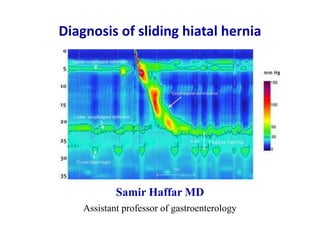
Diagnosis of Sliding Hiatal Hernia with HRM
- 1. Diagnosis of sliding hiatal hernia Samir Haffar MD Assistant professor of gastroenterology
- 2. Diagnosis of sliding hiatal hernia ① Types of hiatal hernia ② Barium swallow radiography ③ Upper gastrointestinal endoscopy ④ Standard esophageal manometry ⑤ High resolution manometry (HRM)
- 3. ① Types of hiatal hernia
- 4. Type of hiatal hernia Normal anatomy Type I Type II Type III sliding hiatal hernia paraesophageal hernia mixed hiatal hernia most common (95%) Duranceau A. Dis Esophagus 2016;29(4):350–66.
- 5. Normal anatomy Ishimura N et al. Dig Endoscopy 2009;21:213–218. Distance between squamous-columnar junction and diaphragmatic indentation < 2 cm
- 6. Hiatal hernia type 1 sliding hiatal hernia most common form (95%) Duranceau A. Dis Esophagus 2016;29(4):350–66. Distance between squamous-columnar junction and diaphragmatic indentation > 2 cm
- 7. Endoscope emerges from gastroesophageal junction which is in normal position The endoscope retroflexes and looks at stomach fundus herniated through diaphragm Duranceau A. Dis Esophagus 2016;29(4):350–66. Hiatal hernia type 2 para-esophageal hiatal hernia
- 8. Duranceau A. Dis Esophagus 2016;29(4):350–66. Forward view of massive herniation observed from gastroesophageal junction at 30 cm from incisors Retroflexed view under the diaphragm of a type III hernia and an enlarged hiatus Hiatal hernia type 3 mixed hiatal hernia Forward view Retroflexed view
- 9. ② Barium swallow radiography
- 10. Kahrilas PJ et al. Best Practice Research Clin Gastroenterol 2008;22(4):601–616. Anatomical features of sliding hiatal hernia viewed radiographically Ring A: Superior margin of LES (highest pressure zone in LES) Ring B: At squamocolumnar junction, present in 15% of persons Division of phrenic ampulla into oesophageal vestibule (A to B ring) & HH (B ring to sub-diaphragmatic stomach) Hiatal hernia: Distance from B ring to hiatus > 2 cm
- 11. Barium swallow radiography Kahrilas PJ et al. Best Practice Research Clin Gastroenterol 2008;22(4):601–616. Well developed ring A and ring B Hiatal hernia defined by distance from B ring to hiatus > 2 cm Image in early swallow: hiatus hernia indicated by black bracket Image in late swallow: hiatus hernia indicated by white bracket Size estimate of hiatal hernia depends on when in the swallow sequence the measurement is made Early swallow Late swallow
- 12. Limitations of barium swallow radiography • Not all of previous structures always demonstrable radiographically • Commonly, A ring but not B ring is evident and thus the limits of measurement defining hiatus hernia become arbitrary • B ring located at SCJ only demonstrable in only 15% of individuals • Measurement of B ring to hiatus depends on timing of swallow: early swallow, late swallow or between swallows • Frequency of sliding hiatus hernia increased in case of abdominal compression during barium swallow imaging Prevalence of sliding hiatal hernia vary enormously from 10 – 80% Identification of type 1 hernia < 3 cm by radiography is unreliable Kahrilas PJ et al. Best Practice Research Clin Gastroenterol 2008;22(4):601–616.
- 13. Hyun JJ et al. Gut and Liver 2011;5(3):267–277. Barium swallow radiography When sliding hiatal hernia is > 3 cm, is its presence obvious because gastric folds are evident traversing diaphragm both during swallow-induced shortening & at rest diaphragmatic indentation diaphragmatic indentation
- 14. ③ Upper gastrointestinal endoscopy
- 15. Upper gastrointestinal endoscopy forward view Sliding hiatus hernia diagnosed when distance between squamocolumnar junction and diaphragmatic impression > 2 cm Accuracy and reproducibility of such measurements have not been tested Kahrilas PJ et al. Best Practice Research Clin Gastroenterol 2008;22(4):601–616.
