Spinal cord injury_040036.pptx
•Descargar como PPTX, PDF•
0 recomendaciones•91 vistas
Neurological disorder
Denunciar
Compartir
Denunciar
Compartir
Recomendados
Recomendados
Más contenido relacionado
La actualidad más candente
La actualidad más candente (20)
Similar a Spinal cord injury_040036.pptx
Similar a Spinal cord injury_040036.pptx (20)
Cervical spine trauma and spinal cord injuries by Dr Shamavu Gabriel.pptx

Cervical spine trauma and spinal cord injuries by Dr Shamavu Gabriel.pptx
CORD COMPRESSION SYNDROME by DR. CHUKWUMA O.N. G. Department of Internal Medi...

CORD COMPRESSION SYNDROME by DR. CHUKWUMA O.N. G. Department of Internal Medi...
Más de ShubhrimaKhan
Más de ShubhrimaKhan (20)
Plural effusion, PE & lung abscess, pneumothorax_014402.pptx

Plural effusion, PE & lung abscess, pneumothorax_014402.pptx
Gatekeeper training programme on mental health royal college of nursing.pptx

Gatekeeper training programme on mental health royal college of nursing.pptx
Último
Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls
(๏ 人 ๏) Punjab Call Girls provide you with erotic massage therapy
Punjab Call Girls are well-trained in courtship and seduction. They can offer you true love and companionship. They can also. They can help you forget your problems and frustrations. They are also experts in playing several roles.
( • )( • )ԅ(≖⌣≖ԅ) Call Girls Punjab is also available for special occasions. They can take you to business meetings or business tours. They can also take you to public functions or any special occasion. These ladies are ready to serve their clients with care and respect. They have a wide range of experience and can also offer customized services. College Call Girls Punjab These websites can help you find escorts in your area. You can also find reviews about them and get recommendations. Their expertise allows them to reach the sensational areas of a man's body and release feelings more intensely with touches and adult words.
You can full your all deserts with Punjab Call Girls
Punjab Call Girls you can find the best escort girls to meet your sexual desires. There are many options, from cute college girls to sexy models. However, you should be careful when choosing an escort service because some will not offer quality services.
Independent Call Girls Punjab will offer companionship services in addition to their sexual services. They can also accompany you to dinner or other social events. In addition, some escorts will perform intimate massages to increase your sensual pleasure another option is to hire a hot Russian escort. These girls are not only beautiful but also very talented in sex. In addition to orgasm, they can offer various erotic positions.
These sexy babes are a perfect choice for a sexy night in town. They know all the sexy positions and will make you moan in delight. They can also play with your dick in the deep throat position and lick it like ice cream. There are plenty of Call girls in Punjab who are available for one-night stands. Just make sure that you use a trusted site and read reviews before booking. You can find a wide variety of gorgeous call girls in our city on the internet. These websites offer a safe and convenient way to meet a woman and enjoy her company for a night of fun. These sites typically offer a photo of the girl and her number. You can contact her through the phone or sexing to arrange a rendezvous.
★OUR BEST SERVICES: - FOR BOOKING A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)
★ Spending time in my rooms
★ BJ (Blowjob Without a Condom)
★ COF (Come On Face)
★ Completion
★ (Oral to completion) bjnonCovered
★ Special Massage
★ O-Level (Oral sex)
★ Blow Job;
★ Oral sex with a noncondom)
★ COB (Come On Body)Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls

Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls@Chandigarh #call #Girls 9053900678 @Call #Girls in @Punjab 9053900678
Último (20)
Call Girl in Bangalore 9632137771 {LowPrice} ❤️ (Navya) Bangalore Call Girls ...

Call Girl in Bangalore 9632137771 {LowPrice} ❤️ (Navya) Bangalore Call Girls ...
Call Girls Service Mohali {7435815124} ❤️VVIP PALAK Call Girl in Mohali Punjab

Call Girls Service Mohali {7435815124} ❤️VVIP PALAK Call Girl in Mohali Punjab
Sexy Call Girl Dharmapuri Arshi 💚9058824046💚 Dharmapuri Escort Service

Sexy Call Girl Dharmapuri Arshi 💚9058824046💚 Dharmapuri Escort Service
Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls

Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls
Patna Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Patna Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Gorgeous Call Girls Mohali {7435815124} ❤️VVIP ANGEL Call Girls in Mohali Punjab

Gorgeous Call Girls Mohali {7435815124} ❤️VVIP ANGEL Call Girls in Mohali Punjab
Ernakulam Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Ernakulam Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
kozhikode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

kozhikode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Vip Call Girls Makarba 👙 6367187148 👙 Genuine WhatsApp Number for Real Meet

Vip Call Girls Makarba 👙 6367187148 👙 Genuine WhatsApp Number for Real Meet
Muzaffarpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Muzaffarpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
kochi Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

kochi Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
surat Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

surat Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Call Girl in Indore 8827247818 {Low Price}👉 Nitya Indore Call Girls * ITRG...

