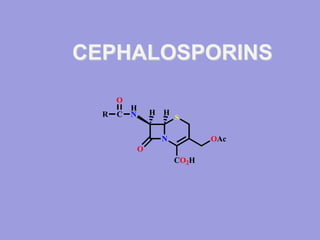
4. cephalosporins
- 2. INTRODUCTION • Antibacterial agents which inhibit bacterial cell wall synthesis • Discovered from a fungal colony Cephalosporium acremonium in Sardinian sewer water (1948) • Cephalosporin C identified in 1961 • These are β-lactam antibiotics that are closely related both structurally and functionally to the pencillins • Most cephalosporins are produced semisynthetically by the chemical attachment of side chains to 7-aminocephalosporanic acid
- 3. Why Cephalosporins? • Broad spectrum of activity • Stability to -lactamase • Oral and parenteral preparations • Widely accepted • Treats ‘day to day’ as well as ‘serious infections’ • High safety profile
- 4. Cephalosporins -Limitations • Emerging resistance patterns • Some III & IV generation cephalosporins were available only as parenteral formulations • Pharmacoeconomics
- 6. Mechanism of action • Identical to pencillins, i.e., – Binding to cephalosporin binding proteins (PBP) – Inhibition of transpeptidation process – Activation of autolysin enzyme
- 8. Resistance 1. Bacteria produce -lactamase: -lactamases are either constitutive, or more commonly, are acquired by the transfer of plasmids. 2. Altered PBPs: Modified PBPs have a low affinity for lactam antibiotics. 3. Decreased concentration of antibiotics in target site: altered porin (either in the number or function); increased active efflux system.
- 9. Classification • Have been classified as first, second, third and fourth generation, based on their bacterial spectrum and resistance to β-lactamases Note: Cephalosporins are ineffective against MRSA, L. monocytogenes, Clostredium dificile and the enterococci
- 10. Classification Generation Parenteral Agents First-generation(1960s) Cefazolin, Cephalothin Oral Agents Cefadroxil, cephalexin,cephradine Second-generation (1970s) Cefotetan, cefoxitin, cefuroxime Cefaclor, cefprozil, cefuroxime axetil Third-generation (1980s) Cefotaxime, ceftazidime, ceftizoxime, ceftriaxone Cefdinir, cefditoren, cefpodoxime proxetil, ceftibuten, cefixime Fourth-generation (1997-98) Cefepime, cefpirome
- 11. First Generation Cephalosporins Pharmacokinetics: • Oral cephalosporins are generally well absorbed • IM injection of cephalothin is very painful and hence given by IV route • Except for cefazolin, which is 80-90% protein bound, others exhibit a poor protein binding • Good distribution to most tissues except in CSF • Metabolism is not a major elimination path • Primarily excreted through kidney • Probenecid increases plasma half life • All are sensitive to β-lactamase enzyme degradation
- 13. Antimicrobial spectrum Gram-positive bacteria Gram-negative bacteria + Streptococcus pyogenes, Some viridans streptococci, Some Staphylococcus aureus, Some Streptococcus pneumoniae Some Escherichia coli, Some Klebsiella pneumonia, Some Proteus mirabilis Cocci > - Bacilli > + Bacilli > - Cocci
- 14. Uses • UTI’s • Minor staphylococcal infections • Cellulitis or soft tissue abscess • Ineffective in meningitis (do not cross BBB) • Cefazolin is drug of choice for surgical prophylaxis before cardiac surgery and before orthopedic prosthesis procedures (has better penetration to tissues)
- 15. Second Generation Cephalosporins Pharmacokinetics: • Cefaclor and cefuroxime can be given orally and have good bioavailability • Cefuroxime axetil is an ester prodrug formulation in which the ester is hydrolyzed during drug passage through the intestinal mucosa • The free cefuroxime then enters the systemic circulation • Only cefuroxime crosses BBB among 2nd gen • Only cefoxitin is 80-90% protein bound; others have poor protein binding
- 16. Second Generation Cephalosporins • More stable to β-lactamase degradation than 1st gen • Their IM injections are painful and hence preferably given administered by IV route • These are excreted unchanged through kidney • Probenecid increases plasma half life
- 17. Antimicrobial spectrum • The second-generation cephalosporins have a greater Gram-negative spectrum while retaining some activity against Gram-positive cocci.
