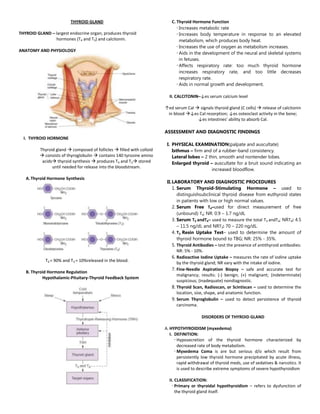
Thyroid Gland Disorders
- 1. THYROID GLAND THYROID GLAND – largest endocrine organ; produces thyroid hormones (T4 and T3) and calcitonin. ANATOMY AND PHYSIOLOGY I. THYROID HORMONE Thyroid gland composed of follicles filled with colloid consists of thyroglobulin contains 140 tyrosine amino acids thyroid synthesis produces T4 and T3 stored until needed for release into the bloodstream. A.Thyroid Hormone Synthesis T4 = 90% and T3 = 10%released in the blood. B. Thyroid Hormone Regulation Hypothalamic-Pituitary-Thyroid Feedback System C. Thyroid Hormone Function Increases metabolic rate Increases body temperature in response to an elevated metabolism, which produces body heat. Increases the use of oxygen as metabolism increases. Aids in the development of the neural and skeletal systems in fetuses. Affects respiratory rate: too much thyroid hormone increases respiratory rate, and too little decreases respiratory rate. Aids in normal growth and development. II. CALCITONIN–↓es serum calcium level ↑ed serum Cal signals thyroid gland (C cells) release of calcitonin in blood ↓es Cal resorption; ↓es osteoclast activity in the bone; ↓es intestines’ ability to absorb Cal. ASSESSMENT AND DIAGNOSTIC FINDINGS I. PHYSICAL EXAMINATION(palpate and auscultate) Isthmus – firm and of a rubber-band consistency. Lateral lobes – 2 thin, smooth and nontender lobes. Enlarged thyroid – auscultate for a bruit sound indicating an increased bloodflow. II.LABORATORY AND DIAGNOSTIC PROCEDURES 1. Serum Thyroid-Stimulating Hormone – used to distinguishsubclinical thyroid disease from euthyroid states in patients with low or high normal values. 2. Serum Free T4–used for direct measurement of free (unbound) T4; NR: 0.9 – 1.7 ng/dL 3. Serum T3 andT4– used to measure the total T3 andT4; NRT4: 4.5 – 11.5 ng/dL and NRT3: 70 – 220 ng/dL. 4. T3 Resin Uptake Test– used to determine the amount of thyroid hormone bound to TBG; NR: 25% - 35%. 5. Thyroid Antibodies – test the presence of antithyroid antibodies: NR: 5% - 10%. 6. Radioactive Iodine Uptake – measures the rate of iodine uptake by the thyroid gland; NR vary with the intake of iodine. 7. Fine-Needle Aspiration Biopsy – safe and accurate test for malignancy; results: (-) benign; (+) malignant; (indeterminate) suspicious; (inadequate) nondiagnostic. 8. Thyroid Scan, Radioscan, or Scintiscan – used to determine the location, size, shape, and anatomic function. 9. Serum Thyroglobulin – used to detect persistence of thyroid carcinoma. DISORDERS OF THYROID GLAND A. HYPOTHYROIDISM (myxedema) I. DEFINITION: Hyposecretion of the thyroid hormone characterized by decreased rate of body metabolism. Myxedema Coma is are but serious d/o which result from persistently low thyroid hormone precipitated by acute illness, rapid withdrawal of thyroid meds, use of sedatives & narcotics. It is used to describe extreme symptoms of severe hypothyroidism II. CLASSIFICATION: Primary or thyroidal hypothyroidism – refers to dysfunction of the thyroid gland itself.
