach To The Management Of Hyperbilirubinemia In Term
Approach To The Management Of Hyperbilirubinemia In Term

Approach To The Management Of Hyperbilirubinemia In Term
Approach To The Management Of Hyperbilirubinemia In Term

Approach To The Management Of Hyperbilirubinemia In Term
Approach To The Management Of Hyperbilirubinemia In Term

Approach To The Management Of Hyperbilirubinemia In Term
Nephrotic syndrome in children. for under graduates

Nephrotic syndrome in children. for under graduates
Último
❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Chandigarh Call Girls Service ☎️ Call Girls In Chandigarh BEST CALL GIRL ESCORTS SERVICE IN CHANDIGARH CALL WATTSAPP 98151-579OO THE MOST BEAUTIFUL INDEPENDENT ESCORT CALL GIRL SERVICE In Chandigarh WE ARE PROVIDING GENUINE CALL GIRL SERVICE
I AM A a NATURAL BRUNETTES, SLIM BODY, NATURAL LONG HAIR AND ALL TYPE OF HAIR IS A NATURAL BRUNETTE IN THE MOST BEAUTIFUL MODELS INDEPENDENT ESCORT GIRL I AM A NATURAL BRUNETTE WITH ROOM AND HOTEL AND A NATURAL BRUNETTE WITH A BODY MADE FOR SIN AND ALL TYPE OF ME ALL THE TIME
I SEND YOU A HAIR, VERY SOCIABLE AND FUNNY, READY TO ENTERTAIN TO ENTERTAIN U AND MAKE FORGET ABOUT TO AGET ENTERTAINMENT YOU AND MAKE FORGET ABOUT ALL THE PROBLEMS. LET'S HAVE A WONDERFUL TIME TOGETHER AND FORGET ABOUT EVERYTHING ALL TYPE SERVICE ENJOYMENT SAFE AND SECURE IN CALL OUT CALL HOME AND HOTEL ANYTIME AVAILABLE
AND ALL TYPE SERVICE ENJOYMENTPANCHKULA INDEPENDENT BEST CALL GIRL ESCORTS SERVICE IN PANCHKULA INDEPENDENT CALL GIRL Chandigarh Call Girls In Chandigarh BEST Call Girls in CHANDIGARH Escort Service provide Cute Nice sweet and Sexy Models in beautiful CHANDIGARH city cash in hand to hand call girl in CHANDIGARH and CHANDIGARH escorts. HOT & SEXY MODELS // COLLEGE GIRLS IN CHANDIGARH AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME ★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE ★ 100% SATISFACTION,UNLIMITED ENJOYMENT. ★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE Profiles Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call
Services :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without a Condom)-❤️ Chandigarh Call Girls Service☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Chandigarh Call Girls Service ☎️ Call Girls In Chandigarh❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...

❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...Rashmi Entertainment
PEMESANAN OBAT ASLI : +6287776558899
Cara Menggugurkan Kandungan usia 1 , 2 , bulan - obat penggugur janin - cara aborsi kandungan - obat penggugur kandungan 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 bulan - bagaimana cara menggugurkan kandungan - tips Cara aborsi kandungan - trik Cara menggugurkan janin - Cara aman bagi ibu menyusui menggugurkan kandungan - klinik apotek jual obat penggugur kandungan - jamu PENGGUGUR KANDUNGAN - WAJIB TAU CARA ABORSI JANIN - GUGURKAN KANDUNGAN AMAN TANPA KURET - CARA Menggugurkan Kandungan tanpa efek samping - rekomendasi dokter obat herbal penggugur kandungan - ABORSI JANIN - aborsi kandungan - jamu herbal Penggugur kandungan - cara Menggugurkan Kandungan yang cacat - tata cara Menggugurkan Kandungan - obat penggugur kandungan di apotik kimia Farma - obat telat datang bulan - obat penggugur kandungan tuntas - obat penggugur kandungan alami - klinik aborsi janin gugurkan kandungan - ©Cytotec ™misoprostol BPOM - OBAT PENGGUGUR KANDUNGAN ®CYTOTEC - aborsi janin dengan pil ©Cytotec - ®Cytotec misoprostol® BPOM 100% - penjual obat penggugur kandungan asli - klinik jual obat aborsi janin - obat penggugur kandungan di klinik k-24 || obat penggugur ™Cytotec di apotek umum || ®CYTOTEC ASLI || obat ©Cytotec yang asli 200mcg || obat penggugur ASLI || pil Cytotec© tablet || cara gugurin kandungan || jual ®Cytotec 200mcg || dokter gugurkan kandungan || cara menggugurkan kandungan dengan cepat selesai dalam 24 jam secara alami buah buahan || usia kandungan 1_2 3_4 5_6 7_8 bulan masih bisa di gugurkan || obat penggugur kandungan ®cytotec dan gastrul || cara gugurkan pembuahan janin secara alami dan cepat || gugurkan kandungan || gugurin janin || cara Menggugurkan janin di luar nikah || contoh aborsi janin yang benar || contoh obat penggugur kandungan asli || contoh cara Menggugurkan Kandungan yang benar || telat haid || obat telat haid || Cara Alami gugurkan kehamilan || obat telat menstruasi || cara Menggugurkan janin anak haram || cara aborsi menggugurkan janin yang tidak berkembang || gugurkan kandungan dengan obat ©Cytotec || obat penggugur kandungan ™Cytotec 100% original || HARGA obat penggugur kandungan || obat telat haid 1 bulan || obat telat menstruasi 1-2 3-4 5-6 7-8 BULAN || obat telat datang bulan || cara Menggugurkan janin 1 bulan || cara Menggugurkan Kandungan yang masih 2 bulan || cara Menggugurkan Kandungan yang masih hitungan Minggu || cara Menggugurkan Kandungan yang masih usia 3 bulan || cara Menggugurkan usia kandungan 4 bulan || cara Menggugurkan janin usia 5 bulan || cara Menggugurkan kehamilan 6 Bulan
________&&&_________&&&_____________&&&_________&&&&____________
Cara Menggugurkan Kandungan Usia Janin 1 | 7 | 8 Bulan Dengan Cepat Dalam Hitungan Jam Secara Alami, Kami Siap Meneriman Pesanan Ke Seluruh Indonesia, Melputi: Ambon, Banda Aceh, Bandung, Banjarbaru, Batam, Bau-Bau, Bengkulu, Binjai, Blitar, Bontang, Cilegon, Cirebon, Depok, Gorontalo, Jakarta, Jayapura, Kendari, Kota Mobagu, Kupang, LhokseumaweCara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...Cara Menggugurkan Kandungan 087776558899
Último (20)
Call 8250092165 Patna Call Girls ₹4.5k Cash Payment With Room Delivery

Call 8250092165 Patna Call Girls ₹4.5k Cash Payment With Room Delivery
Difference Between Skeletal Smooth and Cardiac Muscles

Difference Between Skeletal Smooth and Cardiac Muscles
💰Call Girl In Bangalore☎️63788-78445💰 Call Girl service in Bangalore☎️Bangalo...

💰Call Girl In Bangalore☎️63788-78445💰 Call Girl service in Bangalore☎️Bangalo...
Race Course Road } Book Call Girls in Bangalore | Whatsapp No 6378878445 VIP ...

Race Course Road } Book Call Girls in Bangalore | Whatsapp No 6378878445 VIP ...
Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available
💞 Safe And Secure Call Girls Coimbatore🧿 6378878445 🧿 High Class Coimbatore C...

💞 Safe And Secure Call Girls Coimbatore🧿 6378878445 🧿 High Class Coimbatore C...
❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...

❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...
Chennai ❣️ Call Girl 6378878445 Call Girls in Chennai Escort service book now

Chennai ❣️ Call Girl 6378878445 Call Girls in Chennai Escort service book now
Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available

Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available
Russian Call Girls In Pune 👉 Just CALL ME: 9352988975 ✅❤️💯low cost unlimited ...

Russian Call Girls In Pune 👉 Just CALL ME: 9352988975 ✅❤️💯low cost unlimited ...
Lucknow Call Girls Just Call 👉👉8630512678 Top Class Call Girl Service Available

Lucknow Call Girls Just Call 👉👉8630512678 Top Class Call Girl Service Available
👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...

👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...
Call Girls Kathua Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Kathua Just Call 8250077686 Top Class Call Girl Service Available
Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...
Circulatory Shock, types and stages, compensatory mechanisms

Circulatory Shock, types and stages, compensatory mechanisms
(RIYA)🎄Airhostess Call Girl Jaipur Call Now 8445551418 Premium Collection Of ...

(RIYA)🎄Airhostess Call Girl Jaipur Call Now 8445551418 Premium Collection Of ...
Call Girls Service Jaipur {9521753030 } ❤️VVIP BHAWNA Call Girl in Jaipur Raj...

Call Girls Service Jaipur {9521753030 } ❤️VVIP BHAWNA Call Girl in Jaipur Raj...
Bhawanipatna Call Girls 📞9332606886 Call Girls in Bhawanipatna Escorts servic...

Bhawanipatna Call Girls 📞9332606886 Call Girls in Bhawanipatna Escorts servic...
Lucknow Call Girls Service { 9984666624 } ❤️VVIP ROCKY Call Girl in Lucknow U...

Lucknow Call Girls Service { 9984666624 } ❤️VVIP ROCKY Call Girl in Lucknow U...
Presentation on nephrotic syndrome
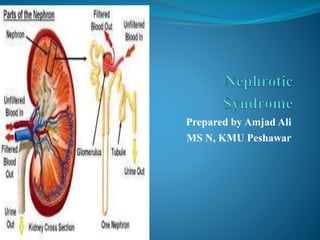
- 1. Prepared by Amjad Ali MS N, KMU Peshawar
- 2. CASE SCENARIO A male child patient aged 6 yrs was admitted in pediatric ward with: Present complains: Hematuria burning maturation History of present illness: Subject developed dyspnea 2 days back and on the present day morning blood in urine was found. Past family history: Not significant (NO ONE HAD HEMATURIA)
- 3. Investigations 1. CUE (COMPLETE URINE EXAMINATION): urine proteins: 420 (0-8 mg/dl) creatinine: 39 (30-40 mg/dl) P/C ratio : 10.70 (<0.2) pus cells : 10-15 RBC’s: LOADED 2. Abdomen USG: urinary bladder: walls are irregular and thickened IMPRESSION: cystitis (chronic) 3. Culture Test: NEGATIVE
- 4. DEFINITION Manifestation of glomerular disease, characterized by nephrotic range proteinuria and a triad of clinical findings associated with large urinary losses of protein : hypoalbuminaemia , edema and hyperlipidemia. Defined as protein excretion of > 40 mg/m2/hr First morning protein : creatinine ratio of > 2-3 : 1
- 8. Incidence ( pediatric ) 2 – 7 cases per 100,000 children per year Higher in underdeveloped countries ( South east Asia ) Occurs at all ages but is most prevalent in children between the ages 1.5-6 years. It affects more boys than girls, 2:1 ratio http://www.kidney.org/site/107/pdf/NephroticSyndro me.pdf
- 9. Etiology Genetic Secondary Idiopathic or Primary
- 10. Genetic causes Finnish type Congenital Nephrotic Syndrome Focal Segmental Glomerulosclerosis Diffuse Mesangial Sclerosis Denys-Drash Syndrome Nail – Patella Syndrome Alport Syndrome Charcot-Marie-tooth disease Cockayne syndrome Laurence-Moon-Beidl-Bardet Syndrome Galloway-Mowat Syndrome
- 11. Secondary causes Congenital Oligomeganephronia Infectious Hepatitis (B,C) , HIV-1, Malaria, Syphilis, Toxoplasmosis Inflammatory Glomerulonephritis Immunological Castleman Disease, Kimura Disease, Bee sting, Food allergens Neoplastic Lymphoma, Leukemia Traumatic ( Drug induced ) Penicillamine, Gold, NSAIDS, Pamidronate, Mercury, Lithium.
- 12. Idiopathic Minimal Change disease ( >80 % ) Mesangial proliferation Focal segmental Glomerulosclerosis Membranous Nephropathy Membranoproliferative glomerulonephritis
- 13. Clinical Features Edema Mild to start with – peri orbital puffiness, lower extremities Progression to generalized edema, ascites, pleural effusion, genital edema Decreased urine output Anorexia, Irritability, Abdominal pain and diarrhea Absence of Hypertension Gross hematuria
- 14. NO PEDAL EDEMA BUT FACIAL PUFFYNESS PRESENT
- 15. DIFFERENTIALS Protein losing enteropathy Hepatic failure Heart failure Acute/Chronic Glomerulonephritis Protein Malnutrition