- 18. Antimicrobial spectrum Gram-positive bacteria Gram-negative bacteria Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Haemophilus influenzae, Neisseria spp. Anaerobic bacteria - True cephalosporins have activity equivalent to first-generation agents. Cefoxitin and cefotetan have little activity Cefoxitin and cefotetan have moderate anaerobic activity. Cocci - Bacilli > Anaerobes + Bacilli, Cocci
- 19. Uses • Cefaclor: URTI’s • Cefuroxime: commonly acquired pneumonia, gonorrhoea and meningitis • Cefoxitin & cefotetan: peritonitis and diverticulitis and some gynecological infections (anaerobic infection)
- 20. Third Generation Cephalosporins Pharmacokinetics: • All these drugs distribute very well into body compartments • Adequate levels in the CSF regardless of inflammation, are achieved only with these 3rd gen • Thus these are used to treat meningitis • Ceftriaxone differs from others by its long plasma half life(7-8hrs) and high protein bound (90%)- OD • Metabolism is not major path for elimination • Cefotaxime is metabolized to active metabolite – desacetyl cefotaxime
- 21. Third Generation Cephalosporins • Cefoperazone and ceftriaxone are excreted through bile, so no dose adjustment requied for renal insufficiency • Urinary excretion is the major elimination route • Probenecid may increase the plasma half life • All are highly resistant to degradation by β-lactamases from gram-negative bacteria
- 23. Antimicrobial spectrum Gram-positive bacteria Streptococcus pyogenes, Viridans streptococci, Many Streptococcus pneumoniae, Modest activity against Staphylococcus aureus Gram-negative bacteria Escherichia coli, Klebsiella pneumoniae, Proteus spp. Haemophilus influenzae, Neisseria spp. Some Enterobacteriaceae. Anaerobic bacteria Atypical bacteria Spirochetes - Cocci, Bacilli > anaerobic org. Borrelia burgorferi + Bacilli, Cocci
- 24. Ceftriaxone: • Very effective in treating meningitis caused by N. meningitidis, Pneumococci, H. influenza and susceptible enteric gram-negative rods but not by Listeria monocytogenes • A single IM dose of 250mg is effective in gonorrhoae and chancroid • Excellent for treatment of community acquired pneumonia caused by pneumococci, H. influenzae and staph aureus • Lyme disease caused by Borrelia burgdorferi • Also efficacious in treating complicated UTI’s, abdominal sepsis and septicaemias • Also used to treat multi drug resistant typhoid fever (doses are high)
- 25. Cefotaxime: • Like ceftriaxone, has been utilized effectively for treating meningitis and community acquired pneumonia • A single 0.5-1g IM dose is effective in treating gonorrhoea • Has been used in respiratory, genitourinary, abdominal infections, septicaemia, anaerobic and hospital acquired infections
- 26. Cefoperazone: • More active than cefotaxime against pseudomonas (but less active than ceftadizime) • Good for Salmonella typhi and B. fragilis also • Used for pseudomonal UTI’s, bactreamia, and infections in immunocompromised patients • Other uses like meningitis, gonorrhoae and septicaemia are common to other drugs of this series
- 27. Ceftazidime: • Has excellent activity against pseudomonas (better than cefoperazone) and other gram-negative bacilli • Ceftadizime+aminoglycosides is the treatment of choice for pseudomonal meningitis • Also useful for nosocomial infections also
- 28. Ceftizoxime: • More active agaist B. fragilis than cefotaxime, otherwise similar
- 29. Cefixime: • Orally administered (200-400mg BD) • Cefixime is used to treat respiratory, urinary, biliary infections • In a single 400mg oral dose it provides effective treatment of uncomplicated gonorrhoea • Not effective against Staph. aureus and Pseudomonas Cefpodoxime: • Is similar to cefixime but it is active against Staph. aureus also
- 30. Fourth Generation Cephalosporins Oximinocephalosporins • Zwitterionic compounds • Enhanced ability to cross the outer membrane of Gram negative bacteria • Given by IM /IV • Plasma half life is 2hrs • Protein binding is only 20% • Widely distributed in tissues and body fluids • Accumulates well in CSF
- 31. Fourth Generation Cephalosporins • It is eliminated 85-90% through kidney • Pharmacokinetics of cefpirone is identical to cefepime expect that its protein binding is only 10% • Good affinity for the transpeptidase enzyme • Low affinity for some β-lactamases • Active vs. Gram +ve cocci and a broad array of Gram ve bacteria • Active vs. P. Aeruginosa
- 32. Antimicrobial spectrum Gram-positive bacteria Streptococcus pyogenes, Viridans streptococci, Many Streptococcus pneumoniae. Modest activity against Staphylococcus aureus Gram-negative bacteria Escherichia coli, Klebsiella pneumoniae, Proteus spp. Haemophilus influenzae, Neisseria spp. Many other Enterobacteriaceae, Pseudomonas aeroginosa. Anaerobic bacteria Atypical bacteria - Cocci, Bacilli > + Cocci. Noanaerobic , No + Bacilli
- 33. IV Gen. Uses • Hospital acquired pneumonia • Bactreamia and septicaemia • Also useful in UTI’s, RTI’s and as empiric therapy for febrile neutropinic patients
- 34. Adverse effects • Pain after IM inj. (cephalothin) • Diarrhoea (cephradine and cefoperazone) • Hypersensitivity reactions • Nephrotoxicity (cephaloridine, cephalothin and few other) • Bleeding (cefoperazone, ceftriaxone)(N-methyl thiotetrazole side chain at R2 position • Disulfiram like reaction (cefoperazone)
Notas del editor
- chancroids Veneralulcers Haemophilusduceryi
