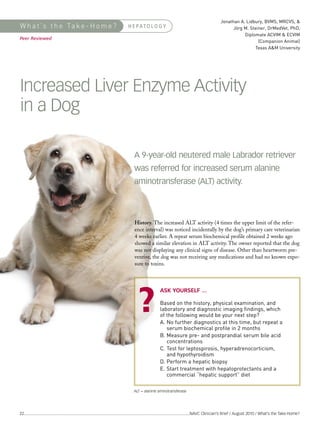
Increased liver enzyme activity in a dog
- 1. Jonathan A. Lidbury, BVMS, MRCVS, & Jörg M. Steiner, DrMedVet, PhD, Diplomate ACVIM & ECVIM (Companion Animal) Texas A&M University W h a t ’s t h e Ta k e - H o m e ? H E PATO L O G Y Peer Reviewed Increased Liver Enzyme Activity in a Dog Based on the history, physical examination, and laboratory and diagnostic imaging findings, which of the following would be your next step? A. No further diagnostics at this time, but repeat a serum biochemical profile in 2 months A 9-year-old neutered male Labrador retriever B. Measure pre- and postprandial serum bile acid concentrations was referred for increased serum alanine C. Test for leptospirosis, hyperadrenocorticism, and hypothyroidism aminotransferase (ALT) activity. D. Perform a hepatic biopsy E. Start treatment with hepatoprotectants and a commercial “hepatic support” diet History. The increased ALT activity (4 times the upper limit of the refer- ence interval) was noticed incidentally by the dog’s primary care veterinarian 4 weeks earlier. A repeat serum biochemical profile obtained 2 weeks ago showed a similar elevation in ALT activity. The owner reported that the dog was not displaying any clinical signs of disease. Other than heartworm pre- ventive, the dog was not receiving any medications and had no known expo- sure to toxins. ASK YOURSELF ... ALT = alanine aminotransferase 22 ...........................................................................................................................................................NAVC Clinician’s Brief / August 2010 / What’s the Take-Home?
- 2. Glucose (mg/dL) 106 60–135 Cholesterol (mg/dL) 242 120–247 BUN (mg/dL) 13 5–29 Creatinine (mg/dL) 0.9 0.3–2 Magnesium (mg/dL) 1.8 1.7–2.1 Physical Examination. The patient was showed an ALT activity of 584 U/L judged to be overweight (body condition (reference interval, 10–130 U/L). Urinal- Total calcium (mg/dL) 9.9 9.3–11.8 score of 7/9). Moderate dental calculus ysis results were within normal limits. Phosphate (mg/dL) 3.7 2.9–6.2 was noted on oral examination and bila- Total protein (g/dL) 6.3 5.7–7.8 terial ceruminous discharge was noted Diagnostic Imaging. An abdominal on otic examination. No other abnor- ultrasound examination showed gastric Albumin (g/dL) 2.9 2.4–3.6 malities were found. distension but no other significant find- Globulin (g/dL) 3.4 1.7–3.8 ings. No changes of the liver or biliary ALT (U/L) 584 10–130 Laboratory Results. The results of a system were observed. ALP (U/L) 145 24–147 complete blood count and blood smear examination were unremarkable. A GGT (U/L) 9 0–25 serum biochemical profile (Table 1) CONTINUES Total bilirubin (mmol/L) 0.3 0–0.8 Sodium (mmol/L) 144 139–147 Potassium (mmol/L) 3.9 3.3–4.6 Chloride (mmol/L) 115 107–116 Table 1. Serum Biochemical Profile Results Variable Result Reference Interval ALP = serum alkaline phosphatase; ALT = serum alanine aminotransferase; BUN = blood urea nitrogen; GGT = gamma glutamyltransferase What’s the Take-Home? / NAVC Clinician’s Brief / August 2010..........................................................................................................................................................23
- 3. W h a t ’s t h e Ta k e - H o m e ? CONTINUED • Inflammatory (acute hepatitis, chronic hepatitis, lobular dissecting hepatitis, copper hepatopathy) • Neoplasia (primary, metastatic) CORRECT ANSWER: Diagnostics. Because the liver has a considerable • Infectious (leptospirosis, infectious canine hepatitis, D. PERFORM A HEPATIC BIOPSY reserve capacity, patients with liver disease can toxoplasmosis, Heterobilharzia infection) have normal liver function test results.2 The • Trauma (contusions, herniation, torsion) ALT activity is a marker for hepatocellular dam- results of the dog’s serum biochemical profile did • Hyperplastic hepatic nodules age (Table 2). While serum alkaline phosphatase not suggest hepatic insufficiency. Paired pre- and activity may be increased due to a number of postprandial serum bile acid measurement is sen- extrahepatic conditions, increased serum ALT sitive and specific for detecting hepatic insuffi- • Endocrine disease (diabetes mellitus, hyperadrenocorticism, activity is considered to be a more specific ciency in dogs. However, in this case, serum bile adrenal hyperplasia) marker for hepatobiliary disease.1 This patient acid measurement would not have aided in diag- • Inflammatory (enteritis, pancreatitis, peritonitis, systemic had ALT activity level greater than 4 times the nosis or therapy selection. inflammatory response syndrome, sepsis) upper limit of the reference interval, and this ele- • Hypoxia (anemia, thromboembolic disease, congestive heart vation persisted for more than 4 weeks. This Abdominal ultrasound is a useful imaging modal- failure, circulatory shock) finding suggested clinically important hepatobil- ity for evaluation of the hepatobiliary system. • Anaphylaxis iary disease and warranted further investigation. However, clinicians