- 2. Central hypothyroidism – the cause of thyroid dysfunction is failure of the pituitary gland, the hypothalamus, or both. Pituitary or secondary hypothyroidism - the cause of thyroid dysfunction is entirely a pituitary disorder Hypothalamic or tertiary hypothyroidism – the cause is a disorder of the hypothalamus resulting in inadequate secretion of TSH due to decreased stimulation of TRH. Cretinism – thyroid deficiency is present at birth III. CAUSES: Autoimmune disease (Hashimoto’s thyroiditis, Post Graves’ disease) Atrophy of thyroid gland with aging Therapy for hyperthyroidism: radioactive iodine, thyroidectomy Medications: lithium, iodine compounds, antithyroid medications Radiation to head & neck for treatment of head & neck cancers, lymphoma Infiltrative diseases of the thyroid (amyloidosis, scleroderma, lymphoma) Iodine deficiency & iodine excess IV. SIGNS AND SYMPTOMS: Hypotension Bradycardia Hypothermia Hyponatremia hypoglycemia respiratory failure death V. MANAGEMENTS: 1. Medical Management: a. Synthetic levothyroxine (Synthroid or Levothroid) is the preferred preparation for treating hypothyroidism a suppressing nontoxic goiters. 2. Nursing Management: a. Provide for comfort and safety b. monitor for infection or trauma c. provide warmth d. prevent heat loss & vascular collapse e. administer thyroid meds as ordered f. Monitor HR including rhythm. g. Instruct patient re: thyroid replacement therapy. h. Instruct on low-calorie, low-cholesterol, low-saturated fat diet. i. Assess for constipation & provide roughage. j. Provide for warm environment. k. Monitor for overdose of thyroid meds. l. Patent airway m. Keep patient warm & check V/S frequently n. Administer IV fluids & levothyroxine Na (Synthroid) o. Give IV glucose & corticosteroids p. Health teaching: Diet: low calorie, high protein S/Sx of hypothyroidism & hyperthyroidism Lifelong meds, dosage, desired effects, side effects. Stress-management techniques Exercise program B. HYPERTHYROIDISM I. DEFINITION: Hypersecretion of the thyroid gland. It is a type of thyrotoxicosis, a hypermetabolic clinical syndrome which occurs when there are elevated serum levels of T3 and/or T4. The most common underlying cause of hyperthyroidism is “Graves' disease”,an autoimmune disesase. In its most severe form, untreated hyperthyroidism may result in "thyroid storm," a condition involving high blood pressure, fever, and heart failure. (S/Sx: fever, tachycardia, hypotension, marked respiratory distress, pulmonary edema, irritability, apprehension, agitation, restlessness, confusion, seizures.) II. SIGNS AND SYMPTOMS: V/S: increased systolic BP, widened pulse pressure, tachycardia Excessive sweating Heat intolerance Increased bowel movements Tremor (usually fine shaking) Nervousness; agitation Rapid heart rate Weight loss despite of increased appetite Fatigue Enlarged thyroid Irregular and scant menstrual flow dyspnea exophthalmos In older patients, irregular heart rhythms and heart failure can occur. III. DIAGNOSTIC FINDINGS: blood tests that show a decreased thyroid-stimulating hormone (TSH) level and elevated T4 and T3 levels radioactive iodine uptake test and thyroid scan Thyroid scintigraphy IV. MANAGEMENTS: 1. Medical Management: Antithyroid drugs(carbimazole, methimazole, propylthiouracil) - drugs that inhibit the production of thyroid hormones. Beta-blockers (Propranolol (Inderal), atenolol (Tenormin), metoprolol (Lopressor)- used to treat high blood pressure, are a class of drugs that offset this effect, reducing rapid pulse associated with the sensation of palpitations, and decreasing tremor and anxiety. Radioactive Iodine Therapy-destroy the overactive thyroid cells; treat toxic adenomas,multinodular goiter and thyrotoxicosis. Iodine preparations (SSKI, Lugol’s Solution) - decrease size & vascularity of the thyroid gland; palatable if diluted with water, milk or juice; give through straw tp prevent staining of teeth; takes 2-4 weeks before results are evident. 2. Surgical Management: Thyroidectomy-removal of thyroid tissue that was producing the excessive thyroid hormone. PRE-OPERATIVE CARE: Assess V/S, weight, electrolyte & glucose level Teach DBE & coughing as well as how to support neck in post-op period when coughing & moving Administer antithyroid meds etc. to prevent thyroid storm POST-OP CARE: Monitor for respiratory distress & have tracheostomy set, O2 & suction machine at bed side Maintain semi-Fowler’s position to reduce edema Immobilize head with pillows/sandbags; prevent flexion & hyperextension of neck Check surgical site for edema & bleeding
