Osteoporosis
•
2 recomendaciones•95 vistas
Osteoporosis is a disease where bone density decreases to the point of potential fracture. It occurs when bone resorption exceeds bone formation, resulting in porous and fragile bones. Key factors that increase the risk include low estrogen after menopause, physical inactivity, glucocorticoid use, and older age. Treatment focuses on preventing further bone loss with bisphosphonates or drugs that inhibit bone resorbing cells like denosumab.
Denunciar
Compartir
Denunciar
Compartir
Descargar para leer sin conexión
Recomendados
Más contenido relacionado
La actualidad más candente
La actualidad más candente (20)
Factors that increase & decrease risk of aging

Factors that increase & decrease risk of aging
Bone physiology, OSTEOPOROSIS, Pagets Disease, Hyperparathyoidism

Bone physiology, OSTEOPOROSIS, Pagets Disease, Hyperparathyoidism
Similar a Osteoporosis
Similar a Osteoporosis (20)
Último
☑️░ 9630942363 ░ CALL GIRLS ░ VIP ░ ESCORT ░ SERVICES ░ AGENCY ░
9630942363 THE GENUINE ESCORT AGENCY VIP LUXURY CALL GIRLS
HIGH CLASS MODELS CALL GIRLS GENUINE ESCORT BOOK
BOOK APPOINTMENT - 9630942363 THE GENUINE ESCORT AGENCY
BEST VIP CALL GIRLS & ESCORTS SERVICE 9630942363 VIP CALL GIRLS ALL TYPE WOMEN AVAILABLE
INCALL & OUTCALL BOTH AVAILABLE BOOK NOW
9630942363 VIP GENUINE INDEPENDENT ESCORT AGENCY
VIP PRIVATE AUNTIES
BEAUTIFUL LOOKING HOT AND SEXT GIRLS AND PARTY TYPE GIRLS YOU WANT SERVICE THEN CALL THIS NUMBER 9630942363
ROOM ALSO PROVIDE HOME & HOTELS SERVICE
FULL SAFE AND SECURE WORK
WITHOUT CONDOMS, ORAL, SUCKING, LIP TO LIP, ANAL, BACK SHOTS, SEX 69, WITHOUT BLOWJOB AND MUCH MORE
FOR BOOKING
9630942363Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...

Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...GENUINE ESCORT AGENCY
Model Call Girl Services in Delhi reach out to us at 🔝 9953056974 🔝✔️✔️
Our agency presents a selection of young, charming call girls available for bookings at Oyo Hotels. Experience high-class escort services at pocket-friendly rates, with our female escorts exuding both beauty and a delightful personality, ready to meet your desires. Whether it's Housewives, College girls, Russian girls, Muslim girls, or any other preference, we offer a diverse range of options to cater to your tastes.
We provide both in-call and out-call services for your convenience. Our in-call location in Delhi ensures cleanliness, hygiene, and 100% safety, while our out-call services offer doorstep delivery for added ease.
We value your time and money, hence we kindly request pic collectors, time-passers, and bargain hunters to refrain from contacting us.
Our services feature various packages at competitive rates:
One shot: ₹2000/in-call, ₹5000/out-call
Two shots with one girl: ₹3500/in-call, ₹6000/out-call
Body to body massage with sex: ₹3000/in-call
Full night for one person: ₹7000/in-call, ₹10000/out-call
Full night for more than 1 person: Contact us at 🔝 9953056974 🔝. for details
Operating 24/7, we serve various locations in Delhi, including Green Park, Lajpat Nagar, Saket, and Hauz Khas near metro stations.
For premium call girl services in Delhi 🔝 9953056974 🔝. Thank you for considering us!Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X79953056974 Low Rate Call Girls In Saket, Delhi NCR
☑️░ 9630942363 ░ CALL GIRLS ░ VIP ░ ESCORT ░ SERVICES ░ AGENCY ░
9630942363 THE GENUINE ESCORT AGENCY VIP LUXURY CALL GIRLS
HIGH CLASS MODELS CALL GIRLS GENUINE ESCORT BOOK
BOOK APPOINTMENT - 9630942363 THE GENUINE ESCORT AGENCY
BEST VIP CALL GIRLS & ESCORTS SERVICE 9630942363 VIP CALL GIRLS ALL TYPE WOMEN AVAILABLE
INCALL & OUTCALL BOTH AVAILABLE BOOK NOW
9630942363 VIP GENUINE INDEPENDENT ESCORT AGENCY
VIP PRIVATE AUNTIES
BEAUTIFUL LOOKING HOT AND SEXT GIRLS AND PARTY TYPE GIRLS YOU WANT SERVICE THEN CALL THIS NUMBER 9630942363
ROOM ALSO PROVIDE HOME & HOTELS SERVICE
FULL SAFE AND SECURE WORK
WITHOUT CONDOMS, ORAL, SUCKING, LIP TO LIP, ANAL, BACK SHOTS, SEX 69, WITHOUT BLOWJOB AND MUCH MORE
FOR BOOKING
9630942363Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...

Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...GENUINE ESCORT AGENCY
Último (20)
Call Girls Service Jaipur {9521753030} ❤️VVIP RIDDHI Call Girl in Jaipur Raja...

Call Girls Service Jaipur {9521753030} ❤️VVIP RIDDHI Call Girl in Jaipur Raja...
Call Girls Vadodara Just Call 8617370543 Top Class Call Girl Service Available

Call Girls Vadodara Just Call 8617370543 Top Class Call Girl Service Available
Best Rate (Guwahati ) Call Girls Guwahati ⟟ 8617370543 ⟟ High Class Call Girl...

Best Rate (Guwahati ) Call Girls Guwahati ⟟ 8617370543 ⟟ High Class Call Girl...
Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...

Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7
Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available
Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...

Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...
Night 7k to 12k Navi Mumbai Call Girl Photo 👉 BOOK NOW 9833363713 👈 ♀️ night ...

Night 7k to 12k Navi Mumbai Call Girl Photo 👉 BOOK NOW 9833363713 👈 ♀️ night ...
Call Girls Raipur Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Raipur Just Call 9630942363 Top Class Call Girl Service Available
Best Rate (Patna ) Call Girls Patna ⟟ 8617370543 ⟟ High Class Call Girl In 5 ...

Best Rate (Patna ) Call Girls Patna ⟟ 8617370543 ⟟ High Class Call Girl In 5 ...
The Most Attractive Hyderabad Call Girls Kothapet 𖠋 9332606886 𖠋 Will You Mis...

The Most Attractive Hyderabad Call Girls Kothapet 𖠋 9332606886 𖠋 Will You Mis...
Call Girls Visakhapatnam Just Call 8250077686 Top Class Call Girl Service Ava...

Call Girls Visakhapatnam Just Call 8250077686 Top Class Call Girl Service Ava...
Premium Call Girls In Jaipur {8445551418} ❤️VVIP SEEMA Call Girl in Jaipur Ra...

Premium Call Girls In Jaipur {8445551418} ❤️VVIP SEEMA Call Girl in Jaipur Ra...
Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available
VIP Hyderabad Call Girls Bahadurpally 7877925207 ₹5000 To 25K With AC Room 💚😋

VIP Hyderabad Call Girls Bahadurpally 7877925207 ₹5000 To 25K With AC Room 💚😋
Top Rated Bangalore Call Girls Ramamurthy Nagar ⟟ 9332606886 ⟟ Call Me For G...

Top Rated Bangalore Call Girls Ramamurthy Nagar ⟟ 9332606886 ⟟ Call Me For G...
Top Rated Hyderabad Call Girls Erragadda ⟟ 9332606886 ⟟ Call Me For Genuine ...

Top Rated Hyderabad Call Girls Erragadda ⟟ 9332606886 ⟟ Call Me For Genuine ...
Call Girls Kakinada Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Kakinada Just Call 9907093804 Top Class Call Girl Service Available
Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...

Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...
All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...