Call Girl in Indore 8827247818 {Low Price}👉 Nitya Indore Call Girls * ITRG...
Sangli Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Sangli Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Mangalore Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Mangalore Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Erode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Erode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Sambalpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Sambalpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
bhubaneswar Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

bhubaneswar Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
dhanbad Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

dhanbad Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Bareilly Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Bareilly Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Spinal cord injury_040036.pptx
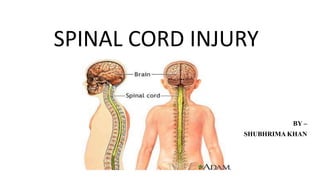
- 1. BY – SHUBHRIMA KHAN SPINAL CORD INJURY
- 2. • The spinal cord is a collection of nerves that travels from the bottom of the brain down to back. • There are 31 pairs of nerves that leave the spinal cord and go to arms, legs, chest and abdomen. • These nerves allow brain to give commands to the muscles and cause movements of the arms and legs. • The spinal cord is very sensitive to injury. Unlike other parts of body, the it does not have the ability to repair itself if it is damaged. INTRODUCTION
- 4. A spinal cord injury refers to any damage to the spinal cord either from trauma, loss of its normal blood supply, or compression from tumor or infection. DEFINITION
- 5. • Trauma: automobile or motor cycle accidents, gunshot or knife wounds, falls and sports mishaps • Weakened spine: rheumatoid arthritis or osteoporosis • Spinal stenosis: spinal canal protecting the spinal cord has become too narrow due to the normal aging process. • Vertebrae most commonly involved are the 5th, 6th and 7th cervical vertebrae, 12th thoracic vertebrae and 1st lumbar vertebrae. CAUSES AND RISK FACTORS
- 6. 1. Mechanism of injury • Flexion injury • Hyper extension injuries • Compression injuries • Flexion rotation injuries 2. Level of injury • Skeletal level • Neurologic level 3. Degree of injury • Complete cord injury • Incomplete cord injury CLASSIFICATION
- 7. Flexion injuries • Occurs when the head strikes the steering wheel, the spine is forced into acute hyper flexion • Rupture of posterior ligaments results in forward dislocation of the vertebrae • Cervical spine usually affected are the C5 to C6 level Mechanism of injury
- 8. Hyper extension injuries • Results after a fall in which the chin hits an object and the head is thrown back • Anterior ligament is ruptured with fracture of the posterior elements of the vertebral body • Greatest area of stress is at the C4 and C5 CONT..
- 10. Compression injuries • Caused by falls or jumps in which the person lands directly on the head, sacrum or feet • Force of impact fractures the vertebrae and the fragments compress the cord • Lumbar and lower thoracic vertebrae are usually affected CONT..
- 11. Flexion rotation injuries • Most unstable because ligaments that stabilize the spine are torn. • Rupture of the posterior ligament with displacement of the vertebral body. • This injury most often contributes to the several neurologic deficits. CONT..
- 13. Skeletal level • Skeletal level of injury is the vertebral level with the most damage to the vertebral bones and ligaments. Neurologic level • Lowest segment of the spinal cord with normal sensory or motor function on both the side of the body. Level of injury
- 14. • Level of injury may be cervical, thoracic, lumbar or sacral. • Cervical and lumber injuries are most common because they are associated with the greatest flexibility and movement. • Involvement of cervical cord = paralysis of all four extremities (quadriplegia). • Involvement of thoracic, lumbar or sacral cord = paralysis of lower extremities (paraplegia). • The degree of impairment of arms depends on the level of injury, the lower the level, more function is retained in the arms. CONT..
- 16. • Complete cord injury: Results in total loss of sensory and motor function below the level of injury. • Incomplete cord injury: mixed loss of voluntary motor activity and sensation and leaves some tracts intact. Central cord syndrome Anterior cord syndrome Brown sequard syndrome Conus medullaris and cauda equina syndrome Degree of injury
- 17. Central cord syndrome • Damage to central spinal cord • Occurs most commonly in the cervical region • Motor weakness and sensory loss are present in both upper and lower extremities CONT..
- 18. Anterior cord syndrome • Results from injury causing compression of anterior portion of the spinal cord. • Paralysis and loss of pain and temperature sensation below the level of injury • Sensation of touch, position and vibration remains intact. CONT..
- 19. Brown sequard syndrome • Result of damage to one half of the spinal cord (knife injury) • Ipsilateral paralysis with ipsilateral loss of motor function and pressure and contralateral loss of pain and temperature. CONT..