- 16. Lab Investigations Urine Examination Complete Blood Count & Blood picture Renal parameters : Spot Urine Protein : Creatinine ratio Urinary protein excretion protein selectivity ratio Liver Function Test Renal Biopsy ???
- 17. Continue……… • Urinalysis - 3+ to 4+ proteinuria • Renal Function Spot UPC ratio > 2.0 UPE > 40 mg/m2/hr Serum Creatinine – normal or elevated Serum albumin - < 2.5 gm/dl Serum Cholesterol/ TGA levels – elevated Serum Complement levels – Normal or low - Nelson Textbook of Pediatrics, Vol 2, 19th Edition, page 1804
- 18. Additional Tests C3 and antistreptolysin Chest X ray and tuberculin test Hepatitis B surface antigen Indications for Biopsy Age below 12 months Gross or persistent microscopic hematuria Low blood C3 Hypertension Impaired renal Function Failure of steroid therapy
- 19. Management (Initial Episode) High protein diet Salt moderation Treatment of infections If significant edema – diuretics Aldosterone antagonist ( Fursemide, spironolactone ) Corticosteroid therapy with Prednisolone or prednisone ( 2mg/kg per day for 6 weeks followed by 1.5 mg/kg single morning dose on alternate days for 6 weeks )
- 20. Subsequent course Relapse Infrequent Relapsers : 3 or less relapses per year Frequent Relapsers : 4 or more relapses per year Steroid therapy Steroid dependant : relapse following dose reduction or discontinuation Steroid resistant : Partial or no response to initial treatment
- 21. Management of Relapse Parent Education Symptomatic therapy for infections in case of low grade proteinuria Persistent proteinuria ( 3 - 4+ ) – Prednisolone ( 2mg/kg/day until protein is negative for 3 days ) 1.5 mg/kg on alternate days for 4 weeks ) Ghai Essential Pediatrics,8th edition, page 479.
- 22. Complications Edema Infections Thrombotic complications Hypovolaemia and Acute renal Failure Steroid Toxicity
- 23. Nursing management Goals of nursing management Reducing edema Nutrition Administering medications Skin care Infection prevention Promoting psychosocial growth Parental teaching
- 24. Nursing management Assessment Age, height and weight Vital signs Past hospital admissions Immunization status Edema Urinary output Presence of infections Dietary pattern Malnourishment
- 25. Nursing management Monitoring of Vital signs Intake output Urinary protein Diet Weight Abdominal girth
- 26. Nursing management Diet High protein diet 2-3 gm/kg/day Calories- 50- 70 kcal/kg/day No Added salt Protein rich food items Egg Milk Fish Chicken Paneer Spourts Pulses & legumes
- 27. FLUID MANAGEMENT Strict intake output monitoring Hypovolemic symptoms persistent tachycardia Hypotension abdominal pain Capillary refill >2sec urine Na <10mmol/l being indicative of severe hypovolaemia Previous day output + insensible water loss Urine output monitoring
- 28. Nursing management Immunization. Live vaccines should not be given to immunosuppressed children. killed vaccines are safe to administer However live vaccine can be considered if the child is not on steroids for minimum of 03 months. Recommended -varicella, pneumococcal vaccines during remission.
- 29. References Lau, Keith, et al. "Steroid Responsive Nephrotic Syndrome in IgA Nephropathy with FSGS." The Internet Journal of Nephrology 4 (2008): n. pag. Print. "Pediatric Nephrotic Syndrome." Pediatric Nephrotic Syndrome. N.p., n.d. Web. <http://emedicine.medscape.com>. USA. NIH. NIDDK. Childhood Nephrotic Syndrome. N.p.: n.p., 2008. Print. Trachtman, Howard. “Common Diseases: Minimal Change Nephrotic Syndrome.” Nephrology Self Assessment Program 11 (2012) 19-20. Print. Trachtman, Howard. “Common Diseases: Focal Segmental Glomerulosclerosis.” Nephrology