23204949
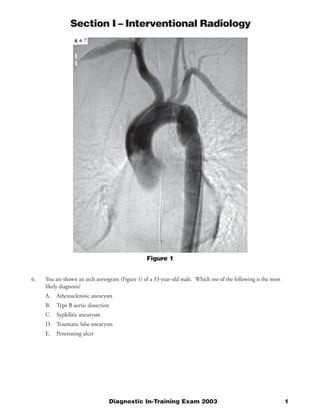
- 1. Section I – Interventional Radiology Figure 1 6. You are shown an arch aortogram (Figure 1) of a 33-year-old male. Which one of the following is the most likely diagnosis? A. Atherosclerotic aneurysm B. Type B aortic dissection C. Syphilitic aneurysm D. Traumatic false aneurysm E. Penetrating ulcer Diagnostic In-Training Exam 2003 1
- 2. Section I – Interventional Radiology Question #6 Findings: There is a focal dilatation of the proximal descending aorta, with linear defects projecting transversely across the aorta at the proximal and distal aspects of the focal dilatation. An endotracheal tube, a left chest tube, and a nasogastric tube are present. Rationales: A) Incorrect. The aorta and proximal great vessels appear normal with the exception of the findings described. Atherosclerotic disease is usually extensive and affects multiple vessels. It also usually affects older individuals. B) Incorrect. A Type aortic dissection involves the ascending aorta, which is normal in this case. Aortic dissection usually develops after age 50, and is more common in males. C) Incorrect. Syphilitic aneurysms more commonly affect the ascending aorta or arch. They are typically saccular in appearance and are a late complication of syphilis, occurring 10 to 30 years after the primary infection. D) Correct. The proximal descending aorta is the most common location of a traumatic false, or pseudoaneurysm, of the aorta. The presence of a chest tube, an endotracheal tube, and a nasogastric tube support the diagnosis of a traumatic injury. It most commonly occurs in young adults or adults, with a mean reported age of 35 in one large study. E) Incorrect. A penetrating ulcer is usually an eccentric, focal outpouching of the aorta. It occurs in older age groups and is associated with underlying atherosclerotic disease. Citations: Razzouk AJ, Gundry SR, Wang N, del Rio MJ, Varnell D, Bailey LL. Repair of traumatic aortic rupture: a 25-year experience. Arch Surg. Aug 2000;135(8):913-918; discussion 919. Kampmeier RH. The late manifestations of syphilis. Med Clin North Am 1964;48:667–697. Pressler V, McNamara JJ. Thoracic aortic aneurysm: natural history and treatment. J Thorac Cardiovasc Surg 1980;79:489–498. Tittle SL, Lynch RJ, Cole PE, et al. Midterm follow-up of penetrating ulcer and intramural hematoma of the aorta. J Thoracic Cardiovascular Surgery. Jun 2002;123(6):1051-1059. Hemley S, Kanick V, Kittredge R, Finby N. Dissecting aneurysms of the thoracic aorta: their angiographic demonstration. AJR 1964;91:1263 2 American College of Radiology
- 3. Section I – Interventional Radiology Figure 2 7. A 55-year-old female presents with recent onset of severe hypertension. You are shown an aortogram (Figure 2). Which one of the following is the best management option? A. Transcatheter thrombolysis B. Percutaneous transluminal angioplasty C. Primary arterial stenting D. Surgical aortorenal vein bypass E. Renal vein renin sampling Diagnostic In-Training Exam 2003 3
- 4. Section I – Interventional Radiology Question #7 Findings: There is irregularity of the left main renal artery, extending to the main bifurcation, with alternating areas of aneurysm and narrowing. The aorta and other opacified visceral vessels appear normal. Rationales: A) Incorrect. While the vessel appears irregular, there is no filling defect to suggest acute thrombus. Therefore, thrombolysis is not indicated. B) Correct. The alternating aneurysms and narrowing is characteristic of the “sting of beads” appearance of fibromuscular dysplasia (medial fibroplasia type). It usually affects the mid and distal segments of the main renal arteries, and is usually bilateral. Stenoses due to fibromuscular dysplasia of the renal artery respond favorably to percutaneous transluminal angioplasty (PTA), which is the treatment of choice.