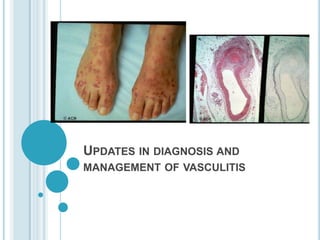
Vasculitis
- 1. UPDATES IN DIAGNOSIS AND MANAGEMENT OF VASCULITIS
- 2. OVERVIEW Basic facts Definition and Classification Patient perspective Management Evidence based recommendation Newer therapy Monitoring Complications Summary
- 3. VASCULITIS: BASIC FACTS • Vasculitis affects all ages, although some types are restricted to certain age groups • Vasculitis tends to affect Caucasians, although many African-Americans are affected • Vasculitis has a genetic component, but is not heritable • Vasculitis is a chronic relapsing disease, although some patients experience prolonged remission
- 5. VASCULITIS: DEFINITION Pathologist Inflammatory destruction of blood vessels • Infiltration of vessel wall with inflammatory cells – Leukocytoclasis – Elastic membrane disruption • Fibrinoid necrosis of the vessel wall • Ischemia, occlusion, thrombosis • Aneurysm formation • Rupture, hemorrhage Rheumatologist A clinicopathologic process characterized by inflammatory destruction of blood vessels that results in occlusion or destruction of the vessel and ischemia of the tissues supplied by that vessel.
- 6. VASCULITIS: CLASSIFICATION • Large-vessel vasculitis – Giant cell arteritis, Takayasu‟s arteritis – Behcet‟s disease, Cogan‟s syndrome • Medium-vessel vasculitis – Polyarteritis nodosa – Buerger‟s disease, Central nervous system vasculitis, Kawasaki‟s disease, Rheumatoid vasculitis • Small-vessel vasculitis – Wegener‟s, microscopic polyangiitis, Churg-Strauss – Cryoglobulinemic vasculitis, Henoch-Schönlein purpura,
- 7. VASCULITIS: CLASSIFICATION • Large-vessel vasculitis – Aorta and the great vessels (subclavian, carotid) – Claudication, blindness, stroke • Medium-vessel vasculitis – Arteries with muscular wall – Mononeuritis multiplex (wrist/foot drop), mesenteric ischemia, cutaneous ulcers • Small-vessel vasculitis – Capillaries, arterioles, venules – Palpable purpura, glomerulonephritis, pulmonary hemorrhage
- 8. ANCA-ASSOCIATED VASCULITIDES Wegener’s granulomatosis: granulomatous inflammation involving the respiratory tract and necrotizing vasculitis affecting small to medium- sized vessels Microscopic polyangiitis: Necrotizing vasculitis affecting the small vessels. Churg-Strauss Syndrome: Eosinophil-rich and granulomatous inflammation involving the medium- sized vessels, and associated with asthma and eosinophilia
- 9. Wegener‟s Churg- Strauss MPA Necrotizing Granuloma Hypereosinophilia •Sinusitis •Subglottic stenosis •Pulmonary nodules •Orbital pseudotumor •Asthma •Pulmonary infiltrates •Myocarditis •Pulmonary capillaritis •Glomerulonephritis •Sensory neuropathy •Mononeuritis multiplex
- 11. VASCULITIS: PATIENT PERSPECTIVE Herlyn K, Arthritis Rheum 2010; 659
- 12. VASCULITIS: PATIENT PERSPECTIVE Pain Disease-Specific • Sensory neuropathy • Cutaneous ulcerations • Arm claudication Non-specific • [Arthritis] • Vertebral fracture Fatigue Vasculitis-induced • Loss of proprioception Glucocorticoid-induced • Muscle loss, Weight gain • Emotional liability Immunosuppression-induced • Cognitive impairment • Drug-associated fatigue
- 13. MANAGEMENT