- 20. Conus medullaris and cauda equina syndrome • Result from damage to the very lowest portion of the spinal cord (conus) and the lumbar and sacral nerve roots (cauda equina). • Flaccid paralysis of the lower limbs and areflexia (flaccid bladder and bowel). CONT..
- 21. Respiratory system • Injury below the level of C4 diaphragmatic breathing hypoventilation • Cervical and thoracic injuries paralysis of abdominal and intercostal muscles patient cannot cough effectively to remove secretions atelectasis and pneumonia • Neurogenic pulmonary edema. CLINICAL MANIFESTATIONS
- 22. Cardio vascular system • Injury above the level of T6 decreases the influence of sympathetic nervous system bradycardia occurs peripheral vasodilation reduces return of blood to the heart Decreases cardiac output hypotension. CONT..
- 23. Urinary system • Urinary retention (loss of sensation and decreased reflexes) in acute SCI or spinal shock. • Neurogenic bladder (urgency, frequency, incontinence, inability to void, increase bladder pressure, reflux urine into kidney). CONT..
- 24. Gastrointestinal system • Injury above the level of T5 decreased gastro intestinal motility development of paralytic ileus and gastric distension • Development of stress ulcers • Intra abdominal bleeding • Less voluntary control over the bowel neurogenic bowel (bowel is areflexic and sphincter tone is decreased) CONT..
- 25. Problems with thermoregulation • Poikilothermism is lost in spinal cord injuries • Decreased ability to sweat or shiver below the level of the lesion • Patients with high cervical injury have a greater loss of ability to regulate temperature CONT..
- 26. Peripheral vascular problems • Deep vein thrombosis (during the first 3 months), if remain unrecognized , leading to pulmonary embolism which is the leading cause od death. CONT..
- 27. Spinal shock • Temporary loss of neurologic function characterized by decreased reflexes, loss of sensation and flaccid paralysis below the level of injury. • Syndrome lasts days to months Neurogenic shock • Effects are associated with cervical or high thoracic injury • Due to loss of vasomotor tone caused by injury and is characterized by hypotension and bradycardia. • Peripheral vasodilation decreased cardiac output CONT..
- 28. DIAGNOSTIC EVALUATION History and physical examination X ray spine CT scan MRI scan Vertebral angiography: an x ray study of blood vessels suppling spine.
- 29. MANAGEMENT Initial care • Neck should be stabilized in a neutral position without flexion or extension • Place the affected person on a spine board and secure the spine with a hard collar around the neck
- 30. CONT.. • Log rolling technique • Maintain a patent airway • Mechanically assisted ventilation • patients with severe cervical injury, placed in skeletal traction
- 31. CONT.. Drug therapy • Methyl prednisolone (effective if given within 8 hours of injury) • Loading dose of 30mg/kg given within 3 hours of injury followed by 24 hours of 5.4mg/kg IV methyl prednisolone drip. • Vasopressor agents (dopamine) • Histamine 2 receptor blocking agents
- 32. CONT.. Managing respiratory dysfunction • If the injury is at or above C3 endotracheal intubation and mechanical ventilation. • Chest physiotherapy, adequate oxygenation and pain management • Use of incentive spirometry.
- 33. CONT.. Managing cardiovascular instability In case of bradycardia, administer anticholinergic (atropine) Hypotension managed with dopamine infusion Compression gradient stockings to prevent DVT If severe blood loss has occurred, blood should be administered according to protocol
- 34. CONT.. Fluid and nutritional balance • First 48 to 72 hours after SCI, GI tract may stop functioning (paralytic ileus) • NG tube insertion for gastric decompression • Introduce oral foods and fluids once the bowel sounds returns • In patients with high cervical injuries swallowing capacity must be evaluated • Increased dietary fiber
- 35. CONT.. Temperature control Monitor body temperature Monitor the environment closely to maintain appropriate temperature Patient should not be overloaded with covers or unduly exposed
- 36. CONT.. Managing stress ulcers Stool and gastric contents are tested daily for blood. Give corticosteroids along with antacids H2 receptor blockers or proton pump inhibitors
- 37. CONT.. Bladder and bowel management Insertion of indwelling catheter After patient is stabilized, start intermittent catheterization Suppository should be inserted daily Increased fiber intake
- 38. NURSING DIAGNOSIS • Ineffective breathing pattern related to weakness or paralysis of abdominal and intercostal muscles • Impaired physical mobility related to motor and sensory impairments • Disturbed sensory perception related to motor and sensory impairment • Impaired urinary elimination related to inability to void spontaneously • Constipation related to presence of atonic bowel • Risk for impaired skin integrity related to immobility
- 39. COMPLICATIONS Neurologic deterioration Pressure sores Pulmonary complications - Atelectasis - Increased work of breathing - Decrease cough retained secretions Pneumonia - Muscle fatigue Loss of circulatory control Muscle tone problems - Spastic and flaccid muscles depression.