† Five-year patency rates are approximately 90%. C) Incorrect. While angioplasty with stent placement is typically necessary in patients with an atherosclerotic etiology of renovascular hypertension, angioplasty alone is highly effective for the treatment of the medial fibroplasia type of fibromuscular dysplasia. Stent placement following angioplasty in patients with fibromuscular dysplasia should be reserved for use in treating a hemodynamically significant dissection as a complication of angioplasty. D) Incorrect. Surgical aortorenal vein bypass is an effective treatment for severe, long segment stenoses of the main renal artery causing renovascular hypertension. These stenoses usually result from atherosclerotic disease. Angioplasty with stenting is less effective with long segment stenoses. E) Incorrect. Renal vein renin sampling is performed to evaluate for a renovascular cause for hypertension. In hypertensive patients with a documented unilateral etiology for the hypertension, as in the present patient, there is no additional information gained by performing renal vein renin sampling. The hypertension is presumed to be caused by the severe narrowing caused by the fibromuscular disease, and balloon angioplasty is indicated. Citations: Amsterdam EA, Couch NP, Christlieb AR. Renal vein renin activity in the prognosis of surgery for renovascular hypertension. Am J Med 1969;47:860. Itzchak Y, Katznelson D, Boichis H, Jonas A, et al. Angiographic features of arterial lesions in neurofibromatosis. AJR 1974;122:643. Klinge J, Willem PT, Puijilaert CB, Geyskes GG, Becking WB, Feldberg MA. Percutaneous transluminal renal angioplasty: initial and long-term results. Radiology 1989;171:501–506. Sacks D, Rundback JH, Martin LG. Renal angioplasty/stent placement, and hypertension in the year 2000. J Vasc Interv Radiol Sep 2000;11(8):949-953. 4 American College of Radiology
- 5. Section I – Interventional Radiology Figure 3 8. You are shown a venacavagram (Figure 3) of a 58-year-old male performed prior to placement of an inferior vena caval filter. Which one of the following is the most likely diagnosis? A. Venacaval occlusion with azygous continuation B. Extension of left renal vein tumor thrombus C. Duplicated inferior vena cava D. Hypovolemic shock E. Venacaval occlusion with recanalization Diagnostic In-Training Exam 2003 5
- 6. Section I – Interventional Radiology Question #8 Findings: The inferior vena cava is patent. The infrarenal segment is narrowed for the entire length. There is an absence of inflow artifact from the left iliac vein. There is a large inflow artifact from the left renal vein, and the inferior vena cava becomes much larger in diameter cephalad to the renal vein level. Rationales: A) Incorrect. The vena cava appears patent and in the normal location. The azygous vein would be located more medially. There would also likely be large collateral veins present. B) Incorrect. Left renal vein tumor thrombus would be possible if the filling defect in the inferior vena cava cephalad to the renal vein was an isolated finding. However given the other associated findings described above, this is less likely Another cause of thrombus in the IVC would be extension from a lower extremity deep venous thrombosis. However, filling defect would be evident extending cephalad from an iliac vein. C) Correct. All of the described findings are seen with a duplication of the inferior vena cava, with insertion of the duplication into the left renal vein. This explains the absence of inflow from the left iliac vein, and the larger than normal inflow artifact from the left renal vein. D) Incorrect. Hypovolemic shock can cause a diffuse decrease in the diameter of the inferior vena cava. However, the vena cava cephalad to the renal vein level appears normal. Common etiologies of hypovolemic shock are trauma or sepsis, and the patient has associated clinical findings of tachycardia and hypotension. E) Incorrect. The inferior vena cava appears normal in contour, and without filling defects. A venacaval occlusion with recanalization would result in an irregular vena caval contour, and chronic coaptations or filling defects. Collateral veins would also likely be present. Citations: Hicks ME, Malden ES, Vesely TM, Picus D, Darcy MD. Prospective anatomic study of the inferior vena cava and renal veins: comparison of selective renal venography with cavography and relevance in filter placement. J Vasc Interv Radiol. Sep-Oct 1995;6(5):721-729. Jeffrey RB Jr, Federle MP. The collapsed inferior vena cava: CT evaluation of hypovolemia. AJR 1988;150:431–432 3 Ney C. Thrombosis of inferior vena cava associated with malignant renal tumors. J Urol 1946;55:583–590. 6 American College of Radiology
- 7. Section I – Interventional Radiology Figure 4A Figure 4B 9. You are shown a celiac arteriogram (Figure 4A) and a superior mesenteric arteriogram (Figure 4B) of a 46-year-old male prior to hepatic chemoembolization. Which one of the following findings is present? A. Arc of Buehler B. Arc of Riolan C. Pathway of Winslow D. Anomalous right hepatic artery E. Anomalous left hepatic artery Diagnostic In-Training Exam 2003 7
