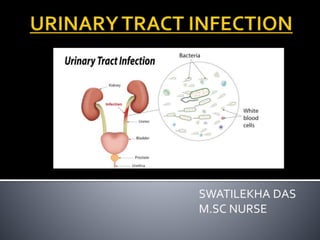
Urinary Tract Infection with Nursing Management
- 2. A urinary tract infection (UTI) is a bacterial infection in part of the urinary tract. When it affects the lower urinary tract, it is known as a simple cystitis (a bladder infection).When it affects the upper urinary tract, it is known as pyelonephritis (a kidney infection). UTI is 50 times more common in women, with about 5 per cent per year developing symptoms. UTI is uncommon in men below 60 years of age, but the frequency is similar in men and women in older age groups.
- 3. A urinary tract infection (UTI) is an infection involving the kidneys, ureters, bladder, or urethra.These are the structures that urine passes through before being eliminated from the body.
- 4. Escherichia coli [ causes 80% of cases ] Enterococcus Klebsiella Enterobactor Proteus Pseudomonas Staphylococcus Candida albicans
- 5. Several classification systems can be used for UTIs.Therefore depending on the site involved, the clinical presentation of UTI is as follows: Asymptomatic bacteriuria- is a significant number of bacteria in the urine that occurs without usual symptoms such as burning during urination or frequent urination. Acute cystitis- indicates inflammation of the bladder wall. Acute pyelonephritis- implies inflammation (usually due to infection) of the renal parenchyma and collecting system. Acute urethritis- means inflammation of the urethra. Acute prostatitis- is a serious bacterial infection of the prostate gland.
- 6. A urinary tract infection is said to be complicated if: it is in the upper tract the person has diabetes mellitus the person is pregnant the person is male the person has a weakened immune system (immunocompromised) because of another illness.
- 7. 1. Factors increasing urinary stasis Intrinsic obstruction(stone, tumor of urinary tract, urethral strictures, BPH) Extrinsic obstruction(tumor, fibrosis compressing urinary tract) Urinary retention(including neurogenic bladder and low bladder wall compliance) Renal impairment 2. Foreign bodies Urinary tract calculi Catheters ( indwelling external condom catherter, urethral stent, intermittent catheterization) Urinary tract instrumentation( cystoscopy, urodynamics) 3. Anatomic factors Congenital defects leading to obstruction or urinary stasis Fistula exposing urinary system to skin, vagina, or fecal stream Shorter female urethra and colonization from normal vaginal flora obesity
- 8. 4. Factors comprising immune response Ageing Human immunodeficiency virus infection Diabetes mellitus 5. Functional disorders Constipation Voiding dysfunction 6. Other factors Pregnancy Hypoestrogenic state Multiple sex partners Poor personal hygiene
- 9. The urinary tract above the urethra is normally sterile. Several mechanical and physiologic defence mechanisms include normal voiding with complete emptying of the bladder, ureterovesical junction competence and peristaltic activity that propels urine toward the bladder. Antibacterial characteristics of urine are maintained by an acidic pH (<6.0) high urea concentration, and abundant glycoproteins that interfere with the growth of bacteria. These defence mechanisms assist in maintaining sterility and preventing UTIs.
- 10. A strong, persistent urge to urinate A burning sensation when urinating Passing frequent, small amounts of urine Urine that appears cloudy Urine that appears red, bright pink or cola-colored — a sign of blood in the urine Strong-smelling urine Pelvic pain, in women — especially in the center of the pelvis and around the area of the pubic bone
- 11. History taking with detailed clinical manifestations Physical examination UrineTests Urinalysis- Urine Culture- Clean-Catch Sample-
- 12. Ultrasound- Ultrasound is a noninvasive imaging test that can be used to screen for hydronephrosis (obstructions of the flow of urine). X-Rays- Special x-rays can be used to screen for structural abnormalities, urethral narrowing, or incomplete emptying of the bladder. Due to the possible risks to the fetus, x-rays are not performed on pregnant women. Voiding cystourethrogram- It is an x-ray of the bladder and urethra.To obtain a cystourethrogram, a dye, called contrast material, is injected through a catheter inserted into the urethra and passed through the bladder. An intravenous pyelogram (IVP)- It is an x-ray of the kidney. For a pyelogram, the contrast matter is injected into a vein and eliminated by the kidneys. In both cases, the dye passes through the urinary tract and reveals any obstructions or abnormalities on x-ray images.
- 13. Cystoscopy- Cystoscopy is used to detect structural abnormalities, interstitial cystitis, or masses that might not show up on x-rays during an IVP.The patient is given a light anesthetic, and the bladder is filled with water.The procedure uses a cystoscope, a flexible, tube-like instrument that the urologist inserts through the urethra into the bladder ComputedTomography (CT)- A computed tomography (CT) scans may be used to check for kidney stones or other obstructions. Blood Cultures- If symptoms are severe; the doctor will order blood cultures to determine if the infection is in the bloodstream and threatening other parts of the body.