- 14. • Diagnosis of a systemic vasculitis is often a diagnosis of exclusion, based on recognition of the clinical syndrome – e.g. Churg-Strauss: adult onset asthma x 2 years, followed by atypical pneumonias, followed by peripheral nerve involvement • Biopsy of involved organ is the most straightforward method of establishing a diagnosis – Biopsy may be helpful to exclude infection/malignancy • Other tests may be suggestive, but not diagnostic – ESR, CRP – CT: pulmonary hemorrhage, cavitary lesions – Bronchoscopy: pulmonary hemorrhage (hemosiderosis) – Urinalysis: for patients with kidney vasculitis – ANCA (antineutrophil cytoplasmic antibodies) – Angiogram (including MRA, CT-angiogram) VASCULITIS: DIAGNOSIS
- 15. PRINCIPLES OF TREATMENT Identify drives Infection, drugs, malignancy Induce and maintain remission Minimise drug toxicity
- 16. • Remission induction: – Cyclophosphamide 2mg/kg po qd x 3-6 months [or 15 mg/kg IV q 2 wk x3 then q 3 weeks x 6-12 months] – Prednisone 1mg/kg po qd x 1 month, then taper – [Bactrim, Calcium, Vitamin D] • Remission maintenance (minimum 2 years) – Methotrexate 20-25 mg po q week + folate – Azathioprine 2mg/kg po qd – Mycophenolate mofetil 1.5 g po BID – Leflunomide 20-30 mg po BID VASCULITIS: TREATMENT
- 17. „STANDARD‟ THERAPY: „ADD-ON‟ THERAPY CYC ? improve effective + reduce toxicity IV methyl prednisolone Plasma exchange Intravenous immunoglobulin TNF blockade AZA/MTX 0 3 6 9 12 15 18 24 months Prednisolone CYC; cyclophosphamide, AZA; azathioprine, MTX; methotrexate
- 18. REDUCE CYCLOPHOSPHAMIDE EXPOSURE Switch to alternative on remission IV pulse instead of daily oral Alternative induction for non-severe disease 18
- 19. GENERALISED (CYCAZAREM) 80 95 5 0 25 50 75 100 percentage 3 months 6 months Died Jayne, N Engl J Med 2003 Time from remission to relapse (months) 1614121086420 Survival 1.0 .9 .8 .7 .6 Group Cyclophosphamide Azathioprine Remission Relapse Oral CYC + prednisolone Continued CYC vs. AZA
- 20. CYCLOPSde Groot et al, Ann Int Med 2009
- 21. Months from entry 20181614121086420 Survivaltofirstrelapse 1.0 .9 .8 .7 .6 .5 .4 .3 .2 .1 0.0 LIMB Cyclophosphamide Methotrexate Survivalto1strelapse EARLY SYSTEMIC (NORAM): METHOTREXATE (MTX) VS. CYCLOPHOSPHAMIDE (CYC) MTX CYC P = 0.02 EUVAS % 0 10 20 30 40 50 60 70 80 90 100 MTX CYC 91.5 95.5 Remission Relapse de Groot et al, Arthritis Rheum 2005
- 22. Generalised vasculitis – cyclophosphamide (3-6 months) Time (months) 183-60 Glomerularfiltrationrate(ml/min) 80 70 60 50 40 De Groot, ASN 2006 Jayne, New Eng J Med 2003 Time to remission Months from entry 181614121086420 1.0 .8 .6 .4 .2 0.0 LIMB Daily oral Pulse Time to remission, BVAS =0 Recovery of renal function
- 23. REMISSION MAINTENANCE Azathioprine ≅ methotrexate How long ? 23
- 24. LESS CYCLOPHOSPHAMIDE - INCREASES RELAPSE RISK
- 26. IMPROVE: CUMULATIVE INCIDENCE OF RELAPSE 0.000.250.500.751.00 0 1 2 3 4 5 Time (years) AZA MMF Hiemstra, Am Soc Nephrol 2009
- 28. EULAR RECOMMENDATIONS FOR CONDUCTING CLINICAL STUDIES AND/OR CLINICAL TRIALS IN SYSTEMIC VASCULITIS: FOCUS ON ANCA-ASSOCIATED VASCULITIS. For clinical trials or studies, patients with vasculitis should be categorised into clearly defined activity states. The following terms are recommended to use: remission, response, refractory disease and relapse Comprehensive disease assessment in vasculitis requires the recording of disease activity, damage and function. Use form of the Birmingham Vasculitis Activity Score, the Disease Extent Index, the Vasculitis Damage Index and the Short Form 36 Ann Rheum Dis. 2007;66:605-617.
