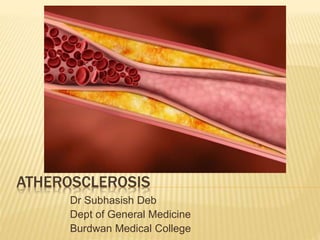
Atherosclerosis
- 1. ATHEROSCLEROSIS Dr Subhasish Deb Dept of General Medicine Burdwan Medical College
- 2. ATHEROSCLEROSIS A condition characterized by : Hardening of arteries with loss of elasticity Characterized by intimal lesions called atheroma that protrude into the vessel lumen
- 3. ARTERIOSCLEROSIS Hardening of arteries with loss of elasticity 3 types: 1. Monckeberg medial calcific sclerosis 2. Atherosclerosis 3. Arteriolosclerosis
- 4. MONCKEBERG MEDIAL CALCIFIC SCLEROSIS Most benign Medium sized arteries – radial, ulnar Calcification in MEDIA, usually age related, 60-70yrs Calcification does not encroach into intima, hence no dangerous complications Usually involves U/L arteries
- 6. ATHEROSCLEROSIS No 1 killer in western world Disease of INTIMA Formation of fibro fatty plaques Involves: Elastic arteries - aorta, carotid, iliac Medium sized muscular arteries – coronary, popliteal, circle of willis In smaller vessles they cause occlusion and in larger ones medial weakening - aneurysms
- 8. ARTERIOLOSCLEROSIS 1. Hyaline arteriolosclerosis Deposition of amorphous hyaline in media Seen in – senile changes, Essential HTN, DM 2. Hyperplastic arteriolosclerosis Arterioles become narrow Media has concentric layers of smooth muscle hypertrophy – onion skin Seen in Malignant hypertension
- 11. PATHOGENESIS OF ATHEROSCLEROSIS Hypothesis: 1. Intimal cellular proliferation 2. Repetitive formation and organization of thrombi 3. Response - to – injury A process of chronic inflammation in response to a chronic or acute injury Key players: 1. Modified lipoproteins 2. Monocyte derived macrophage 3. T lymphocytes 4. Smooth muscles from media
- 12. Atherogenesis: developmental process of atheromatous plaque Characterized by remodeling of arteries leading to sub endothelial accumulation of fatty substances called plaques A slow process, developed over many years, 1st lesion being fatty dots
- 13. I. ENDOTHELIAL INJURY It leads to: Increased vascular permeability Leukocyte adhesion Thrombus formation What causes injury?? a) Haemodynamic stress: plaques tend to occur in areas of disturbed blood flow 1. Branch points 2. Ostia of vessels 3. Post wall of abd aorta
- 14. Laminar flow of blood is protective. It suppresses expression of leukocyte adhesion molecules Augments production of NO by endothelial cells which not only cause vasodilatation but also acts as local anti-inflmmatory autacoid - limiting adhesion molecule expression Laminar flow stimulates production of superoxide dismutase from endothelial cells – anti oxidant
- 16. b) Lipid Abnormalities Inc LDL Inc lipoprotein a Dec HDL How these lipid abnormalities are bad? Inc LDL means more cholesterol goes to peripheries They damage endothelial cells 1. Make them more permeable – more lips go inside 2. NO released from endothelial cells do not allow platelets to stick. But excess lipids – formation of free radicals which neutralize NO – platelets
- 17. 3. LDL in intima gets oxidized and plays role in atheroma formation Other risk factors causing endothelial injury: c) Smoking d) Toxins e) Microbes – CMV, chlamydia Pneumoniae f) Homocystine g) Inflammatory cytokines
- 18. INITIATION OF LESION: Initial lesions are fatty dots and streaks Accumulation of lipoprotein particles may not result form increased permeability or ‘leakiness’ Lipoprotein may accumulate as they bind to some GAG in the extracellular matrix
- 19. II. ACCUMULATION OF LIPOPROTEINS IN VESSEL WALL Usually ldl It gets oxidized
- 20. III. MONOCYTE ADHESION TO ENDOTHELIUM Healthy endothelium does not express adhesion molecules for WBC VCAM-1 (vascular endothelial cell adhesion molecule expressed in response to injury Monocytes convert to macrophages and bind to these VCAM-1 and enter the sub endothelial space
- 21. They release cytokines that stimulates lymphocytes. These lymphocytes also produce chemical mediators that stimulate macrophages. Macrophages release: 1. IL 1 2. TNF 3. MCP 1 (monocyte chemotactic protein 1) Lymphocytes release: 1. Gamma IF