- 8. Section I – Interventional Radiology Question #9 Findings: Figure 4A is a selective superior mesenteric arteriogram. There is a large vessel arising from the proximal portion of the superior mesenteric artery which course towards the right upper quadrant. The branching pattern of this vessel is consistent with a hepatic artery. Figure 4 B is a selective celiac arteriogram. Left gastric, left hepatic, gastroduodenal, and splenic arteries are identified. Rationales: A) Incorrect. An Arc of Buehler is a persistent embryologic ventral anastomosis between the celiac artery and the superior mesenteric artery. B) Incorrect. An arc of Riolan is an anastomotic artery between the left and middle colic arteries. C) Incorrect. The Pathway of Winslow is a collateral pathway through the epigastric arteries to provide blood flow to the lower extremities. In the presence of significant aortic stenosis or occlusion, blood can travel from the internal mammary arteries through the superior epigastric arteries, then retrograde through the inferior epigastric arteries and into the external iliac arteries. D) Correct. The described findings are diagnostic of an anomalous origin of the right hepatic artery, which occurs in approximately 10% of individuals. The anomalous vessel typically arises from the proximal portion of the superior mesenteric artery. E) Incorrect. As seen in Figure 4B, the left hepatic artery, and gastroduodenal artery, arise from the celiac artery. Citations: Kadir S. Atlas of Normal and Variant Angiographic Anatomy. W.B. Saunders. 1991 Lunderquist A. Arterial segmental supply of the liver: an angiographic study. Acta Radiol Suppl (Stockh) 1967;272:1. 8 American College of Radiology
- 9. Section I – Interventional Radiology Figure 5 10. A 57-year-old female presents with acute left chest pain two weeks following a hemorrhagic stroke. She is hemodynamically stable. You are shown a pulmonary angiogram (Figure 5). What should the next step in this patient’s management should be? A. Anticoagulation B. Thrombolytic therapy C. Percutaneous mechanical thrombectomy D. Contrast enhanced CT Scan E. Inferior vena cava filter placement Diagnostic In-Training Exam 2003 9
- 10. Section I – Interventional Radiology Question #10 Findings: Figure 5 is a selective left pulmonary angiogram. There are multiple filling defects in the left main pulmonary artery, and in the lobar and segmental branches. Rationales: A) Incorrect. Recent major abdominal, thoracic, or neurological surgery is risk factors for hemorrhage with anticoagulation therapy. Central nervous system events in the prior 6 months are also considered a contraindication to anticoagulation. Other contraindications include recent or ongoing hematuria, or gastrointestinal bleeding. B) Incorrect. There is no proven benefit to thrombolytic therapy or to mechanical thrombectomy compared with anticoagulation therapy in hemodynamically stable patients. However, in patients with hemodynamic instability or patients with poor cardiopulmonary reserve, more aggressive therapy such as thrombolysis or thrombectomy may be indicated. C) Incorrect. As noted above, there is no proven benefit to percutaneous thrombectomy in hemodynamically stable patients. D) Incorrect. The pulmonary angiogram is the gold standard imaging modality for the diagnosis of pulmonary embolism. A contrast enhanced CT scan would not add any additional useful information. At this point, a therapeutic decision is required E) Correct. The standard therapy for deep venous thrombosis and it major complication, pulmonary embolus, is anticoagulation. Placement of an inferior vena caval filter is preferred if anticoagulation is contraindicated. It protects the patient from further pulmonary emboli while the body autolyses the existing pulmonary thrombi. Contraindications for anticoagulation are noted above in option A. The recent stroke in this patient is a contraindication to anticoagulation and thus, the best alternative therapy is an inferior vena caval filter. Citations: Savin MA, Panicker HK, Sadiq S, Albeer YA, Olson RE. Placement of vena cava filters: factors affecting technical success and immediate complications. AJR Am J Roentgenol. Sep 2002;179(3):597-602. Riedel M. Acute pulmonary embolism 2: treatment. Heart. Mar 2001;85(3):351-360. 10 American College of Radiology