- 29. Given the high mortality of untreated systemic vasculitis, the use of placebo must in general be restricted as an adjunct to standard therapy for induction treatment. Biomarkers such as CRP and/or ESR should be determined regularly as serologic markers of disease activity, but results must be interpreted in the context of the clinical findings.
- 30. EULAR RECOMMENDATIONS FOR THE MANAGEMENT OF PRIMARY SMALL AND MEDIUM VESSEL VASCULITIS. Anti-neutrophilic cytoplasmic antibody (ANCA) testing (including indirect immunofluorescence and ELISA) should be performed in the appropriate clinical context A positive biopsy is strongly supportive of vasculitis and should be performed to assist diagnosis and further evaluation for patients suspected of having vasculitis Use of a structured clinical assessment, urine analysis and other basic laboratory tests at each clinical visit for patients with vasculitis Ann Rheum Dis. 2008;68:310-317.
- 31. Combination of cyclophosphamide (intravenous or oral) and glucocorticoids for remission induction of generalised primary small and medium vessel vasculitis a combination of methotrexate (oral or parenteral) and glucocorticoid as a less toxic alternative to cyclophosphamide for the induction of remission in non-organ threatening or non- life threatening ANCA-associated vasculitis Use of high-dose glucocorticoids as an important part of remission induction therapy
- 32. Plasma exchange for selected patients with rapidly progressive severe renal disease in order to improve renal survival Remission-maintenance therapy with a combination of low- dose glucocorticoid therapy and, either azathioprine, leflunomide or methotrexate Use of antiviral therapy for the treatment of hepatitis C- associated cryoglobulinaemic vasculitis A combination of antiviral therapy, plasma exchange and glucocorticoids for hepatitis B-associated PAN
- 33. EULAR RECOMMENDATIONS FOR THE MANAGEMENT OF LARGE VESSEL VASCULITIS. A temporal artery biopsy should be performed whenever a diagnosis of giant cell arteritis is suspected, but this should not delay the treatment; a contralateral biopsy is not routinely indicated Early initiation of high-dose glucocorticoid therapy for induction of remission in large vessel vasculitis An immunosuppressive agent should be considered for use in large vessel vasculitis as adjunctive therapy Ann Rheum Dis. 2008;68:318-323.
- 34. Monitoring of therapy for large vessel vasculitis should be clinical and supported by measurement of inflammatory markers The use of low-dose aspirin in all patients with giant cell arteritis Reconstructive surgery for Takayasu arteritis should be performed in the quiescent phase of disease and should be undertaken at expert centres
- 35. NEWER THERAPY
- 36. NEWER THERAPIES, BIOLOGIC OR NON-BIOLOGIC ? IVIg Anti-TNF Rituximab ATG Alemtuzumab Abatacept Mycophenolic acid Mycophenolate mofetil (Cellcept) Enteric coated MPA (Myfortic) Leflunomide Deoxyspergualin
- 37. RITUXIMAB
- 38. RITUXIMAB FOR REFRACTORY VASCULITIS N = 63 Jones, Arthritis Rheum 2009
- 39. RITUXIMAB IN ENT/EYE DISEASE (N=32) Pre-RTX Post-RTX Martinez del Pero et al, Clin Otolaryngol 2009
- 40. RITUXIMAB - RANDOMISED TRIALS IN ANCA ASSOCIATED VASCULITIS RITUXVAS (EUVAS) New, with renal involvement N=44 12 month data reported 2008 RAVE (US) New/relapsing renal/non-renal N=197 6 month data reported 2009
- 41. RITUVAS - BASELINE CHARACTERISTICS RTX CYC Both Patients 33 11 44 Age 68 67 68 PR3/MPO-ANCA 20/13 5/6 25/19 GFR (ml/min/1.73m2) 25 15 21 Dialysis 24% 9% 20% Jones, New Engl J Med 2010