- 23. IV. SMOOTH MUSCLE CELL PROLIFERATION AND EXTRA CELLULAR MATRIX PRODUCTION The next major player coming rushing to the site is Smooth Muscle cells from the MEDIA Due to the environment with theses chemicals, the SMCs change their behavior. Their contractile protein dissolves and they behave primitively – only proliferation. SMC also release ECM and collagen
- 24. FOAM CELLS Derived from macrophages and smooth muscle cells that have taken up a lot of cholesterol Macrophages release ros that oxidises LDL Oxidized LDL is more delicious so taken up more my macrophages and SMC – foam cells
- 26. Some of the foam cells overladen with lipid will burst and become necrotic. Their contents leak out, so a lipid core is formed. The SMCs which are multiplying are present both above and below this lipid core encircling it SMCs near the endothelial surface multiply more due the proximity to Growth Factors. They secrete GAG and collagen extracellularly –FIBRIN CAP
- 27. Fibrin cap is composed of: Smooth muscle cells Collagen, GAG Some lymphocytes Some macrophages
- 31. Below the fibrous cap lies the core Growth factors go to the shoulder of the lesion and stimulate vasa vasorum. So new vessels grow in from the sides. (play imp role in plaque Hg)
- 33. RISK FACTORS FOR ATHEROSCLEROSIS Fixed risk factors: 1. Age 2. Sex: M>>F (women protected until menopause – estrogen) 3. Genetics : htn, dm, hypercholesterlemia have a genetic component
- 34. Modifiable risk factors: 1. Hyperlipidemia: Omega 3 fatty acid in fish oil is good Baked products with PUFA bad 2. Hypertension : responsible for both initiation and progression 3. Tobacco smoking 4. DM 5. Homocystinuria : some people develop this due to folate & B6 def 6. Chronic inflammation 7. Obesity 8. Type A personality
- 35. AMERICAN HEART ASSOCIATION CLASSIFICATION OF ATHEROSCLEROSIS 1. Type 1/ initial lesion/ fatty dots: 1mm yellow dots Starts appearing in early life, even at 1yr in aorta Almost all children have such lesion by 10yrs Contain just few scattered macrophages
- 37. 2. Type 2 lesions/ fatty streaks: Linear kesons formed by fusion of dots Upto 1cm Develops at early age ~10yrs They are precursors of mature plaques But their location are not similar to location of plaques (thus every fatty streak is not going to grow into a plaque) Consists of more macrophages, more foam cells and some T cells
- 39. 3. Type 3 lesion/ intermediate lesions: Lipids are present not only in macrophages but also extracellularly. Hence different from II. 4. Type 4/ atheromatous plaque: Presence of core of lipid surrounded by foam cells 5. Type 5/ fibroatheromatous lesion: Neovascularization at shoulder Fibrin cap Central core of lipid + necrotic debri
- 40. 6. Type 6/ complicated lesions/ complicated atheroma: Surface defect in endothelium Presence of platelet plug and fibrin on the lumen side = thrombus There may by Hg. Blood comes from ruptured vessels in plaque. Intra plaque hg enlarges and blocks lumen of vessel Growth of lesions 1-4 manily depends on acculumation of lipid in lesion Growth of 5 due to accumulation of SMC and collagen Growth of 6 by blood or thrombus
- 42. MOST COMMON SITES OF ATHEROSCLEROSIS 1. Abdominal aorta (infra renal) 2. Coronary art 3. Popliteal art 4. Carotid art 5. Circle of willis (in this order)
- 43. COMPLICATIONS 1. Fibrosis 2. Calcification 3. Erosions 4. Ulcerations 5. Rupture 6. Platelet plug formation 7. Thrombus formation 8. Atheroembolism 9. Intra plaque haemorrhage
- 44. 1. Erosion and ulcerations: When endothelium is removed and underlying basement membrane of intima exposed. This BM is highly thrombogenic and will attract platelets. 2. Fissuring and rupture: Damage goes deeper and exposes the lipid. (ie both endothelium and BM lost) When very narrow called fissure, when wide = rupture 21 endothelium Basement membrane
- 45. THANK YOU