All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...
Osteoporosis
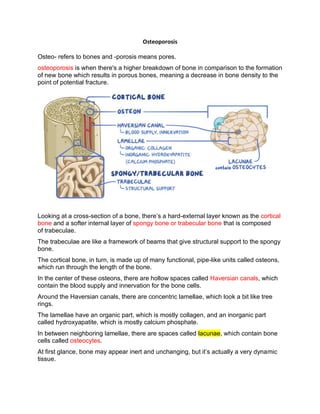
- 1. Osteoporosis Osteo- refers to bones and -porosis means pores. osteoporosis is when there's a higher breakdown of bone in comparison to the formation of new bone which results in porous bones, meaning a decrease in bone density to the point of potential fracture. Looking at a cross-section of a bone, there’s a hard-external layer known as the cortical bone and a softer internal layer of spongy bone or trabecular bone that is composed of trabeculae. The trabeculae are like a framework of beams that give structural support to the spongy bone. The cortical bone, in turn, is made up of many functional, pipe-like units called osteons, which run through the length of the bone. In the center of these osteons, there are hollow spaces called Haversian canals, which contain the blood supply and innervation for the bone cells. Around the Haversian canals, there are concentric lamellae, which look a bit like tree rings. The lamellae have an organic part, which is mostly collagen, and an inorganic part called hydroxyapatite, which is mostly calcium phosphate. In between neighboring lamellae, there are spaces called lacunae, which contain bone cells called osteocytes. At first glance, bone may appear inert and unchanging, but it’s actually a very dynamic tissue.
- 2. spongy bone is replaced every 3 to 4 years and compact bone is replaced every 10 years, in a process called bone remodeling which has two steps: - bone resorption when specialized cells called osteoclasts break down bone - bone formation which is when another type of cells called osteoblasts form new bone. Bone remodelling as a whole is highly dependent on serum calcium levels, which, in turn, are kept in the normal range by a balance between parathyroid hormone, or PTH, calcitonin and vitamin D. 1. Parathyroid hormone is produced by the parathyroid glands in response to low serum calcium, and it increases bone resorption to release calcium into the bloodstream. 2. calcitonin is produced by the thyroid gland in response to high serum calcium, so it opposes the action of PTH - therefore promoting bone formation and decreasing bone resorption. 3. vitamin D promotes calcium absorption in the gut, so it increases serum calcium, promoting bone formation and decreasing bone resorption. The balance between these regulatory factors results in a peak bone mass, usually by age 20 to 29 - and this usually occurs earlier in females than in males.
- 3. strength training increases peak bone mass, as well as hormones like estrogens and androgens that inhibit bone resorption. In osteoporosis osteoclasts break down bone faster than the osteoblasts can rebuild, it results in the lowering of the bone mass and eventually. These bone changes increase the risk of fracture, and they are known as fragility or pathologic fractures. Some bones like the vertebrae, shoulder blades, and ribs consist mainly of spongy bone, so they are in great risk of fragility fractures. Factors that accelerate bone mass loss and increase the risk of osteoporosis are : 1. low estrogen levels after menopause 2. low serum calcium. 3. alcohol consumption 4. smoking 5. drugs like glucocorticoids which decrease calcium absorption from the gut through antagonism of vitamin D 6. drugs like heparin and L-thyroxine. 7. physical inactivity, as seen in astronauts in a zero-gravity environment where they just don't use their musculoskeletal system as hard as when they’re on earth.As a result, bone deposition decreases due to a lack of stress, while resorption increases. 8. Turner syndrome, hyperprolactinemia, Klinefelter syndrome, Cushing syndrome, and diabetes mellitus.
- 4. the two most common types of osteoporosis are postmenopausal osteoporosis and senile osteoporosis. -postmenopausal osteoporosis, decreased estrogen levels lead to increased bone resorption. -senile osteoporosis, on the other hand, it’s believed that osteoblasts just gradually lose the ability to form bone, while the osteoclasts keep doing their thing unabated.bone resorption usually overtakes bone formation around the 8th decade of life. People with osteoporosis don’t usually have symptoms until a fracture occurs. The most common type of fractures are vertebral fractures, also known as compression fractures, and it occurs when one or more bones in the spine weaken and shatter. Vertebral fractures cause back pain, height loss, and a hunched posture. Femoral neck fractures and distal radius fractures can also occur, and they’re often associated with postmenopausal osteoporosis. Osteoporosis is usually diagnosed with a dual-energy X-ray absorptiometry or DEXA scan which tests for bone density. The test compares an individual's bone density to that of a normal adult which yields the result or the T score. A T score less than or equal to -2.5 is diagnostic of osteoporosis.
- 5. Treatment for osteoporosis usually relies on bisphosphonate drugs like alendronate and risedronate. If osteoporosis is really advanced, teriparatide, a recombinant parathyroid hormone can be used. Now, even though parathyroid hormone stimulates bone resorption, it’s been found that intermittent injections with teriparatide activates osteoblasts more than osteoclasts, therefore increasing bone formation. Interestingly, a thiazide diuretic like Hydrochlorothiazide can be used to treat osteoporosis as well. Hydrochlorothiazide boosts calcium retention in the kidney and directly stimulates osteoblast differentiation, therefore decreasing mineral bone loss. Finally, medications like denosumab, which is a monoclonal antibody that inhibits osteoclasts, and raloxifene, which is a selective estrogen receptor modulator, can be used for postmenopausal osteoporosis.