- 3. Limit client talking & assess for hoarseness Assess for laryngeal nerve damage…high-pitched voice, stridor, dysphagia, dysphonia & restlessness Monitor for signs of hypocalcemia & tetany & have calcium gluconate at bed side 3. Nursing Management: Protect from stress: private room, restrict visitors, quiet environment. Promote physical & emotional equilibrium:cool, quiet, cool well ventilated environment; eye care: sunglasses to protect from photophobia, protective drops (methylcellulose) to soothe cornea; diet: high calorie, protein, vit. B; avoid stimulants Prevent complications: give medications as ordered. Monitor for thyroid storm. Health teaching: stress reduction techniques; importance of medications; methods to protect eyes from environment; s/sx of “Thyroid Storm”. Measure neck circumference daily to check for progression of thyroid enlargement. Weigh patient. C. THYROIDITIS I. DEFINITION: The inflammation of the thyroid gland. II. TYPES a.Acute thyroiditis Definition: Is a rare disorder caused by infection of the thyroid gland by bacteria, fungi, mycobacteria, or parasites Causes: Staphylococcus aureus are the most common S & Sx: Anterior neck pain and swelling, fever, dysphagia, dysphonia, pharyngitis, or pharyngeal pain Examination: Reveals warmth, erythema (redness), and tenderness of the thyroid gland Treatment: Antimicrobial agents and fluid replacement, surgical incision and drainage may be needed if an abscess is present b.Subacute Thyroiditis Definition: May be of two kinds: Subacute granulomatous thyroiditis and painless thyroiditis Subacute Granulomatous Thyroiditis Definition: Is an inflammatory disorder of the thyroid gland that predominantly affects women between 40-50 ages of years. It is also associated with a viral respiratory infection and has a summer peak incidence that coincides with coxsackievirus groups A and B and echovirus infections. Causes: Virus S & Sx: Myalgias, pharyngitis, low-grade fever, and fatigue, painful swelling at the anterior neck, symmetric enlargement of the thyroid, difficulty of swallowing Treatment: NSAIDs to relieve neck pain, Acetylsalicylic acid (aspirin) is avoided if Sx of hyperthyroidism occur, oral corticosteroids, follow up monitoring Painless thyroiditis (Subacute Lymphocytic Thyroiditis) Definition: Often occurs in the postpartum period and is thought to be an autoimmune process S & Sx: Sx of hyperthyroidism and hypothyroidism Treatment: Directed at symptoms, and a yearly follow-up is recommended c. Chronic Thyroiditis Definition: Also known as Hashimoto’s disease or chronic lymphocytic thyroiditis, it occurs most frequently in women between 30-50 ages of years.Cell mediated immunity may play a significant role in the pathogenesis of chronic thyroiditis and there may be a genetic predisposition to it. Cause: Unknown S & Sx: initially the Sx of hyperthyroidism, such as restlessness, tremors, chest pain, increased appetite, diarrhea, moist skin, heat intolerance, and weight loss. III. DIAGNOSTIC TESTS:Immunofluorescent assay, a test that detects antigens on cells using an antibody with a fluorescent tag, detects antithyroid antibodies. TSH is elevated, while (T3) and (T4) levels are low. A thyroid scan is also done. IV. TREATMENT: The objective is to reduce the size of the thyroid gland and the prevent hypothyroidism, thyroid hormone therapy D.THYROID TUMORS Tumors are classified on the basis of: Being benign or malignant The presence or absence of thyrotoxicosis The diffuse or irregular quality of glandular enlargement. If the enlargement is sufficient to cause a visible swelling in the neck, the tumor is referred to as GOITER. Grades of goiter: Barely visible and producing disfigurement. Symmetric and diffuse Nodular Accompanied by hyperthyroidism Toxic or non-toxic I. ENDEMIC (IODINE-DEFICIENT) GOITER SIMPLE OR COLLOID GOITER Most common type of goiter encountered chiefly in geographic regions where the natural supply of iodine is deficient. (e.g., Great Lakes areas of the United States) May be caused by an intake of large quantities of goitrogenic substance in patients with unusually susceptible glands. These substances include excessive amounts of iodine or lithium, which is used in treating bipolar disorders. Represents a compensatory hypertrophy of the thyroid gland, caused by stimulation by the pituitary gland. Its production increases if there is subnormal thyroid activity, as when insufficient iodine is available for production of the thyroid hormone. Such goiters usually cause no symptoms, except for the swelling in the neck. SSKI, a supplementary iodine which is prescribed to suppress the pituitary’s thyroid-stimulating activity Ensuring a preoperative euthyroid state through treatment with antithyroid medication and iodide will minimize the risk of postoperative complications. Providing children in iodine-poor regions with iodine compounds can prevent simple or endemic goiter. The introduction of iodized salt has been the single most effective means of preventing goiter in at-risk populations. II. NODULAR GOITER Some thyroid glands are nodular because of areas of hyperplasia (overgrowth) No symptoms may arise as a result of this condition, but not uncommonly these nodules slowly increase in size, with some
