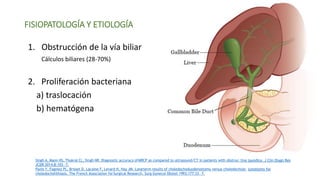
Este documento describe la fisiopatología, criterios diagnósticos, gravedad y tratamiento de la colecistitis aguda y la colangitis aguda. La colecistitis aguda se produce cuando hay inflamación de la vesícula biliar, generalmente debido a cálculos biliares. La colangitis aguda es una infección grave de la vía biliar, causada comúnmente por obstrucción de los conductos biliares y proliferación bacteriana. El diagnóstico se basa en criterios clínicos, de laboratorio e imagenológicos.