- 42. RITUXVAS – REMISSION (BVAS = 0 FOR 6 MONTHS) 0.000.250.500.751.00 0 100 200 300 400 Time (days) Cyclophosphamide Rituximab Jones, New Engl J Med 2010 RTX CYC Sustained remission 25/33 (76%) 9/11 (82%) No sustained remission 2 incomplete response 6 deaths 1 incomplete response 1 death Time to Remission
- 43. RITUXVAS – SAFETY RTX CYC SAEs 31 (42%) 1.0 /pat yr 12 (36%) 1.1 /pat yr Infections 21 (39%) 0.66/pat yr 7 (21%) 0.60/pat yr Death 6 (18%) 2 (18%) 0.000.250.500.751.00 ProportionFreeofSAE 0 50 100 150 200 250 300 350 Time (days) CYC RTX Time to first SAE Jones, New Engl J Med 2010
- 44. RELAPSE RTX N=33 CYC N=11 Relapse 7 (21%) 2 (18%) Major 1 (3%) 2 (18%) Minor 6 (18%) 0 (0%) Jones, ACR/ASN 2010
- 45. RAVE = US TRIAL
- 46. RAVE DESIGN 197 new (49%) or relapsing WG/MPA creatinine < 4.0mg/dl, no lung haemorrhage Randomised, double-blind rituximab 375mg/m2/wk x4 vs. oral CYC Primary end-point remission and steroid withdrawal at 6 months Stone J et al, N Engl J Med 2010
- 47. RAVE – REMISSION RATES * p=0.01 %patients p=ns p=ns Stone J et al, N Engl J Med 2010
- 48. RAVE RESULTS Efficacy Nephritis and alveolar haemorrhage similar response Safety Similar AE rates 18 month data end 2010 Stone J et al, N Engl J Med 2010
- 49. MONITORING
- 50. VASCULITIS: MONITORING • Large-vessel vasculitis – MRI/MRA chest/abdomen/pelvis every 6-12 months • Medium-vessel vasculitis – Mesenteric angiogram to assess disease activity – EMG/NCV to monitor nerve damage – Wound care for cutaneous ulcers • Small-vessel vasculitis – Chest CT every 6-12 months – Blood and urine tests every 1-4 weeks
- 51. COMPLICATIONS
- 52. VASCULITIS: LONG-TERM DAMAGE • Large-vessel vasculitis – Blindness, Stroke – Claudication: “Angina” of the arms • Medium-vessel vasculitis – Foot drop: inability to lift a foot – Wrist drop: inability to lift a hand – Cutaneous ulcerations • Small-vessel vasculitis – Oxygen dependence – Renal insufficiency/failure
- 56. SUMMARY
- 57. VASCULITIS: SUMMARY • The systemic vasculitides are chronic diseases, characterized by relapse and remission • Achieving remission requires intense monitoring by a multidisciplinary team with expertise in these diseases • Even after achieving disease remission, patients will continue to suffer from the chronic, irreversible consequences of both the disease and its therapies • Pain and fatigue are common consequences of vasculitis that are independent of disease activity and generally fail to respond to immunosuppression
- 58. Cyclophosphamide induction has been optimised Remission maintenance with AZA or MTX, MMF less effective Rituximab alternative to CYC and preferred for relapsing/refractory disease. ? Maintenance of remission after RTX
- 59. Thank you
Notas del editor
- Induction rates in this trial were high with oral cyclophosphamide and high dose oral glucocorticoids.
- Median creatinine at entry was 200 (GFR 48ml/min). Good recovery of renal function was observed.
- The primary endpoint of time to first relapse was evaluated using a COX proportional hazards regression model. Kaplan Meyer cumulative incidence curves show an early divergence which is maintained throughout the follow-up period, with more events occurring in the Azathioprine group. There were 187 patient years follow-up in the MMF group and 217 patient years in the AZA group, reflecting the higher relapse rate in the MMF group.The analysis was left-censored at the start of remission therapy, and right censored at relapse, death, end of follow-up, or withdrawal.
- We have conducted a retrospective registry review of 63 AAV patients treated with rituximab.