must recognize that patients • Metabolic (storage diseases) may have clinically important hepatic parenchy- mal disease despite an apparently normal liver and biliary tract on abdominal ultrasonography.3 • Drug toxicity (barbiturates, carprofen, antimicrobials, azathioprine, glucocorticoids, griseofulvin, ketoconazole) Table 2. Causes of Increased Serum ALT • Toxic (heavy metals, copper, carbon tetrachloride, Extrahepatic Disease. Because of the liver’s cen- Activities in Dogs petrochemicals, mycotoxins, blue-green algae, sago palm) tral role in metabolism and its unique dual blood supply, it is often affected by extrahepatic disease. Primary Hepatopathies Hepatopathies can be the primary disease process • Severe muscle injury (uncommon) or can be secondary to extrahepatic disease, drugs, or toxins.4 The diagnostic and therapeutic approach for patients with primary and secondary hepatopathies differs greatly. Based on the signal- ment, history, physical examination, and clinico- pathologic findings, there was no evidence that this dog had extrahepatic disease or exposure to xenobiotics. Consequently, extensive testing for Secondary Hepatopathies extrahepatic disease was not indicated. Hepatic Biopsy. Collection of a hepatic biopsy was indicated due to the strong suspicion of a chronic primary hepatopathy. No evidence of a coagulopathy was found on a coagulation profile (including prothrombin time and activated partial thromboplastin time) or a buccal mucosal bleed- ing time. Xenobiotic-Related Causes Seven hepatic wedge biopsies were collected laparoscopically (Figure 1). Six of these were submitted for histopathology, and one specimen was immediately frozen. In addition, bile was submitted for aerobic and anaerobic culture. Extrahepatic Sources of ALT The frozen specimen was submitted for copper ALT = alanine aminotransferase 24 ...........................................................................................................................................................NAVC Clinician’s Brief / August 2010 / What’s the Take-Home?
- 4. • Depending on magnitude and duration, increases of serum ALT activity are clinically important and warrant further investigation.* • Hepatic function tests can be TX AT A GLANCE normal in patients with early quantification by flame atomic absorption Treatment. The patient was switched to chronic hepatitis. spectrometry (Colorado State University a commercial hepatic support diet with a • Treatment should be • Abdominal ultrasound exam- Veterinary Diagnostic Laboratories; vegetable protein source, restricted cop- started as early as ination can be unremarkable possible in the course of in patients with chronic dlab.colostate.edu). per content, and increased zinc content.5 chronic hepatitis. hepatic parenchymal disease. Supportive treatment with ursodiol and • Treatment should be • Increases in serum hepatic Diagnosis. Histopathologic evaluation of SAMe was initiated. The patient’s guided by hepatic enzyme activities can be from the liver biopsy specimens showed chronic hepatic copper accumulation was treated histopathology, hepatic extrahepatic sources (eg, periportal hepatitis with bridging fibrosis. with D-penicillamine.6 copper quantification, and alkaline phosphatase can be Copper-staining showed accumulation of bile/liver culture. of hepatic or bone origin) or copper in hepatocytes (Figure 2). The See Aids & Resources, back page, for • Chelating agents and due to primary or secondary hepatic copper concentration was 1651 references and suggested reading. reduced dietary copper hepatopathies. ppm dry weight (reference interval, intake are the main • Biopsy is indicated in patients 120–400 ppm). The final diagnosis was treatments for copper- that are suspected of having associated chronic chronic primary hepatopathy. copper-associated chronic hepatitis. hepatitis. • Hepatoprotectants have a place in the treatment of copper-associated chronic hepatitis. TAKE-HOME MESSAGES • The use of corticosteroids and other antiinflamma- * In our opinion, further investigation is tory drugs in the treatment warranted when a single ALT activity determination is greater than 5 times of copper-associated the upper limit of the reference inter- chronic hepatitis is val, or when multiple determinations controversial. 1 demonstrate activity greater than 2 • Assessment of the times the upper limit of the reference interval for more than 4 weeks. Laparoscopic view of the liver; patient’s response to biopsy sites are visible on the margin of the liver treatment is crucial. 2 Copper-associated chronic hepatitis; this histopathologic section shows abundant copper granules in the cytoplasm of periportal hepatocytes and in some hepatocytes Rhodamine stain; original magnification, 40x SAMe = s-adenosylmethionine What’s the Take-Home? / NAVC Clinician’s Brief / August 2010...........................................................................................................................................................25