- 4. descending into the thorax, where they cause local pressure symptoms. Some nodules become malignant Some are associated with a hyperthyroid state III. THYROID CANCER Much less prevalent than other forms of cancer; however it accounts for 90% of endocrine malignancies According to American Cancer Society, such cases are more occurring to men than the women. Types: Papillary adenocarcinoma 70%- most common, least aggressive, asymptomatic, starts in childhood or early adult life/ more aggressive in adults life, metastasizes along the lymphatics if untreated Follicular adenocarcinoma 15%- appears after 40 yrs. of age, encapsulated, feels elastic or rubbery on palpation, spreads through the blood stream to bone, liver and lung, prognosis is not as favorable as papillary adenocarcinoma Medullary 5%- after 50 yrs. of age, occurs as part of multiple endocrine neoplasia (MEN), hormone producing tumor causing endocrine dysfunction symptoms, metastasizes by lymphatics and bloodstream, moderate survival rate Anaplastic 5%- after 60 yrs. of age, hard, irregular mass that grows quickly and spreads by direct invasion to adjacent tissues, may be painful or tender, survival is usually less than 6 months Thyroid lymphoma 5%- after 40 yrs. of age, may have history of goiter, hoarseness, dyspnea, pain and pressure, good prognosis External radiation of the head, neck or chest in infancy and childhood increases the risk of thyroid carcinoma. Appears to increase 5 to 40 years after Consequently, people who underwent radiation treatment or were otherwise exposed to radiation as children should consult a physician and request an isotope thyroid scan as part of the evaluation. Assessment and Diagnostic Findings Single, hard, and fixed lesions on palpation suggest malignancy usually associated with cervical lymphadenopathy. Thyroid Function Test- helpful in evaluating thyroid nodules and masses. Needle Biopsy- used as an outpatient procedure to make a diagnosis of the thyroid Cancer - Procedure is safe and usually requires only a local anesthesia. Large Bore needle- may be used when the result of the standard biopsy are in convulsive or with rapidly growing tumors. Additional Diagnostic Studies Ultrasound MRI CT Thyroid Scan Radioactive iodine uptake test Thyroid Suppression Test Medical Management Surgical Removal- Treatment of Choice for Thyroid Carcinoma Total or near-total Thyroidectomy Modified neck dissection- performed if there is lymph node involvement Ablation Procedure- carried out with radioactive iodine to eradicate residual thyroid tissue if the tumor is radiosensitive. Radioactive Iodine- also maximizes the chance of discovering thyroid metastasis at a later date if total body scans are carried out. After Surgery Administer; Thyroid Hormone- to prevent hypothyroidism Thyroxine Several routes for administering radiation therapy to the thyroid or tissue of the neck: 1. Oral Administration of radioactive iodine 2. External administration of radiation therapy Nursing Management Important preoperative goals are to gain the patient’s confidence and reduce anxiety. a. PROVIDING PREOPERATIVE CARE The nurse instructs the patient about the importance of eating a diet high in carbohydrates and proteins. A high daily caloric intake. The patient is reminded to avoid tea, coffee, cola, and other stimulants. The nurse also informs the patient about the purpose of preoperative tests, if they are to be performed, and explains what preoperative preparations to expect. Preoperative teaching includes demonstrating to the patient how to support the neck with the hands after surgery. b. PROVIDING POSTOPERATIVE CARE The nurse periodically assesses the surgical dressings and reinforces them when necessary. When the patient is in a recumbent position, the nurse observes the sides and the back of the neck as well as the anterior dressing for bleeding. Difficulty in respiration occurs as a result of edema of the glottis, hematoma formation, or injury to the recurrent laryngeal nerve. The intensity of pain is assessed and analgesic agents are administered as prescribed for pain. Intravenous fluids are administered during the immediate postoperative period. The patient is advised to talk as little as possible to reduce edema to the vocal cords. An overbed table may be used to provide easy access to items that are needed frequently, such as paper tissues, water pitcher and glass, and a small emesis basin. The patient is usually permitted out of bed as soon as possible and is encouraged to eat foods that are easily eaten. c. MONITORING AND MANAGINGPOTENTIAL COMPLICATIONS Hemorrhage, hematoma formation, edema of the glottis, and injury to the recurrent laryngeal nerve are common complications. Producing a disturbance in calcium metabolism. Tetany- this type is usually treated with intravenous calcium gluconate. d. PROMOTING HOME AND COMMUNITY-BASED CARE Teaching Patients Self-Care. The patient may be discharged the evening of surgery or within 1 or 2 days. The patient and family need to be knowledgeable about the signs and symptoms of the complications that may occur and those that should be reported. The nurse explains to the patient and family the need for rest, relaxation, and nutrition. The patient is permitted to resume his or her former activities and responsibilities completely once recovered from surgery. Continuing Care. If indicated, a referral to home care is made. The home care nurse assesses the patient’s recovery from surgery. The nurse also assesses the surgical incision and reinforces instruction about limiting activities that put strain on the incision and sutures.
- 5. Family responsibilities and factors relating to the home environment that produce emotional tension have often been implicated as precipitating causes of thyrotoxicosis. A home visit provides an opportunity to evaluate these factors and to suggest ways to improve the home and family environment. The nurse gives specific instructions regarding follow-up visits to the physician or the clinic, which are important for monitoring the thyroid status.
