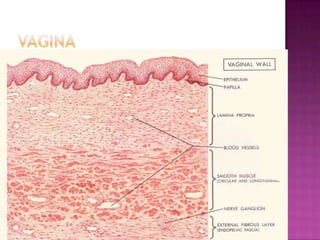
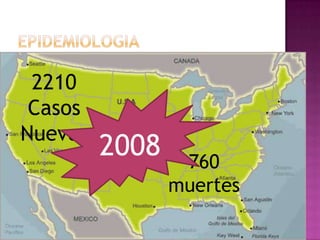
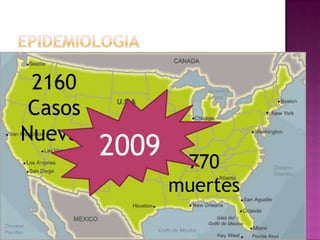
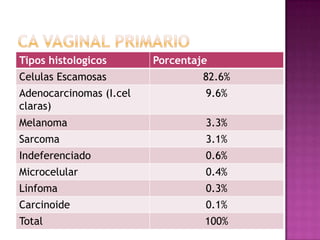
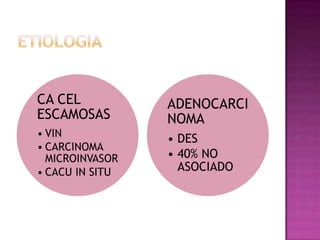
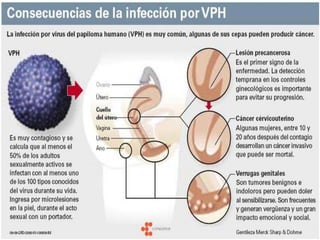
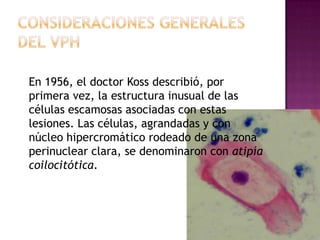
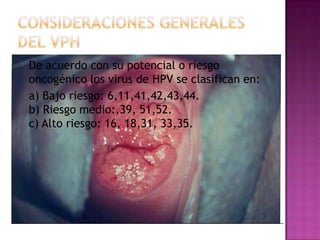
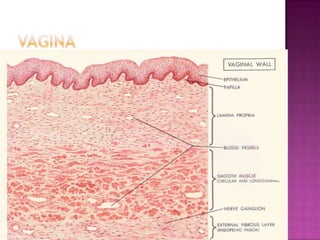
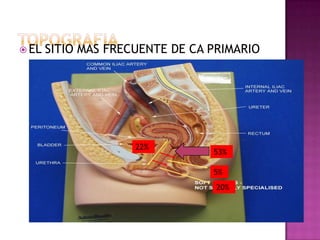
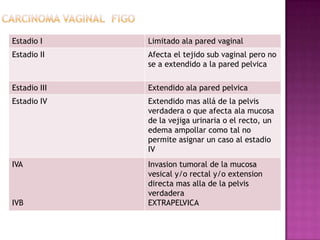
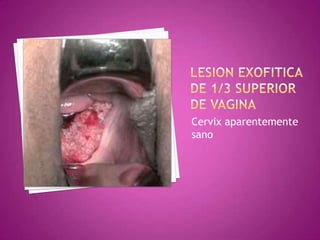
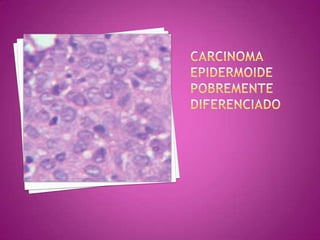
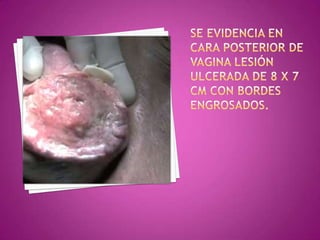
Este documento describe lesiones preinvasivas y canceres de vagina. Define hiperplasia, metaplasia y displasia como lesiones preinvasivas que pueden progresar a cáncer. Explica que la mayoría de cánceres de vagina son metastáticos de cáncer de cuello uterino o vulva, y que los virus del papiloma humano (VPH) causan alrededor del 90% de cánceres de vagina. Resume los síntomas, tipos histológicos, estadios y tratamientos de cáncer de vagina