- 14. Management of UTIs typically involves pharmacologic therapy and patient education. The nurse teaches the patient about medication regimens and infection prevention measures. 1. Acute PharmacologicTherapy- a) Uncomplicated cases- single dose of administration, short course (3 to 4 days) regimens, or 7 to 10 days regimens. The antibacterial agent should be affordable and should have few adverse effects. Most cases are cured after 3 days of treatment.
- 15. Name of Drugs Details Cephalosporin or ampicillin/ aminoglycoside combination For 7 to 10 days for the treatment to be effective. Trimethoprim- sulfamethoxazole These are commonly used medicine. Ciprofloxacin(fluoroquinolone) It is often used as a first line drug because E. coli has developed resistance to ampicillin or amxicillin. Levofloxacin(fluoroquinolone) It is another fluoroquinolone, is a good choice for short term therapy for uncomplicated, mild to moderate UTIs. Nitrofurantion It should not be used in patients with renal insufficiency because it is ineffective at glomerular filtration rates of less than 50ml/min and may cause peripheral neuropathy. Phenazopyridine It is a urinary analgesic may be prescribed to relieve the discomfort associated with the infection. b) Complicated cases-
- 16. 2. LongTerm PharmacologicTherapy- Relapse of UTIs suggest that the source of bacteriuria may be the upper urinary tract or the initial treatment was inadequate or administered for a too short time. The women with recurrent UTIs may be instructed to begin treatment to her own whenever symptoms occur and to contact her health care provider only when symptoms persist, fever occurs, or the number of treatment episodes exeeds four in a 6 month period. If infection recurs after complete antimicrobial therapy another short course (3 to 4 days) of full dose antimicrobial therapy may be prescribed. After treatment and sterilization of urine low dose preventive therapy (trimethoprim with or without sulfamethoxazole) each night at bed time is often prescribed.
- 17. 3. Patient education- The following are measures that studies suggest may reduce the incidence of urinary tract infections. These may be appropriate for people, especially women, with recurrent infections: Do not delay urination when it is necessary. A high fluid intake is essential. Cleaning the urethral meatus (the opening of the urethra) after intercourse has been shown to be of some benefit; however, whether this is done with an antiseptic or a placebo ointment (an ointment containing no active ingredient) does not appear to matter. Drinking 250 to 500ml of cranberry juice daily and avoidance of bubble baths may also help. Often long courses of low-dose antibiotics are taken at night to help prevent otherwise unexplained cases of recurring cystitis.
- 18. ASSESSMENT History of signs and symptoms related to UTIs is obtained from the patient with suspected UTI. The presence of pain, frequency, urgency and hesitancy and changes in urine are assessed, documented and reported. Patient’s knowledge about prescribed antibacterial medications and preventive health care measures is also assessed.
- 19. 1. NURSING DIAGNOSIS Acute pain related to infection within the urinary tract as manifested by pain on urination, suprapubic pain and bladder spasms. GOAL Pain and discomfort will be relieved. INTERVENTION Assess the onset, duration and level of pain. Provide analgesic drugs. Provide comfortable position. Reassure and provide divertional therapy. Give psychological support. Alert patient that phenazopyridine will color urine orange. Apply heating pad to painful area. EVALUATION Reports relief of pain.
- 20. 2. NURSING DIAGNOSIS Impaired urinary elimination related to UTIs as manifested by urgency, frequency, incontinence or hematuria and verbalization of concern over altered elimination pattern. GOAL Normal urination pattern will be returned. INTERVENTION Assess for changes in usual voiding pattern. Instruct patient regarding reason for symptoms. Encourage high fluid intake or administer IV fluid as ordered. Obtain urine for culture and sensitivity. Administer antimicrobial medications as ordered. Instruct patient about good perineal care and cleansing after each bowel movement. Tell patient to observe urine for color, odor,amount and frequency. EVALUATION Exhibits normal urination pattern.
- 21. 3. NURSING DIAGNOSIS Hyperthermia related to infection as manifested by elevation in temperature, tachycardia, chills and malaise GOAL Normal body temperature will be returned. INTERVENTION Assess vital signs 2-4 hourly. Administer antipyretics and antibiotics as ordered. Ensure hydration via oral or IV route. Monitor intake and output. Cover patient and keep him dry. Provide cooling sponge baths or compresses. EVALUATION Reports return of normal temperature.
- 22. 4. NURSING DIAGNOSIS Risk for reinfection related to lack of knowledge regarding measure to prevent recurrence. GOAL Signs of infection will not be present. INTERVENTION Assess the signs and symptoms of infection. Explain importance of taking all the antibiotics as prescribed. Symptoms will improve after 1-2 days of therapy, but organisms may still be present. Instruct the patient on appropriate hygiene, including- Careful cleansing of perineal region. Wiping from front to back after urinating. Cleansing with soap and water after each bowel movement. Explain the emptying of bladder before and after intercourse. Instruct the patient to urinate when the urge occurs or at least 2-4 hour during the day. Instruct the patient about the need to maintain adequate fluid intake. Advise patient to report symptoms or signs of recurrent UTI. EVALUATION Improves knowledge level of patient.