- 16. Kahrilas PJ et al. Best Practice Research Clin Gastroenterol 2008;22(4):601–616. Gastro-esophageal area open all the time Squamous epithelium of distal esophagus seen from retroflexed view Sliding hiatal hernia is always present with this deformity Upper gastrointestinal endoscopy retroflexed view
- 17. Limitations of upper gastrointestinal endoscopy • Extremely patulous hiatus: Difficulty to precisely localize the crural diaphragm • Excess insufflation of stomach Might exaggerate the apparent size of hernia • Barrett’s metaplasia: Difficulty to ascertain location of native squamocolumnar junction HH: hiatal hernia Kahrilas PJ et al. Best Practice Research Clin Gastroenterol 2008;22(4):601–616. Little study of sensitivity of endoscopic measurement of sliding HH Endoscopy suffers from similar limitations to barium swallow Identification of type I hernia < 3 cm with endoscopy is unreliable
- 18. ④ Standard esophageal manometry
- 19. Standard esophageal manometry in hiatal hernia one circumferential sensor distally & pulled out by 0.5 cm steps Fornari F et al. Dig Liver Dis 2009;41:886–890. Dual high-pressure zones at gastro-esophageal junction Distal hump corresponds to diaphragmatic crura Proximal hump corresponds to lower esophageal sphincter
- 20. Fornari F et al. Dig Liver Dis 2009;41:886–890. Diagnostic accuracy of conventional manometry Endoscopy as the referential technique Percentage 95% confidence interval Sensibility 28% 19 – 40 Specificity 97% 93 – 99 Positive predictive value 82% 63 – 92 Negative predictive value 76% 73 – 79 Study of 215 consecutive patients with or without HH
- 21. ⑤ High resolution manometry
- 22. Normal HRM following a wet swallow EGJ: esophago-gastric junction – LES: lower esophageal junction Conklin JL. J Neurogastroenterol Motil 2013;19(3):281–294. UES: Upper esophageal sphincter S1: Striated esophageal muscle TZ: Transition zone from striated to smooth muscle S2: Proximal esophageal smooth muscle S3: Distal esophageal smooth muscle S4: LES repositioning itself at its resting position EGJ: Esophago-gastric junction Composed of tonic LES contraction & phasic crural diaphragm contraction with inspiration
- 23. • Thoracic cavity: Pressure decreases during inspiration Pressure increases during expiration • Abdominal cavity: Pressure increases during inspiration Pressure decreases during expiration • Pressure inversion point: Point at which pressure across EGJ during “PIP” inspiration becomes negative Indicates location of crural diaphragm Esophago-gastric junction Composed of tonic LES contraction and cyclic crural contraction Conklin JL. J Neurogastroenterol Motil 2013;19(3):281–294.
- 24. Esophago-gastric junction in HRM • Type I: no separation between LES & CD (normal) • Type II: 1 – 2 cm separation (small hiatal hernia) • Type III: > 2 cm of separation (large hiatal hernia) Distance between maximal LES pressure & maximal CD pressure CD: crural diaphragm – HRM: high resolution manometry – LES: lower esophageal sphincter Tolone S et al. United Eur Gastroenterol J 2018;6(7)981–989.
- 25. Esophago-gastric junction type I E: expiration – EGJ: esophago-gastric junction – I: inspiration – LES: lower esophageal junction Conklin JL. J Neurogastroenterol Motil 2013;19(3):281–294. ** tonic LES contraction * cyclic crural contraction with respiration red arrowhead: location of pressure inversion point (PIP) EGJ type 1: normal coincident LES and crural diaphragm distancefromnares(cm) I E
- 26. Esophago-gastric junction type II E: expiration – EGJ: esophago-gastric junction – I: inspiration – LES: lower esophageal junction Conklin JL. J Neurogastroenterol Motil 2013;19(3):281–294. ** tonic LES contraction * cyclic crural contraction with respiration red arrowhead: location of pressure inversion point (PIP) EGJ type 2: small sliding hiatal hernia LES-crural diaphragm separation 1-2 cm distancefromnares(cm)
- 27. E: expiration – EGJ: esophago-gastric junction – I: inspiration – LES: lower esophageal junction Conklin JL. J Neurogastroenterol Motil 2013;19(3):281–294. Esophago-gastric junction type III ** tonic LES contraction * cyclic crural contraction with respiration red arrowhead: location of pressure inversion point (PIP) EGJ type 3: large sliding hiatal hernia LES-crural diaphragm separation > 2 cm distancefromnares(cm) I E
- 28. Types of esophageal-gastric junction Distance between maximal LES pressure & maximal CD pressure CD: crural diaphragm – HRM: high resolution manometry – LES: lower esophageal sphincter Tolone S et al. United Eur Gastroenterol J 2018;6(7)981–989. Type I Type II Type III Coincident LES & CD normal 1 – 2 cm separation small hiatal hernia > 2 cm separation large hiatal hernia
- 29. Large sliding hiatal hernia Three high pressure zones: UES, LES and crural diaphragm Swallow followed by propagated contraction along esophagus LES & crural diaphragm separated by more than 2 cm LES: lower esophageal sphincter – UES: upper esophageal sphincter Roman S et al. BMJ 2014;349:g6154.
- 30. Diagnostic accuracy of radiography, endoscopy and HRM Open surgical assessment as gold standard AUROC: area under receiver operating characteristic – HRM : high resolution manometry Tolone S et al. United Eur Gastroenterol J 2018;6(7)981–989. Study of 100 consecutive patients Radiography Gastroscopy HRM Sensibility 70% 96% 94% Specificity 98% 74% 91% Positive predictive value 97% 81% 93% Negative predictive value 74% 95% 93% Kappa value 0.66 0.72 0.85 AUROC – – 0.929
- 31. Conclusion • HRM can accurately diagnose sliding hiatal hernia with high sensibility and specificity • HRM seems to classify sliding hiatal hernia (no hiatal hernia, small or large size) better than radiography and endoscopy • HRM reaches optimal agreement w open surgical assessment HRM: high resolution manometry
- 32. Thank You